I may receive a commission if you purchase through links in this post. I am not a doctor; please consult your practitioner before changing your supplement or healthcare regimen. As an Amazon Associate I earn from qualifying purchases.
This article is an introduction to the Vitamin A Detox diet, or Low Vitamin A Diet: What is it? And why does it show promise in improving liver health, leaky gut, autoimmune issues, mental health, hormone balancing, eye, lung, bladder, kidney, blood sugar, skin conditions and more?
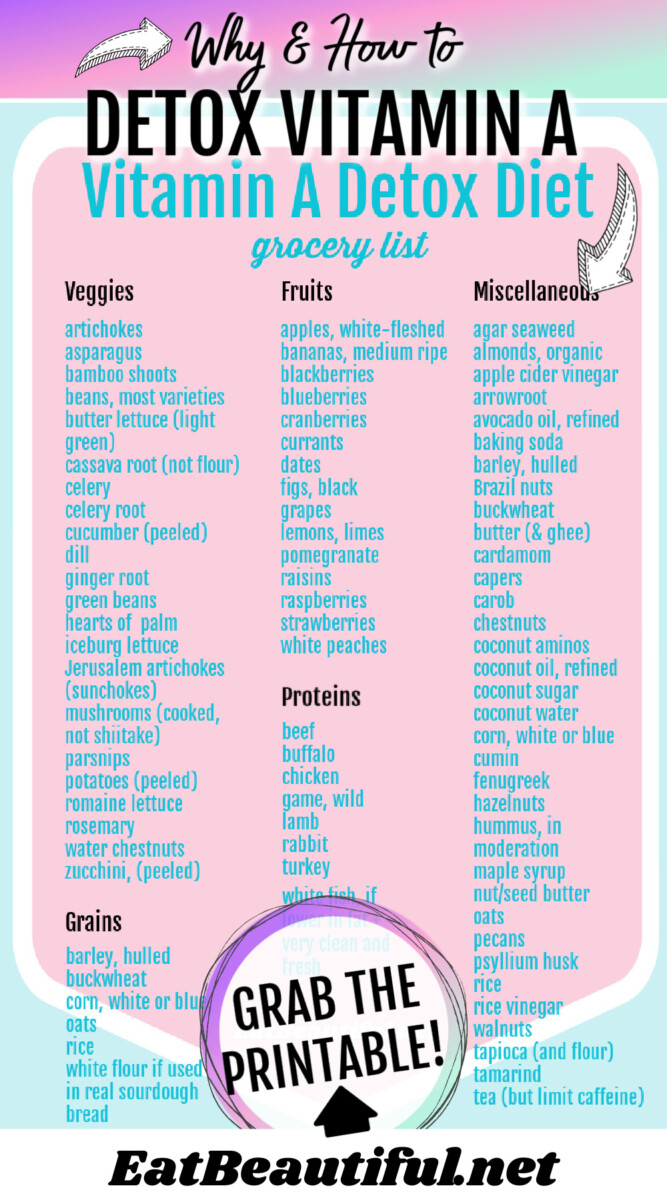
You’ll be able to consider and try the diet more easily with the food lists provided below. These free lists and printable grocery list designate which foods to avoid and which foods to eat more freely.
While doing a vitamin A elimination diet to reduce toxicity, it may be helpful to remember to eat with a calm, peaceful state of mind and a sense of freedom and enjoyment. We don’t benefit from added stress.
A background on vitamin A toxicity
What follows is a lengthy explanation of the vitamin A toxicity theory, which I intended to be brief by way of an introduction to the vitamin A food lists. Nonetheless, I found I had a lot to say and a lot of research to share. I hope you’ll benefit.
This concept was introduced several years ago by an engineer named Grant Genereux. He wrote a free e-book called Extinguishing the Fires of Hell. In 2017, he wrote a second free e-book, Poisoning for Profits. Grant’s research is thorough and has the potential to change the health of thousands, if not millions of people.
Those of us with tricky or frustrating health concerns are willing to try the vitamin A detox diet and be the first ones to see if Grant’s theory is right.
Full of scientific studies that informed his reasoning, Grant’s e-books are compelling to anyone willing to look at the studies and reconsider their formerly held set of nutritional beliefs.
The history of Vitamin A as a supplement
Grant discusses the historical introduction of Vitamin A as a supplement.
(Due to flaws in previous rodent studies, I look forward to sharing with you new rodent studies that are about to begin — research that could, in the long run, help overturn the FDA’s current nutritional guidelines for “vitamin” A.)
Grant’s books look at the corruption involved in making premature and incorrect conclusions about vitamin A’s benefits.
Grant discusses vitamin A’s role in the body:
… vitamin-A is a fat (lipid) soluble molecule. Therefore, it will naturally be absorbed (emulsified) by fats. This includes both dietary fats, and the body’s storage fats. For us, most of the storage of vitamin-A is in the fats within the liver, and to a lesser extent in the fats of the adipose tissues (the skin etc.) … As the liver becomes more and more saturated, more vitamin-A will remain in serum longer and slowly seep into and accumulate within the lipids of the adipose tissues. Even with that, the vitamin-A stored within these fats is not yet toxic … So, vitamin-A in reasonable amounts, given adequate amounts of dietary fats and proteins, is by itself not too terrible. However, there is a tipping point to where vitamin-A can, and does, easily convert into an extremely nasty, and highly toxic molecule (and the thought to be active form of the vitamin). This converted vitamin-A molecule is called retinoic acid.
Retinoic acid for chemotherapy
Grant goes on to explain that retinoic acid is used as a chemotherapy drug. (sources)
What makes retinoic acid effective is that it kills replicating cells. He says,
… every cell in the body will convert excess vitamin-A into retinoic acid. The overall rate of conversion is proportional to the number of cells that are exposed to the vitamin-A molecule. I believe it’s also proportional to the number of cells with damaged cell membranes. Therefore, to be safe, there should never be any excess vitamin-A in the body. What does excess vitamin-A mean? It means several things. One is that you never want to consume vitamin-A at a rate that exceeds your body’s safe storage rate.
Genes, diet, age, environment and other epigenetic factors affect our body’s ability to process vitamin A excess. Many with autoimmune issues have inherent detox limitations. But ultimately, anyone with too much vitamin A in their liver will reach that point of toxicity.
He continues, “As we start to exceed the vitamin-A load carrying capacity of those lipids, we will move into the toxicity state … Once we approach these limits, more and more circulating vitamin-A will be exposed to cells, and the subsequent normal processes of converting vitamin-A to retinoic acid will take place.”
Medical science discusses vitamin A toxicity
As one study says,
…there is a growing body of evidences showing that vitamin A doses exceeding the nutritional requirements may lead to negative consequences, including bioenergetics state dysfunction, redox impairment, altered cellular signaling, and cell death or proliferation, depending on the cell type. Neurotoxicity has long been demonstrated as a possible side effect of inadvertent consumption, or even under medical recommendation of vitamin A and retinoids at moderate to high doses. (source)
When there is retinoic acid in the intercellular fluids, cellular damage is most likely to occur, according to Grant, in the eyes and the skin.
Visual disturbances (spotty vision etc.), eye diseases, declining eyesight and dry eyes are extremely common conditions. Eczema affects 20 percent of American children, 30 percent of whom also have food allergies. Skin issues in general affect a huge percent of the adult population.
Grant also has some fascinating insights about the retinoic acid-based drug Accutane and how its use for acne causes the same well-documented side effects as vitamin A poisoning.
Crohn’s and IBS, plus other autoimmunity
Grant takes it one step further to point out that Crohn’s and IBS are inflammatory diseases of our internal skin. Symptoms of vitamin A toxicity and Crohn’s are remarkably similar. (source and source p. 154)
Because the liver can be saturated at any point in a person’s life, it can take a very small amount of additional vitamin A (often coupled with stress) to push someone into a toxic zone.
This explains why many of us “all of a sudden” break out with a rash or start having blurry vision or dry eyes that we can’t resolve. It also explains recurrent and additional autoimmune conditions, or a leaky gut that just won’t heal.
Grant explains,
The body is safely absorbing and storing all the daily doses until it gets to a slightly saturated point. It is important to understand that all those stored doses have not suddenly become toxic; no, they’re safely stored. It’s the additional doses that cannot be absorbed, or absorbed fast enough, by the liver that are now becoming toxic. What these people are doing is filling up their storage capacity for this substance, and thereby reducing their absorption rates. (source p. 164)

What PubMed says about vitamin A toxicity
PubMed studies are part of what convinced me to take a longer look at the concept of vitamin A toxicity.
Mental health
Anthony R. Mawson shares a great article here on the correlation of high levels of vitamin A with many modern mental health concerns, ranging from ADHD to depression.
My own personal experience with mild mental health issues led me to trial the diet just briefly. Immediate benefits convinced me to continue my interest in the vitamin A toxicity theory.
Mawson says,
Environmental exposures leading to alterations in physiological concentrations of retinoids are associated with birth defects and fetal loss. There is also evidence that high serum concentrations of retinoids resulting from dietary intake, vitamin A supplements, and therapeutic retinoids are causally associated with cognitive impairments, mood disorders (e.g., depression), persistent agitation, suicide, and other forms of violence.
Hormonal effects
Another study discusses vitamin A and its precursors as dietary hormones. When combined with environmental pollutants, the author asserts the various functions that can be disrupted, including healthy pregnancies, immune and skin health.
In fact, there are many studies linking excess vitamin A with various illnesses: malaria, Epstein–Barr virus (EBV), Burkitt’s lymphoma (BL) and increased risk of cancer mortality, to name a few. (source, source)
The vitamin A detox concept is an unexpected and exciting new path for those of us desperate enough in our search for optimum health to try something contrary to what we’ve been taught. Science propels us to be among the first to try this diet and report back on its effects on our bodies.
Sudden health shifts
Why act now? As Mawson says, “Given that about 80% of vitamin A is stored in the liver, sudden shifts in these stores to other tissues due to infection, chronic illness or trauma can result in severe vitamin A poisoning.”
Whether pregnant, nursing or struggling with unresolved health concerns, vitamin A in excess is toxic, and it’s likely that most of us have too much stored in our livers.
Eating too much vitamin A
Is it possible that many in the Traditional/Ancestral community are consuming too many vitamin A rich foods?
Even though liver is super high in some good nutrients, does it also contain toxic amounts of vitamin A?
Presumed “super foods” such as liver and cod liver oil are not the only sources to blame.
Americans who consume a standard diet are constantly exposed to vitamin A through glyphosate, the poison so commonly used on American food crops. Even well water is contaminated with glyphosate.
While glyposate itself isn’t high in vitamin A, it greatly inhibits the detoxification of vitamin A.
Which supplements have vitamin A
When considering which foods to eliminate for a vitamin A detox, we must also consider supplements that contain vitamin A, as well as supplements that contain: carotenoids, retinol, retinyl, retinoids and retinoic acid (natural precursors to vitamin A).
I recently exchanged my B complex that contained vitamin A for just a couple of individual B vitamins that I needed. My doctor helped me to add in minerals as well.
Genereux also implicates and recommends the removal of specific carotenoids: lutein and zeaxanthin. (source p. 205)
Anyone with suspected vitamin A toxicity should avoid liver pills, fish oil, krill oil, cod liver oil and any other seafood oils. I myself have eaten and used these supplements for years.
Usually food-based supplements that are dark in color, like spirulina or vitamin E pills, reflect their high carotenoid content and should be removed.
Some supplements complicate the detox of vitamin A
Additionally, Genereux warns that too much vitamin E through food or supplements causes an increase in serum vitamin A levels.
Vitamin C supplements should be removed because they actually cause vA to be stored in the liver, which doesn’t help the detox process.
Dr. Garrett Smith, now the leading researcher on how to detox vitamin A, recommends eliminating vitamin D supplements. (source)
If you currently take iodine, you might also share this article with your doctor and consider the potential dangers of potassium iodide.
Personally, I have eliminated most of the supplements I was taking! My supplements were like my friends. But I am feeling so good, and one by one I have been able to eliminate several of them, something I never expected but for which I had hoped!
Helpful supplements
Genereux takes zinc occasionally, and that’s all.
Dr. Smith is a whiz at supplements, knowing complications that some can cause, which ones are key, and why. I highly recommend working with one of his practitioners, having blood work and a mineral analysis done, so you can accurately supplement for your unique body.
You can read here about the supplements I take, based on testing with him.
Food lists for high and low vitamin A content
My goal with the following list was to create a most helpful and free resource so that more of us can try this diet and make encouraging progress with stubborn health concerns.
As you’ll see below, when we remove vitamin A from the diet, we also remove most colorful veggies. Yet anyone who can digest fruit well can still enjoy some colorful foods on a low vitamin A diet.
Changes to the diet
How best to detoxify vitamin A is still being discovered by Grant, Dr. Smith and those of us on the diet. That being said, occasionally dietary changes to the protocol will be made.
For example, at one point, cauliflower and pears were removed from the diet: formaldehyde in these foods is competing for the same alcohol dehydrogenase enzymes and inhibiting detoxification.
I recommend signing up for my weekly free newsletter, and checking back here once in a while for dietary updates. I also recommend following Grant’s blog, if interested in the process, where he discusses “the experiment”. However, some of the discussions there are not at all led by Grant, and may be misleading.
The very best way to stay tuned in on all the latest updates is to become part of Dr. Smith’s Love Your Liver community, and to watch his YouTube videos.

Foods high in vitamin A (the Avoid List)
Note on the foods listed below: Because vitamin A is fat soluble, you won’t get as much from a food if it’s prepared with water. However, when foods high in vitamin A are prepared or eaten with a fat source, more vitamin A will be accessible and absorbed by the body.
Green tea is a good example: Green tea steeped in water is low in beta carotene, but when the whole green leaf is prepared with fat, in a Matcha Latte for example, a lot of beta carotene (a precursor to vitamin A) is absorbed by the body.
Some of the foods listed below are obscure, but they make the list more complete and accurate.
Meats and Vegetables High in vitamin A (Avoid)
Cod liver oil
Moose liver
Walrus liver
Peppers of all kinds (bell, passilla, ancho, chili etc.)
Turkey liver
Veal liver
Egg yolks
Natto (fermented soy)
Carrots
Chives
Parsley
Paprika and pepper spices like cayenne
Duck liver
Seal liver
Eel
Turkey giblets
Brussels sprouts
Beef liver and other organs
Goose liver
Caribou liver
Pork liver sausage (liverwurst)
Milk
Grape leaves, raw
Lamb liver
Sweet potato (including chips)
Carrot juice
Pork liver
Salmon, herring, tuna, sturgeon, clams, mackerel, shrimp, red snapper, trout, crab
Tomatoes
Broccoli leaves
Canned pumpkin
Kale
Chicken giblets
Lard
Pork
Dandelion greens
Mustard greens
Spinach
Matcha Green Tea
Turnip greens
Collard greens
Winter squash
Mustard greens
Dried apricots
Nutritional yeast
Avocado, and unrefined avocado oil
Olives and extra-virgin or unrefined olive oil
Peas
Pokeberry shoots
Winged bean leaves, raw
Beet greens
Cheeses
Coconut (most but not all coconut products)
Palm oil
Cantaloupe
Mango
Black-eyed peas
Broccoli
Mung beans
Flax
Chia
Cinnamon
Basil
Coriander
Oregano
Thyme
Grains to Avoid
- Wheat (organic white wheat can be “challenged” later in the diet, if desired, with clean sourdough)
- Best to avoid all gluten at first, unless you tolerate and love sourdough.
- Any grain really high in copper, like buckwheat
Other foods to Avoid
- Canned fruits and Aspartame (These belong to the group of foods that either contain or get converted to formaldehyde. These foods, therefore, compete for our alcohol and aldehyde dehydrogenase enzymes, which are required for vitamin A to detoxify.)
- Alcohol
- Earl Grey tea
- Pears, grapefruits, pineapple (affect the detox process)
- Most fermented foods (more on this below)
Regarding all dairy
Grass-fed milk is higher in beta carotene (a precursor to Vitamin A). Dairy consumption is not a good idea for a vitamin A detox. Even the best milk also contains casein and whey, both of which bind to Vitamin A, acting as carriers and transporters. (source and source)
Most people detoxing Vitamin A should avoid all dairy products. A2A2 ghee is an option for some people, because it’s free of casein and whey. A small number of people doing the diet include butter or very occasional small amounts of heavy cream.
Regarding cheese, I used to eat a small amount on the diet, but now I’ve eliminated it. (The fewer toxins you take in, the more your body can release.)
Regarding yogurt, it is out because it is made from milk and high in aldehydes (which slows down the detox of vA).
Because of the new recommendation (2025) to include 500 mg of dietary calcium daily, some low vitamin A folks are including small amounts of non-fat high quality yogurt in their diets.
I can’t do this, or I have a reaction to the vitamin A. I don’t recommend this.
Foods to avoid, High in stearic acid (that increase vitamin A issues)
This category of foods is very important, but less known, for those doing vitamin A elimination diets. (source)
Stearic acid, unmentioned by most articles on vitamin A toxicity, is what helped me to see the vitamin A theory’s relevance in my own health journey. While my recent diet was somewhat low in most vitamin A foods, I had begun to struggle with new mental health issues that were getting worse.
I realized I had started consuming cocoa butter (with matcha) daily. The day I removed cocoa butter (and matcha) and cocoa from my diet, my healthy brain and thought patterns returned!
Stearic acid may or likely exacerbates vitamin A issues, especially during initial detox stages. Also watch for it in your supplements.
Common sources of stearic acid:
- Beef tallow
- Cocoa butter and dark chocolate
- Coconut oil
- Lamb
- Butter
Some of the above foods may affect you more during an initial vitamin A detox and become tolerable and benign over time (although coconut oil should be refined on the diet, and butter should not be added over time). But lamb may be introduced by some.
Foods to avoid, High in aldehydes (that increase vitamin A issues)
Here’s the piece of the diet that I overlooked, and it was an addition that came later.
Aldehydes are a compound in certain foods that impede the detoxification of vitamin A. The more you eat them, even if they’re low in vA themselves, the more likely you’ll see flares and problems in your detox process.
Avoid these foods for best results on the diet:
- most fermented foods: yogurts, fermented vegetables, kombucha
- chocolate
- coffee (especially instant)
- alcohol
- cinnamon
- vanilla
- citrus oils
- watermelon, other melons, pineapple
- sugars
- starches
True/real sourdough bread is fine to eat once your GI tract is ready for it; so it’s one fermented food that is not included in this aldehyde category.
Reminder
Get the latest food updates from Dr. Garrett Smith N.D. here. (To become part of the Love Your Liver network, there’s a fee, but it’s more than worth it. Dr. Smith has become an authority on vitamin A detoxing and guides his patients through the process. Plus the other members are invaluable; so much support happens in the group. See you in there!)
Vegetables, grains and legumes with No vitamin A

On a vitamin A detox diet, it’s important to avoid glyphosate as much as possible, because it hinders the detoxification of Vitamin A. Therefore, go out of your way to buy organic.
Some of the following foods are obscure. I’ve put an * next to my favorite or the more common no-vitamin A foods. Listen to your unique body to create a gentle diet for your healing process.
Amaranth (a good source of dietary calcium)
Arrowhead tuber (may contain RS)
Bamboo shoots
*Beans — White beans and vaquero beans are best because they’re a great source of dietary calcium. (Eat only if you tolerate beans: For best digestion, soak 48 hours in a new change of plain filtered water each day, rinse, then cook in Instant Pot, optionally with baking soda for no gas. Also, see this beans list, based on blood type, which is what allowed our family to start eating beans again.)
Burdock Root
Butterbur, canned
Celeriac (celery root)
Chayote
*Corn, white or blue
Eppaw
*Ginger Root
Gourd, white flowered calabash
Hearts of Palm, canned (but rinse well if citric acid is an ingredient)
*Hominy, white (Find it here.) — Also a great source of dietary calcium.
Kanpyo (dried gourd strips)
Lotus root (possible, but likely fine)
*Masa, white (This is one of my favorite ingredients on the diet. Find it here.) — Also a great source of dietary calcium.
Mountain yam, Hawaii (May be too high in copper, I haven’t tried this root myself to know how I do with it, but it is high in vitamin B1; it’s a maybe.)
*Parsnips
Pepeao, dried fungus
*Potatoes (Russet, peel them first and no yellow potatoes)
Sesbania flower
*Tahini — only in small amounts for hummus
Water chestnuts
Waxgourd (Chinese preserving melon)
Miscellaneous foods with low or No vitamin A
Arrowroot
Apple cider vinegar (only in small amounts)
Black Tea, Green tea, Oolong, White Tea (but limit caffeine); (avoid Earl Grey) — None of these are ideal on the diet due to polyphenols which slow down detox.
*Carob
Capers
Cassava root, cooked and hot or warm (needs to be fresh, not cold, reheated, nor the flour)
Celery, the lighter in color stalks
*Cucumber, peeled (optional: also remove the seeds to reduce lectins if needed)
*Finger Millet (also called Ragi)
Honey, light-colored
*Rosemary
Sage, in very small amounts
Sunflower seeds (only in small amounts and occasionally)
Tapioca (as always, must be organic, especially important with tapioca), organic pearls here and organic flour here; may be wise to limit amounts of tapioca because it’s a starch. A bit of tapioca flour in certain recipes is handy, if nothing else.
Teff
*Zucchini, peeled
Fruits
Apples and bananas are key fruits for a lot, if not most, of the people who detox vA. Many also enjoy dried black figs, since they were recently discovered to be an asset to the diet, due to their high calcium content.
Best fruits: Apples (white fleshed only), bananas (no green bananas or overly ripe bananas), black figs (fresh or dried) and green grapes
Peeled fruits: Fresh applesauce (but not store-bought or home-canned), white peaches, lemons and limes (not the rind), pomegranate
Other fruits in moderation: blackberries, blueberries, currants (a good source of dietary calcium), raspberries, strawberries — All of these can slow detox, so they should not be staples.
Meats
beef, bison, chicken, turkey, wild game, possibly rabbit
Seafood: Eat minimally (not encouraged) — A few kinds of whitefish are low in Vitamin A (retinoids and carotenoids): Petrale sole, flounder, cod. Any white fish choices should be lower in fat.
Grains
Brown rice, hulled barley and oats are the main grain staples.
If you choose to eat white rice, it’s important to consider a B-1 supplement or eat beans (or other foods high in B1); otherwise it can cause a deficiency. Balance one with the other.
Also: Amaranth, blue or white corn, masa or cornmeal (no yellow), sorghum and quinoa.
UPDATE: With new guidance to increase dietary calcium, a new grain has been added to the encouraged foods to eat: Finger millet, also called ragi. It’s very good. I use both the flour (looks like there’s a limited supply) and the whole grain.
Proceed slowly with grains to be sure you can digest them well, if you don’t currently tolerate them.
Nuts and seeds
Most nuts are okay in moderation (just small amounts and not regularly); make sure they’re organic. (As it says above, avoid cashews [which are actually a fruit] and peanuts [legume], as well as flax and chia.)
Both sesame and sunflower seeds have gone on and off the Yes list of foods for the diet. Tahini is fine in hummus.
A few nuts, in moderation, seem to actually be beneficial, for some people, to the detox process, like walnuts, macadamia nuts and pecans.
Lettuces
Some organic green lettuces are allowed on the diet: iceberg, hearts of butter and romaine only. No red lettuces or extra bitter lettuces.
Allowed spices and seasonings
- Anise
- Caraway
- Cardamom
- Celery Seed
- Cloves
- Coriander
- Cumin
- Fenugreek
- Ginger
- Coconut aminos
- Tamarind
Herbs: Rosemary, Mint, Dill
Baking ingredients
- Baking soda, and baking powder in small amounts (often contains calcium powders which aren’t ideal)
- Cream of tartar
- Natural sweeteners (if light colored, but coconut sugar and maple syrup are allowed; avoid dark honeys and molasses)
Foods high in detoxification enzymes and low in vitamin A
Certain produce items not only help to improve our gut microbiome diversity, they also help to usher vitamin A from our livers.
While this diet may seem like a lot of beef and not enough produce, you can add in the following produce items to expedite your detox process and for variety: white-fleshed apples, peeled lemons and limes, rosemary, walnuts and grapes.
Regarding ginger, for occasional use, add it to smoothies, stir fries, swallow it minced/grated on a spoon, stir it into water.
If you need digestive support when you first start the diet, consider this tincture in water.
Important basic principles on the vAD diet
Food lists are super helpful, but some of the principles that Dr. Smith and Grant Genereux have learned in the last almost seven years are just as important. If you choose to do this diet, I recommend you join the Love Your Live forum for support and to gain the latest information and updates.
One of the most important principles understood and relayed in the last two years has to do with soluble fiber.
Dr. Smith emphasizes the importance it plays in carrying out toxic bile, which contains vitamin A, from our bodies.
Recommended sources of soluble fiber include: oats, beans and a low-FODMAP prebiotic fiber called SunFiber. Start slowly with a very low dose of all of these (at different meals throughout the day), so your body can adjust.
Gradually increase soluble fiber, but very slowly. Otherwise, digestive upsets can occur.
Most of us also take this activated charcoal to protect us from toxic bile.
PRINTABLE VITAMIN A DETOX DIET GROCERY LIST (updated 08/25)
You can Print the grocery list below here.

Prebiotic foods and resistant starch
Dr. Smith has observed that resistant starch (RS) is not beneficial to the detoxification of Vitamin A. He links to studies (here) showing butyrate increases retinoic acid production.
As you may remember, butyrate is the short chain fatty acid consumed by T-cells, which in turn increases T-cells and diversifies our colon ecosystem.
Inulin alternative
Also of note, my son’s long time eczema went away very quickly when we added in inulin, a prebiotic. Dr. Smith states that inulin feeds bad flora. As the Nemechek protocol has shown, inulin can be a powerful way to improve the gut microbiome and skin health. Yet long term, diverse forms of prebiotics are better than a single source, and sometimes we have to take one goal at a time.
Dr. Smith recommends only certain prebiotics on the vA detox diet (like this one).
Prebiotic foods to avoid
Avoid cassava flour, tiger nuts in any form and the flour, jicama, chicory, raw onions and fermented asparagus. Here’s a fuller list of prebiotic foods that may affect vitamin A detoxification.
Included in that list, note that cooked and cooled beans have RS. These do not seem to cause any problem once you’ve been on the diet for a while, but may cause issues during the initial months.
Why tapioca is okay
Happily, one food comes out of the resistant starch conversation free to be eaten, and that’s tapioca.
Extracted from cassava root, tapioca flour and tapioca pearls do not contain RS. To be more specific about cassava, cassava root belongs to the RS3 category of resistant starch foods. This means cassava gains resistant starch when it’s cooked and cooled. It is possible to eat the whole root cooked and hot or warm and not get any resistant starch.
We buy frozen, raw cassava root at our local Asian grocery store. It is less inflammatory than potatoes and works well for some people as a healthy source of complex carbs. (The flour, in contrast, already contains RS. And tiger nuts, in contrast, have resistant starch even when they’re raw [RS1].) We do eat fries made with cassava roots and have no problem.
My story
Regarding my own symptoms and my progress thus far on the diet, I felt initially hopeful when I read more about the symptoms associated with chronic Hypervitaminosis A:
“The toxicity of Vitamin A (hypervitaminosis A) is manifested in two forms: acute and chronic … Chronic hypervitaminosis A is much more common and insidious. It is generally associated with self-prescribed over-supplementation by humans … Toxicity at the cellular level is manifested by redifferentiation of simple types of epithelium into more complex forms, including mucous epithelium. Accompanying this is decreased cohesion between epithelial cells in the skin. Accordingly, most affected humans report skin changes such as … eczema … double vision … ”
This study goes on to describe more of my symptoms including Vitamin A’s pro-oxidative effects on the lungs and its role in anemia. Other symptoms addressed affect two of my loved ones and include issues with bone density and liver health. (source)
After two months:
I saw an immediate and lasting improvement in my mood and mental health, a major improvement in my skin, a day or two of “die off” symptoms and significant anti-histamine effects. Urgency (I have a bladder disease that is in remission) returned after two weeks on the diet. That symptom lasted two weeks and is now resolved. (Vitamin A is very closely related to bladder issues, because it affects epithelial cells and their tight or loose junctions, but also to kidney health.) My sight issues (on and off cloudy vision related to oxalates) have improved.
While this diet isn’t for the faint of heart, the improvements are so encouraging and far outweigh the challenges. I can’t imagine not pursuing this path fully now.
After 2-1/2 years on the diet!:
I am doing great, friends!! This diet has been an amazing help to me. I plan to continue on the diet for another year or so because I’m still seeing benefits, and I believe my body is still detoxing Vitamin A.
After 1-1/2 years, I was able to put my endometriosis into remission. Hashimoto’s in remission, too!, off all thyroid meds. This diet is nothing short of amazing for hormone balancing.
I have zero bladder issues. My histamine intolerance and MCAS is long gone.
The only health conditions that remain for me are a chemical sensitivity, and I maintain a medium oxalate version of the diet. Basically, I’m well and feel great. I do still need to improve my chemical sensitivity, so that’s my ongoing goal. But the VAD diet has been nothing but positive for me, as well as for my kids and husband.
I’ve reduced our supplements significantly, and they’re very specific, based on testing.
Here is my exact current diet and supplements.
And here is my latest update: 5 Years on a Low Vitamin A Diet.
Notes on the ups and downs
Negative symptoms can return during the detoxification of Vitamin A. My N.D. says the body revisits old illnesses as it heals itself. Also Vitamin A can cause issues as it detoxes from the liver.
I experienced decreased immunity on my skin starting at the six week point, which Grant has commented can be a “more tox” stage for the body.
Additionally, I got a staph kidney infection as a result. I used allicin, tea tree oil (here’s how), colloidal silver (here) and goldenseal to combat it and avoid antibiotics. In retrospect, colloidal silver was the most effective and best fit for a low Vitamin A diet.
Even my onerous symptoms encouraged me and baited my curiosity — that this diet affected my issues and allowed my body to heal at a deeper level!
VAD diet NOT working?
If someone believes in this diet and its potential but sees no personal benefits after trying it, here are few questions to ask:
- Have you had your food intolerance evaluation done? You could be eating a food your body can’t digest genetically, discussed at length here. I ask all my clients to get this evaluation done so we can build their diet with this foundational information. (I do not benefit in any way from you reaching out to Dr. Zeff [here] to get his kit in the mail. There aren’t very many doctors who do this evaluation, but there are a handful.)
- Is your diet high in aldehydes or stearic acid?
- Are you including enough soluble fiber (or too much)?
- Have you assessed your mental health? Although more subtle, this is where some people see their main benefit. The brain may be healing itself before other body issues are addressed.
- Are there other foods you’re eating that are NOT gentle: THINK grains, like rice or oats. Think too many nuts or seeds. There are several foods allowed on the VAD diet that could be inflammatory, like potatoes. I am reachable here for support if you need help figuring out your unique diet. Or ask me quick questions below in the Comments section.
- Is your diet too high in fat?
- Have you eliminated alcohol and excess sweeteners?
- Many other healthy lifestyle choices are also needed for this diet to work: no smoking, no artificial foods, flavors, avoiding pre-packaged foods (even the packaging materials affect our process), chemicals, stress and more.
- If you’re struggling at all, it’s best to pay the small fee to be a part of Dr. Smith’s forum so you can ask questions and read the latest insights.
Are you considering a Vitamin A detox? I’d love to hear your experience.
And, here are several low Vitamin A recipes to get you started:
- Gluten-free Rice Bread
- Oat Bread
- Rice Flour Porridge
- Bean Milk (my favorite! I use this daily on my oatmeal.)
- Pan-Fried Parsnips
- Turkey, Apples & Parsnip Hash
- Healthiest Congee Recipe
- Dill Pickle Ground Beef Soup
- Carob Muffins
- Bean and Oat Waffles
Find LOTS more Low vitamin A recipes here.
Learn the latest on how to do this diet (and receive community support), here, on Dr. Smith’s forum.
You can Pin this post here:

Additional Sources
1, 2, 3, 4, 5, 6, 7, 8, 9, 10, 11, 12, 13, 14, 15, 16, 17, 18, 19, 20, 21, 22, 23, 24, 25, 26, 27, 28

Carol Little R.H. @studiobotanica says
Thanks Megan for this very indepth look at the VA ‘diet’. I have pinned and will print for reference. I sincerely hope that you will find this of great personal benefit and look forward to your update in 6 weeks!
As usual, I totally respect that you share your references which, in a post like this one, is SO appreciated.. I will be reading and re-reading this to see if any of my own clients can benefit.
Megan says
Thanks Carol!
Nader ibrahim says
Would hulless barley be okay on this diet? And also wild rice and broccoli stems?
Megan says
Yes to hulled barley. No to wild rice and broccoli stems. 🙂
Heather Wormsley says
The comment about iodine drops scared me. We use Lugols daily to counter fluoride in our water (cheaper than a fluoride filter). I guess I will be in the market for true iodINE instead of the potassium iodide.
Re: the VAD itself, I look at the list of NOs and think, “There goes the rest of my food”. I am already so intolerent of so many “Healthy foods” that this made me want to cry reading. I think I’ll strive for a reduction of Vit. A sources, instead of an elimination of them. Thank you for this info, Megan.
Megan says
Hi Heather, you’re welcome. 🙂 I think that’s a great way to start, actually. When I first started the diet, I tried to start completely, but there are just too many subtle areas where Vitamin A foods or supplements are woven into our lives. I think I ate beef and potatoes for three days straight, LOL, before I figured out how to feed myself all over again. I’m going to start my kids gently. I first removed Vitamin A supplements from their diets, because that’s a major source and easy to remove. If you are encouraged after you begin, you may find additional foods you CAN have that allow you to remove a few more offenders. I find that my old food limitations are going away quickly, so I have new foods now. I hope the same for you! Feel free to comment again or email if you have any specific food questions. I’ve gotten good at it now and am eating well. Re iodine, sorry to make life more complicated, and I hope you find an easy solution.
Debi says
I am feeling the same way.
Linda K. Cornett says
Heather, I feel the same way. For 9 months , I have lived on a limited diet trying to heal my leaky gut . Now the food I love most on my present food plan need to be eliminated. I thought about it and decided to try it two weeks ago, taking the charcoal to help take care of releases toxins. Then go back to the other plan but limit those with high vitamin A content. Praying this works out well .
Theresa says
I see lamb in the stearic acid list as one to be avoided but then in the pink and blue printable list it is in parenthesis. Do the parenthesis mean it is to be avoided? I am looking into getting lambs to raise on pasture and so I am very interested in whether it is acceptable for VA Diet or not 🙂 Thanks.
Megan says
Hi Theresa, great question. The few foods in the stearic acid list are foods that are more likely to exacerbate the Vitamin A detox in the beginning of the detox process. So lamb can be added back in, but best to avoid in the beginning of the diet, and re-introduce with caution. This goes for the other items in the stearic acid list as well, like cocoa.
Cathy says
Why are you not able to eat fruit?
Megan says
Hi Cathy, here’s my story of healing my IC: https://eatbeautiful.net/2015/10/04/how-i-healed-my-interstitial-cystitis/ Also, if you follow the link in the article about food intolerances, that goes into great detail on the concept. While the medical community considers interstitial cystitis to be incurable, I put mine into remission by simply removing fruit, my food intolerance. I had also been doing the GAPS diet for some time, which was helpful to the epithelial cells that line the bladder, urethra etc. As long as I stay away from fruit, I am symptom-free. With the VAD diet, I have occasional urgency now, which to me is temporary and just part of the deeper healing of epithelial cells that needs to happen. My daughter also put her asthma into remission by eliminating her food intolerance. I have dozens of similar stories. One’s food intolerance is a key to digestion and gut lining healing (and is different than one’s food sensitivities).
linda spiker says
Very interesting! I never knew any of this. Of course I knoew Vit A could be over done and make one ‘toxic’ but I never knew about Vit A detoxing and the similarities between Vit A and Crohn’s disease. Thanks for the good read!
Megan says
You’re welcome, Linda! These concepts are relatively new, as of 2015, and they have not been broadly accepted or even read yet, so it’s no wonder they are new to you too. It will take the mainstream a while to consider these truths and trial them. So it’s pretty exciting to be on the front lines and experiencing the diet first hand! Perhaps only the “desperate” will try this diet in the beginning, and then as more and more testimonials of healing and success spread, more people will be willing to try the diet and appreciate the concepts, similar to GAPS, but I think with even greater potential.
Mary Voogt says
Good info. Hopefully people will still look to Dr. Smith for details about the Vitamin A Detox/BAD-AG protocol.
Just wanted to note for anyone reading this that the body can store enough Vitamin A in the tissues to last 2 years. So this is not a short-term diet. I have been on it for 8 months and still have quite a ways to go! Kids will detox faster, more like 6 months or so.
You will likely see some change in 6 weeks. But that is just scratching the surface. It took a long time to get toxic…it will take a long time to detox. Just want people to be aware that this is not a quick fix. There is a bit more info about the end goal here: https://justtakeabite.com/2019/06/19/come-off-vitamin-a-detox-diet/
Also, organic wheat is allowed. We are now enjoying homemade sourdough at this phase.
Megan says
Hi Mary and thanks for your comment! I’m sure Dr. Smith will continue to reach hundreds and thousands of new readers and clients! 🙂 My hope is that this information in general reaches as many as possible!
I appreciate the article about phasing off the VAD diet and appreciate the link you shared, how helpful.
Regarding the duration one stays on the diet, it’s encouraging how quickly kids make progress! The hardest part doesn’t have to last long. Thanks for sharing that the diet can last as long as 2 years. That can be intimidating when someone is considering a whole new dietary concept and diet. I suggest starting the diet and looking for improvements. If things go well, we can think in terms of 6 weeks or 6 months, and then 2 years as needed and decided as time elapses … or if one’s symptoms are desperate enough to be ready for that commitment. Personally, some of my symptoms are gone (amazingly!) after just two weeks. I expect other symptoms to take longer. I also know that some symptoms will come and go as I heal. I read one account of someone who is seeing no progress on the diet at all after several months, which is why I included the troubleshooting section in the article above.
How great that you all are tolerating and enjoying sourdough now!! Most of my readers are gluten-free, and many are grain-free, so just to clarify: An organic unfortified white wheat flour would be gentle on this diet *if someone already tolerates grains/gluten or is ready to trial them after being on the diet.
Chantal Schutz says
Thank you for all the information here. I have also been exposing myself to Dr. Smith’s materials through his paid program. I am keen to hear about your recipe for the homemade sourdough 🙂 if you can share!!!
Deborah says
Thank you for this information! Can you share the multi vitamin you take that does not contain vitamin A? Thank you!
Megan says
Hi Deborah, yes. I take this one: https://amzn.to/2X9C2ZO I like that it includes alpha-lipoic acid and inositol. NOW supplements are always affordable, which is nice too! The one downside, which is why I didn’t share it above, is that it does contain a tiny amount of stearic acid in the “Other ingredients”. I am making such noticeable strides that I don’t think it’s an issue, but just be aware.
Deborah says
I’m sorry, I’m new to a lot of this, but why is stearic acid bad? This pretty much looks like a b complex vitamin. I just switched to a new b-complex: Seeking Health. (I use to take Vital Proteins Beef Liver capsules as my multi, but now will come off of them due to the high vitamin A. Am I missing something?
Megan says
It’s okay Deborah. 🙂 There is a paragraph in the article above, but it’s a long article :), that mentions that stearic acid can exacerbate the detox of Vitamin A, especially in the beginning of the process. I have experienced this personally. A tiny amount like in that supplement is probably not an issue, but it’s best to avoid foods or supplements that have notable amounts of stearic acid (foods like tallow, cocoa and lamb).
Deborah says
Oh, ok. I am sorry! I just went back and read that! Thank you! I am beginning to get the whole picture here. (Takes me awhile sometimes!) So you mentioned removing D, so does that mean we should avoid sun exposure or at least limit it? Also, is there a test for Vitamin A toxicity, i.e., bloodwork?
Megan says
Hi Deborah, great question about Vitamin D. We should get regular exposure to sun, in my opinion, but avoid burning. Here’s a great article on how to get Vitamin D from the sun! 🙂 https://www.thetanningguru.com/tanning-all/do-you-know-how-to-tan/
Regarding Vitamin A toxicity testing, there is not one blood test, but this article offers a bit more insight: https://nutritionrestored.com/blog-forum/topic/blood-tests-for-poison-vitamin-a/ My doctor and I found it much easier for me to just start the diet, especially because I had several symptoms associated with toxicity, to see if it would help. And it did. While it’s a controversial approach, it’s also safe and costs nothing financially. Sometimes the best test is just to begin. 🙂
Rebecca says
Thank you for this extensive article. I have been considering the Vit. A Detox diet, but have been procrastinating. Maybe I’ll get my act together soon.
Megan says
I’m so glad Rebecca! Best wishes as you begin. May it be encouraging and super helpful with your health challenges!
Tessa Simpson says
This one is totally new to me…and one of those tricky chronic health cases with one of my kiddos, I love learning new things and exploring new avenues!
Allie Whitney says
Upon reading this I can see that I would likely benefit from this diet, but it is very hard to swallow. I’m not sure if I’m for such a big “project” when right now our clean eating habits we have in place are easy and work well for us. Sigh. But there are indeed pesky AI issues at play.
One thing I cant figure out is how I will get enough energy from the allowed foods? As someone who relies HEAVILY on cocoa butter for my morning fat, sardines in olive oil for my midday fat, and veggies covered in fat for dinner, these are my main sources of energy. Megan how do you handle this? How do you stay full and energetic? Thanks in advance!
Megan says
Hi Allie, thank you for sharing and your questions. Well, firstly, we are different bodies, so I can’t say for sure what your body’s needs are, but I can tell you what happened with me. Before starting the VAD diet, I probably ate more fat than anyone I know, even those on a Keto diet. I LOVE butter, cocoa butter etc, and they helped me to feel good. So we are similar that way. 🙂 On the VAD diet, I limit my fat intake to some extent, … and I feel the best I’ve felt in years, and it’s lasting. My mental clarity and happiness is SO encouraging to me. And my body keeps working through symptoms, which is actually fun to watch. So my experience is that the diet helped me feel energy and happiness, both of which propel me each day and help me to love this new approach. I do not lack for energy with decreased fat. When I switched foods, my body’s cravings and what satisfies me changed. So now I eat a lot of beef, whereas before my body could only take so much protein before it said, Stop! No more meat, please! I know I need 50 grams of protein minimum daily to detox Vitamin A, so I eat a lot of meat and egg whites, but I always want it. I have also fallen in love with teas. They bring me joy and nutrition, and they may provide a lovely boost to you in the morning as you get started. I nurse my cup, but I don’t get a caffeine buzz. Also, be patient if you choose to start. The first two weeks are all about figuring it out. Even if you know the foods you can and can’t have, there will likely be a few hiccups and various good or not good symptoms. Also, a possible decrease in energy with initial detoxing is not a bad thing, if you see the overall direction you’re going and feel it’s part of the process. My good progress far outweighs any symptoms that surface. Hopefully the positive changes you see will propel you forward. Best wishes, and I look forward to hearing how it goes!!
Deborah says
What is A2A2? I’ve heard of A2 but not A2A2. Is that different? And, I’m confused as to why no “leftover” white rice.
Megan says
A2A2 refers to the genes of both the mom and the dad. Here’s an article I wrote explaining more if it’s helpful: https://www.foodrenegade.com/which-milk-to-choose-is-a2-superior/
Megan says
Regarding white rice, it forms RS3 when cooled, even if it’s reheated. You can read more on resistant starch here: https://eatbeautiful.net/2014/12/22/what-are-resistant-starches-and-who-should-be-eating-which-ones/
Sarabeth Matilsky says
Hello! Thank you so much for this helpful article – I have been lurking around the Interwebs for the past few weeks, learning about the Vitamin A Detox idea, trying to determine whether it would be worth putting my husband through yet one more attempt (starting with GAPS ten years ago!) to help him feel better…
We started this morning. 🙂
Anyway, I got the brand of acerola powder that you recommend, but it turns out to be a significant source of vitamin A according to whatI read online today. Are you still using it? Is there some reason all that vitamin A is okay?
Thanks for all your useful recipes and optimistic wisdom! I am attempting a Low Vitamin A sourdough waffle batter (and also bread) – I will let you know if it comes out well enough to share. 🙂
–Sarabeth
Megan says
Hi Sarabeth, you’re welcome, and thanks for your comments and questions! I know how you feel about deciding to put a family member on a healing diet and only wanting to do it if you’re pretty sure it’s worth the ups and downs to reach the end goal and get results. How exciting that you’re diving in, and may you see encouragement and renewed health.
Regarding acerola cherry powder, it is low in Vitamin A. I’m not sure of your source. However, in general, fruits that are allowed that contain Vitamin A, are allowed because they have other components that assist with detoxification (such as glucaric acid, Vitamin C, Vitamin E and bromelain). So the good ushers out the bad and outweighs it. 🙂 Yes, I use acerola cherry powder Vitamin C for my kids. (I personally use the tapioca-based one because I don’t digest fruit well.)
I look forward to hearing more about your recipes! 🙂
Sarabeth Matilsky says
The low-Vitamin-A waffles came out great!! I added the recipe variation (the original of which I adapted from your awesome recipe, as attributed), here: 🙂
http://www.lifeisapalindrome.com/recipes/sourdough-cassava-waffles
I’ll test the sourdough bread tomorrow.
Regards,
Sarabeth
Megan says
Both of your recipes look great! Thank you for sharing and your attribution. I’m so happy to think of you enjoying such a great daily wholesome treat! (Hurray for waffles!)
Sarabeth Matilsky says
I’ve been making a low-A gluten-free sourdough bread lately, which is very popular for my lunchtime crowd.
I’d love to hear what others are making and cooking and experiencing on this diet. 🙂
Kassia Batista says
Hi Megan, what is the test to assess whether someone has a toxic load of vitamin A? I would think only a small group of people would need this detox. As Weston Price discovered, traditional cultures were eating up to 10 times the amount of vitamin A as we modern Americans typically do, and they were very healthy.
Megan says
Hi Kassia, thanks for your great questions! I have talked with my doctor and read up on the topic, and there is not a reliable test for vitamin A toxicity in the liver other than symptoms. I have been a loyal Weston A. Price advocate for more than a decade, but I think the Foundation has some things wrong. While I’m a huge advocate for pasture raised meat, raw milk for those who tolerate dairy, soaking, sprouting and sourdough, fermented foods, traditional fats, bone broth and avoiding processed foods, I now believe that supplementing with cod liver oil and liver is dangerous.
Dr. Ron Schmid was an ND, author and WAP advocate who died of heart failure. He took cod liver oil in high doses for many years. He wrote a good article here that doesn’t uncover the role of vitamin A but *begins* to see the cause and effect and dangers of cod liver oil: https://www.drrons.com/product-blog/Too-Much-of-a-NOT-so-Good-Thing While Weston A. Price found healthy cultures eating traditional foods, I do not believe he found healthy cultures living on daily consumption of liver and cod liver oil over the course of years. In fact, history shows us just the opposite with signs of vitamin A toxicity in those who survived on liver. We have been given misinformation. Ironically, those of us who want to be healthy the most are feeding ourselves foods that are not meant for daily consumption. We have taken the word of the WAPF without adequate evidence.
Additionally, if you go back to the original vitamin A animal studies, they were considerably flawed. These studies were supposed to prove (and are the foundation for our modern medical beliefs) that vitamin A is required for good eyesight and many of the body’s other functions (as you name in your other comment). Instead, these early researchers knew so little about nutrition and the precursors to vitamin A, the diets they designed were horribly inaccurate. It’s shocking that it’s taken this long for someone like Grant to come along and look at the original studies and question them. (I love an example he uses in his second book: a rat can live through the winter on nothing but vitamin-A deplete grain, but it couldn’t survive the scientists’ vitamin A deficient diet for 8 weeks! Yeah, their diet wasn’t deficient. It was FULL of vitamin A, and the rats died of vitamin A toxicity.)
Although there’s a time commitment, I highly recommend you read Grant’s books. He gives hundreds of links to scientific studies and historic examples. https://ggenereuxblog.files.wordpress.com/2018/02/poisoningforprofits1.pdf
Those of us who have chosen to be a part of this grand experiment are the ones saying how amazing it is. We are watching our own bodies heal themselves, and it is nothing short of amazing. It’s not popular yet, and it will take a while for most people to consider this concept. But meanwhile I am watching miracles happen in my body. Grant watched them happen in his body. And there are hundreds of us saying, WOW, this is something new and real to consider. If I tried the diet and it didn’t work, I’d be the first to run the other way.
The first priority for every person who considers these truths is to check their vitamins and consider removing all synthetic vitamin A, like from B vitamins and multivitamins. I started there, then I removed liver pills and cod liver oil. Then I was struggling so much I decided to try the diet. Immediately the face rash I’d been struggling with for 11 months went away (over the course of 2 weeks). My depression was gone immediately (1 day) and has never returned. The cloud over my left eye that no doctor could figure out took a full month, but now it’s gone. I am truly amazed. There are many other symptoms I won’t list here, but I plan to write an update. In short, my eye health improved drastically by removing vitamin A, my skin is rash-free, my mental health is wonderful! Some of my symptoms (like my urethra issues) have come and gone, which my ND says is typical of getting well: The body revisits old sicknesses as it heals itself, and if the vitamin A theory it right, the vitamin A detoxing can cause issues as it detoxes.
Well, you’ve gotten a long answer! But I hope it’s a beginning for you of asking more questions and continuing to search. It took me weeks to believe in this theory, but now I am SO thankful for Grant’s amazing insight and research.
Lastly, I do not believe that all foods containing vitamin A are bad. I believe that a balanced diet is healthy. But our current set of beliefs about loading up on super foods that include the rainbow foods and liver is not the right path. If someone doesn’t supplement with vitamin A (including processed foods that are fortified with it), detoxes well, avoids glyphosate etc, there is much less concern. But for those of us who added vitamin A to our diets for years, we need to allow time for our livers to detox vitamin A.
Cind says
Is it possible that’s more a result of removing supplements than real food? I personally follow what my ancestors had available, and that means real food, limited supplements in times my body needs more support. Seasonal eating. Cod liver oil helped me heal cavities, but once healed I discontinued regular use. I also take the liquid and avoid capsules as much as possible. My folks ate liver once to twice a month (and mostly chicken liver), so that is what I do.
Megan says
Hi Cindy, your approach sounds good, especially if it’s what’s working for your body. I wasn’t able to remove my supplements until I’d been on the diet for about two weeks (I removed them gradually). For example, I supplemented with iron. The liver pushes out iron to make room for excess vitamin A, in an effort to protect the body from free-roaming A. Thus anemia results from vitamin A toxicity. When my body began detoxing/unloading from the liver excess A through the diet, I went off my iron supplement. Also, the depression I was struggling with lifted right when I began the diet (still on the supplements) and removed stearic acid and matcha. There are other examples too, but that’s the idea.
Kassia says
Megan, thank you so much for the lengthy response! It’s taken me so long to read it. I must have missed the email notifying me. Anyway, I will definitely look into it. Thanks!!
Megan says
You’re welcome! 🙂
Kassia Batista says
I forgot to say, I’m especially concerned for children being put on a low-vitamin A diet. Isn’t it a crucial vitamin for immune function, bone growth, vision, teeth, etc.? I must be missing something here.
Megan says
No, I don’t believe it is a crucial vitamin. I believe we have been misinformed. There are even families with children who have chosen to have no or low vitamin A diets for years whose children are thriving. Many or most have overcome health issues they couldn’t otherwise surmount.
Bria says
Hello!
May I first say I am so thankful to have found your blog. Even though I have been doing GAPS for over 3 years now with my children, I am amazed at the amount I’m still learning about health and nutrition. At first I was feeling great!, then I started having some peculiar issues (light-headedness especially when physically active, bloodshot eyes, decreased vision, very irritable, lost too much weight, no menses since having second child) . I assumed it was from adrenal fatigue from high stress at my work (and extra work around home cooking fresh from scratch!), but now I’m wondering if it could be linked to vitamin A. We have been “eating the rainbow” and I try to incorporate all of the superfoods – greens and oranges with almost every meal! We have also been doing CLO about every other day and eating liver on occasion.
I have been doing the vitamin A detox diet for a few weeks now. I have had no blood pressure/light-headed spells or bloodshot eyes, or vision trouble. Coincidence?
I was wondering if you would answer a couple questions for me?
1) Vitamin b supplement (berry-based) – and spirulina on occasion for iron etc. – if we consume first thing in the morning with no fat, would you still be worried about absorbing the carotenoids?
2) I have been “cheating” a little (eggs with yolks, meat with ground organs, goat and sheep’s milk kefir, salmon, cod, some avocado) because I don’t throw out food and that is what I have. Plus I don’t know if I should cut out these foods completely from my children’s diet?
Do you have a limit/daily or weekly intake of vitamin A that you feel if you stay under you will still detox and heal? These foods seem to have low amounts of Vitamin A compared to daily max dose, but I know you had mentioned the recommended dose is too high?
3) Beef tallow is listed as a food to avoid, but beef is recommended – are we supposed to remove fat from beef or eat low fat beef?
4) Would it be ok in your opinion to make juice with “NO” foods, since not taking with any fats? To still get good amount of vitamins in our diets?
I’m so sorry for the lengthy comment and questions. It would mean so much to me to hear your opinion!
Megan says
Hi Bria, thanks for your comments and questions. I am more than happy to answer. I also love hearing from folks who are trying this diet, about (former or current) symptoms and responses to it so far, so thank you for sharing. That really helps other readers too. 🙂
In my mind, the best approach for your family would be to consider yourselves to still be phasing on to the diet (as opposed to already fully started). This would allow you to finish up what you have on hand. However, I would not buy new food that is high or medium in vitamin A quantity. As you know, I am not suggesting this for you but rather sharing what I’d do in your shoes. This way you can truly and fully do the diet and reap its benefits. Theoretically, if you are putting new vitamin A in your bodies, your liver will not detox stored vitamin A.
I do think this diet is a mental process anyway. We have to get our minds around something new: that the rainbow isn’t as necessary as we have been told and that our bodies will thrive on certain white and brown foods. That being said, I buy and allow a lot of fruit for our kids: berries, grapes, cherries (summer is a great time to start this diet), peeled apples, ripe bananas, dates, raisins etc. I also have lovely fresh things with other meals like peeled cucumbers and probiotic sauerkraut. We also have cooked broccoli and Brussels sprouts once a week each because they aid phase 2 detoxification, and the green is welcome.
To answer your specific questions, 1) I would need to see your B supplement’s other ingredients before judging that product. (Maybe respond with a link to it. Otherwise, if there is no vitamin A in it, berries are fine on the diet.) Personally, I removed my iron supplement and spirulina after 1 to 2 weeks on the vitamin A detox diet. I do think a B complex is important for aiding detox. But I believe the iron levels will take care of themselves over time. I don’t assume this is the case with your body. That’s a very personal decision, and you need to be safe.
2) Personally, I would phase out most of these foods as soon as possible. Most of the foods you list I consider high in vitamin A. They could, however, be some of the first foods you reintroduce in moderation to your kids’ diets. Most kids need only 6 months on the strict detox stage of this diet. So that might help too, mentally: to know this diet isn’t intended to be long term. The one exception to your list is the milk kefir: It depends on its sourcing. Sheep and goat milk are A2, and that food may not bother their process if you observe and feel it’s benign. While I’ve removed raw milk from my own diet, I’ve allowed my family to stay on ours and our homemade yogurt, because there seems to be zero effect. As mentioned in the article, I believe that A2, pasture-raised pristine dairy (beyond organic) may have beneficial effects on detox.
3) Good question. Tallow is only problematic for some people while they are detoxing initially. I avoid extra tallow, but I don’t worry about the small amount that’s naturally in ground beef or steaks. If someone was experiencing vitamin A toxicity from the fat, this would be an indicator to reduce tallow intake. As we start the diet, each of us, we just need to watch and make adjustments. For someone starting out, no extra tallow is a good place to begin. Beef is not problematic for most.
4) No, it would be best in my opinion to avoid all the No foods completely. Instead, to be open to the nutrition you’re getting from the foods on the Yes list. For example, you can still enjoy a variety of cooked (and raw) vegetables: peeled zucchini, cabbage, (peeled Russet potatoes and parsnips, if tolerated), radishes, daikon radish, mushrooms, garlic, onions, cauliflower, broccoli and Br. sprouts etc. occasionally and all the fruit on the Yes list etc. You may find, as I have, that you can re-introduce more non-GAPS foods sooner because this diet allows gut healing, amazing! My kids are all eating organic gluten-free grains now, which I did not expect so soon: soaked buckwheat, white rice, soaked millet etc. Juicing would be best with Yes foods like celery, peeled cucumber, peeled apples and ginger. I trust my kids are getting great nutrition right now. They are happy, energetic and VERY active. Their skin looks the best it’s looked etc.
Bria says
Thanks so much for responding! That really helps. I wouldn’t have thought to reintroduce grains – seems like there is a good and bad side to every single food; we have been enjoying parsnips and new potatoes though! I’m sure my girls would love the “sprouted” bread/muffins and more fruit. They were/I am battling candida so we haven’t had much fruit besides blueberries and green apples. Makes me feel more relaxed to know you feed your kids those foods.
Here is our vitamin C powder
https://www.radiantlifecatalog.com/product/130/119?gclid=EAIaIQobChMI0_yv0Y6i5AIVcf_jBx2YVAI2EAQYASABEgLm3_D_BwE
and vitamin b
https://www.radiantlifecatalog.com/product/premier-max-stress-b-nd/vitamin-b
https://www.radiantlifecatalog.com/product/super-b-complex/vitamin-b (I know this has fermented soy which is not allowed)
Thanks for all the research you do and share,
Bria
Megan says
Hi Bria, sorry for my delay in responding. Those are not good B vitamins. Most importantly, they don’t contain the right form of folate. Here’s a cute metaphor article that explains it very succinctly: https://mindwhale.com/the-differences-between-folic-acid-folate-l-methylfolate-etc/ Basically you need a B with L-methylfolate or 5-MTHF. (https://www.ncbi.nlm.nih.gov/pubmed/25580388) I wouldn’t do that C either, because camu camu, amla and lemon peel are not allowed on the diet, and manioc contains resistant starch. Great about the potatoes and parsnips!! Yeah, I wouldn’t hurry into gluten-free grains. Even though I make these foods for our family, I am watching for symptoms of reintroducing foods too quickly very closely. Sticking with the candida version of the diet sounds wise for now for you. I will not hesitate to back up if we need to. Blessings!!
Bria says
Oh wow I would have never known. Thank you so so much.
Kaitlyn Federkeil says
Great information here! Thank you for summing this up for us!
I was curious though…why Ian nutritional yeast on the NO list? I specifically buy the non-fortified kind and I checked, it has no vitamin A. Is there something else about it?
Thank you!
Megan says
Hi Kaitlyn, thanks for the great question. If you have never reacted to nutritional yeast in the past, small amounts occasionally may be fine for you. But Dr. Smith has it on his no list, and the rule with the vitamin A diet is general is: When in doubt, don’t eat it, especially if it’s a manufactured food. As you may know, glutamic acid is a neurotransmitter found in plant and animal proteins which excites our taste buds and the neurons in our brains. Whole foods like bone broth and aged cheese contain bound, unprocessed, and healthful (for most people) glutamic acid. Unnaturally fermented or manufactured foods like nutritional yeast contain something called “processed free glutamic acid”. In this case, glutamic acid has been freed from its protein during the manufacturing process. It is now an excitotoxin. Excitotoxins interfere with normal brain function by overstimulating neuron receptors in the hypothalamus and causing the death of neurons. This is why nutritional yeast is considered impure: It most likely contains processed free glutamic acid. The highly concentrated glutamates enter the bloodstream then the brain without going through the proper channels of digestion. 25% of the population reacts adversely to free glutamic acid. MSG has similar side effects to neurological drugs. Excitotoxins also cause long-term, serious neuro-degenerative damage, including Alzheimer’s Disease and Parkinson’s Disease. So, best to stay away in my opinion. While MSG doesn’t cause symptoms in everyone, it is a known carcinogen and damages the brain. Any man-made flavor-enhancer should make us cautious.
Bria says
Could you explain why flaxseed not allowed? I occasionally use ground sprouted flaxseed. It says 0% vitamin A, good source of fiber, and no resistant starch that I’ve read. Does it have that stearic acid?
Thanks,
Bria
Bria says
Also what about sprouted quinoa?
Vicki says
Hi Megan, I’m so excited that I have found your info. I’m reacting to salicylates and histamines and now I think I may have found out why. I’m going to launch into this diet and I’m wondering is there a allowed VA amount per day to stay under?
Also what is the best oil to use, I read avocado oil. What is wrong with olive oil I can’t see where it contains VA. Thanks again Vicki
Megan says
Hi Vicki, great! So hopeful for you! 🙂 Olive oil contains green carotenoids. Refined avocado oil is great. I also use some animal fats, like duck fat or shmaltz for variety. Regarding how much VA, the idea is to keep a low VA diet. But the lower the better in one sense, because that allows the liver to detox more A. Some followers of the diet try to eat almost no VA, by just eating white rice, beef and a few other foods. You’ll find what works for you with a little time, trial and error. But no, there is no hard and fast guideline. We tend to enjoy a lot of beef and white rice ourselves. I do use 2 T of butter daily, too, for the Vitamin K and enjoyment. Best wishes!!
Dorothy says
Hi Megan,
I’ve read and reread your article on the VA diet. A family member is trying it out and now I’m looking into it for myself. It should help my husband too as I won’t be buying or cooking the vitamin A foods. I’ve been gluten free for some time and have cooked mostly paleo, autoimmune paleo, and most recently keto. I always feel the need for bread. All those recipes with multiple eggs probably weren’t helping. I recently starting eating cheese again and have been craving it. So now I need to do an about face and try to back off of all those coconut products: flour, oil, milk, unsweetened shredded, and creamed coconut, as well as avocados, salmon, and al those other things we were consuming large quantities of. I’ve eaten fairly “healthy” for a long time, but it’s not helping, as you pointed out. What about walnuts and macadamia nuts? I didn’t see them on any of the lists. Also soaked and dried pumpkin and sunflower seeds? I had been avoiding grains until recently, but have just begun eating some quinoa. Would that interfere with detoxing from vitamin A? What about baker’s yeast? I looked at my avocado oil, and it’s unrefined. It’s in a dark glass bottle, but it’s not there right type. I’ll have to check around do the refined. I gues friend coconut oil is not going to be good to use? I’m testing the waters with this, but haven’t fully embarked on it yet. I’ve heard that rice can be high in arsenic. What type of white rice do you use? Thanks for your help and please excuse my many questions. By the way, I’m reading the first book, and have found it interesting reading, aside from his language.
Megan says
Hi Dorothy, I’m happy for your new direction and choices and hope they will make a great difference for you and your loved ones. Yes, the nuts and seeds you listed are great choices. I would just add to make sure you soak them overnight in salted water (as described here: https://eatbeautiful.net/2014/04/22/how-to-sprout-nuts-and-seeds/), and watch out for rancid nuts. We love macadamias, but because they’re so high in fat, you have to be a bit more careful. Here are the ones I buy that are the freshest we’ve found: https://amzn.to/33W9a63. I don’t recommend quinoa. White rice is perfect. Yes, it needs to be organic because of the arsenic issue. We buy organic Basmati, and I also buy organic rice flour and use it daily. (I buy this 6-pack and have it on the Subscribe and Save feature from Amazon: https://amzn.to/2pO6FUJ) If tolerated, you can also ferment millet and buckwheat. Ideally, you can start a white flour sourdough starter. I never expected to be able to reintroduce this food, but we now eat sourdough waffles every morning, and I make sourdough baked goods regularly (which actually saves money too) with organic white flour. The sourdough must be fully fermented (24 hours). The avocado oil at Trader Joe’s is fine. What brand is yours? Coconut oil is okay if it’s “triple filtered” or refined. Yes, I had to get past the language in the ebooks too, but well worth it. All of your questions are great ones, and so glad you asked. I think I need to write a post with all of these details for others as well. Blessings!! I’ll love to hear how you all do. It’s a bit bumpy at some stages, but worth getting through the symptoms to truly detoxify and get well. 🙂
Dorothy says
Hi Megan, Thank you for answering my questions and adding tips and links. The avocado oil we were using was the Chosen Foods brand from Walmart. I just realized that it not only says cold-pressed, but also says naturally refined on the label. I bought avocado oil at Kroger today, their Private Selection brand. It says cold pressed, but also says “refined for a mild, buttery flavor with a hint of nuttiness”. So it may be about the same as the other brand? I’m glad that refined coconut oil is ok to use as well. We don’t have a Trader Joe’s nearby, but most stores now seem to carry avocado oil and refined coconut oil. Other things I’m curious about: You listed canned pumpkin as a food high in vitamin A and to avoid. Does that go for home cooked as well? I would assume it would, being dark orange. I have a crusty bread recipe with almond flour and tapioca, and it has an egg and oil, but it uses active dry yeast. I thought I’d try it with a gelatin egg, but what do you think about using yeast? Are gelatin and collagen both neutral with this diet? I’m wondering how to use carob with the other limitations. I thought maybe making fudge with carob, butter, and stevia or monk fruit drops and maybe a little honey might work well. I’ll find a way when it comes to sweets!
Megan says
Hi Dorothy, you’re welcome. 🙂 The new avocado oil sounds like a good bet. Yes, all pumpkin and winter squash are out. The bread recipe sounds good, and yeast is fine if it doesn’t affect you adversely for other reasons. Gelatin and collagen are both fine. Yes, carob is fine; just don’t overdo butter in the fudge: about 2 T. of butter daily.
Dorothy says
Thank you, Megan, for all your help. ?
Megan says
My pleasure! 🙂
Dorothy says
Hi Megan,
It must be pretty busy with getting a book published. About the organic white rice, do you soak it overnight or during the day, and if so, in plain water? Is black rice a good alternative? I think it would have more fiber.
What about organic kelp powder as a supplement? With Thanksgiving approaching, I’m thinking about the sweet potato and pumpkin dishes. Is it best to avoid them altogether, or would a brief break work well for most people? Also, I haven’t bought organic almond flour yet for the bread recipes I’m using because it’s cost prohibitive. It’s probably worth it, but it’s unusually high. I’m thinking of subbing walnut flour for one of them, which would most likely work well. You mentioned making muffins to eat on the go. Is there a recipe you could share?
Megan says
Hi Dorothy, yes, such a busy time, you are right! 🙂 White rice doesn’t need to be soaked. I use organic Basmati and cook it with plain water, sea salt and a bit of fat. Black rice is not a good option (too high in iron and other questions), but brown rice could be used if you prefer, soaked. I recommend cooking it in a pressure cooker, and here’s a recipe for soaking it: https://thenourishinghome.com/2012/03/simple-soaked-brown-rice/ No kelp on this diet. Sorry, definitely no sweet potatoes or pumpkin. Like a lot of healing diets, once you begin, “cheating” makes things worse. It’s better to think of what you’ll really enjoy that you can have, and focus on those things, instead of what you’ll be missing. So, for example, make apple pie or crumble (with walnut-streusel topping) and rice or bread stuffing with turkey, gravy and mashed potatoes. All of that is fine. For bread and crust recipes, can you have white sourdough yet? Do you know? Otherwise nut and tapioca flour recipes. Walnut flour is a great option and MUCH better than almond anything from a health perspective (for most). Walnuts are high in omega 3s; whereas almonds are high in omega 6s. After the cookbook publishes and I have a moment, I’ll publish a muffin recipe! 🙂
Dorothy says
Thank you for taking the time to respond in spite of the time crunch. ? I’m glad we don’t need to soak white rice. I’d probably choose it over brown rice for now because of the high level of phytic acid, though soaking does help. I may try adding a little fat while cooking as well. Apple crumble or pie sounds great, and I have a gluten free stuffing recipe that’s pretty tasty. I don’t know whether it would be best to have sourdough yet. That would be organic white wheat, I believe? I’ve been mostly gluten free for some time now, and don’t know how my body would react to having it. We used to consume large amounts of wheat. We ground our own and used various methods, including sprouting, sourdough, and sifting to minimize phytic acid. I’m glad walnut flour is a good option since the nuts are probably less expensive and they can be soaked, dried, and ground pretty easily. I read earlier where you said it’s healthier too. ?
Another change I’ve heard about recently is that some people on this diet are avoiding onion and garlic and the cruciferous vegetables altogether. I believe it’s because they may interfere with being able to detox vitamin A. So I’m trying to scale back some as onions have been a staple for stir fries, etc. And cauliflower is pretty versatile, but I guess it wouldn’t hurt to avoid it for now.
Megan says
Hi Dorothy, yes, organic white wheat. Yes, we have removed cauli from our diet and scaled back on onion etc. 🙂
Kevin says
Why no coconut besides refined coconut milk? The stearic acid?
Megan says
Hi Kevin, somehow your comment got through unseen; I apologize! Yes, the stearic acid, and also the copper content.
Dorothy says
I should have read over that last comment for typos, as there are many. Please excuse my haste in a sending it before checking it over.
Thank you for informing us about this subject, which seems like it may be an important key to autoimmune issues.
Megan says
No problem!! xo
Dorothy says
Hi Megan, I’m still trying to figure out how to make this work for us while weaning off foods with vitamin A. We like the granulated tapioca recipe, but it seems better texture and taste without a liquid added. This morning I added in ascerola cherry powder, monk fruit drops, and a powdered probiotic. We have two liposomal products which contain natto that I’m backing off of. I have several things to return to the store. Do you have a refined coconut oil product you recommend? I bought a big jar of coconut oil at a good price at Walmart that is “naturally refined organic”, the Better Body Foods brand. It says it contains mct’s. From the reviews on Amazon, some people like it and some don’t. It seems they no longer carry it.
Emily says
Thank you for this!
I have some friends who have been doing ‘red light treatment’ and have noticed that their vitamin a levels have gone down. Have you heard anything about this as a possible aid to detox? Thank you
Megan says
Hi Emily, yes, definitely. You can look into near infrared saunas if you’re interested. I like this company best: http://bit.ly/near_infrared_sauna
Emily says
One other question:
Since beans and rice should not be re-heated and beans especially require soaking etc before cooking. Do you have any tips on how best to cook for just one person?
I find it difficult to cook only enough for myself and yet have it as often as I will need to all while working a job with extensive travel. I don’t know how to manage it without some reheating involved. Any suggestions will be helpful. Thank you!
Megan says
Sure. 🙂 Sometimes the best way to start is just to start with what you can improve, and then keep making modifications to get one’s diet lower and lower in vitamin A. I actually started that way myself as I figured it out. Every improvement or discovery is one step in the right direction. I believe Genereux himself did reheat beans and rice, so resistant starch affects some people more than others. And for some, the initial detox stage won’t last long. My kids and husband all eat reheated beans and rice now, and I am just beginning to. But you can use more tapioca flour and macadamia nuts, for example, to make muffins and baked goods that can be frozen for travel. You can do Applegate Farms turkey with iceberg lettuce. Meats can be reheated of course, so bringing leftover burgers and chicken will work. Celery sticks, dried fruits, certain fresh fruits (like apples with a peeler), macadamia nuts. When we travel for our son’s basketball, we bring a hot plate and a small slow-cooker. I cook rice overnight, and we eat it warm the next day/morning. We bring a small skillet for burgers, egg whites etc. We bring our cooking fat and just make ourselves at home. If you start with these kinds of ideas and determination, it’s very doable. For just one person, you can get a small crock pot and also buy an insulated thermos to keep breakfast leftovers portable and hot until lunch.
Emily says
That’s all very helpful thank you!
I have a friend who has been doing red light therapy (not just infrared) and his labs show that his vitamin a levels have lowered dramatically too so that may be helpful for some as well.
Megan says
Thanks so much for sharing that Emily! I’m sure, very helpful. 🙂
Lianda Ludwig says
Just starting the new eating plan to detox from Vit. A. I have a couple of questions. I’m newly diagnosed with Meniere’s Disease (thankfully without the dizzy symptoms) but Tinnitus has become so loud and pressure in my right eat has made me lose my hearing on the right side. Do you think this diet will help? (I have other auto-immune as well).
Is your cookbook focused on removing Vit. A and following the eating plan of Dr. Garrett Smith and Greg Genereux? Does it follow other restrictive eating plans as well- or just the ones mentioned above?
Thanks for all the information on this site. It gives me some hope.
Megan says
Hi Lianda, I’m sorry for your symptoms and happy you are considering the VAD diet. I also had Meniere’s, many years ago now. My doctor put me on B6 and ginkgo biloba, both of which helped until it went away entirely. I can’t say to what degree the VAD diet will help, but I am inclined to say from my experience that its effects are likely helpful for many conditions. My cookbook has been officially recommended by Grant Genereux. 🙂 But the diet will continue to evolve slightly over time as more is understood about specific foods and how they affect our bodies. So you may need to sub an ingredient in a VAD recipe. I was able to make revisions to the book after cauliflower was removed, but there may be other subs that are needed in certain recipes, if you follow Dr. Smith’s updates or Grant’s insights. You can always email me if you have any questions about ingredients. In regard to other diets, the cookbook provides 80 recipes for several wellness diets, including AIP, GAPS and Keto, and most are Paleo. Many recipes include all the diets, but there is an Index in the back of the book for each protocol and the recipes that fit that diet. I’m happy you are feeling hopeful!! Much love and best wishes as you seek relief and healing.
Lianda Ludwig says
Thanks for your encouragement! I’ll definitely get your cookbook.
Megan says
I’m so glad. Best wishes!! 🙂
Ria says
Thank you so much for all you do. ?? My question is regarding Vit C. I’m taking the sodium ascorbate non GMO for recurring herpes outbreaks ?.why do you say not to take it? I think it’s made from corn (not ideal, I know) but it’s been helping, I think. I also take camu camu, and get why you wouldn’t include that.
Ria
Megan says
Hi Ria, you’re welcome! I am not a doctor and can’t comment on your health in particular. If something is working it may be fine to continue, but a supplement may also interfere with the detox of vitamin A in various ways. It would be great for you to tap into either Dr. Smith’s forum or Grant Genereux’s Discussion. They are the ones leading this investigation and researching the specific mechanisms at work in the body and which foods and supplements interfere and why with vitamin A detoxing efficiently. I go off of their recommendations. Occasionally I have my own insights because of my own doctor or health (such as with tapioca), but for the most part, they are better authorities. Typically if something isn’t allowed it’s because it interferes with the goal of this temporary diet.
Ria says
Thanks Megan, Grant emailed that the Vit c may, in fact, be helpful, however he doesn’t feel he needs it.
Courtney says
Hi thank though for this article! I have been seeing a holistic dr and I had recently had my skin turn yellow orange mostly on my hands and feet and I was told I was eating too much vitamin a. I am waiting on blood tests but I noticed the chlorella supplement I’ve been on since November is high in vitamin a. I stopped taking it, but I read that the vitamin a Carotenosis is harmless but now I’m reading this article. Should I worry a little more about toxicity and bring it up to the doctor?
Megan says
Hi Courtney, it’s great your body told you! Symptoms are usually a good thing when they help us to seek answers and switch directions. 🙂 It would be great to mention to your doctor. Vitamin A toxicity, both acute and chronic, are acknowledged medical conditions. How open your doctor will be to the concept of allowing the liver to detox vitamin A through diet is hard to say. Most practitioners still believe that vitamin A is harmless. If you’d like a doctor to assist you in your process, you can also consider Dr. Smith, as mentioned in the article, from Nutrition Restored. Or my doctor is actually supportive of the concept and has helped me with the diet. I also love Grant’s website and the Discussion there. Best wishes as you decide how to navigate.
Michelle says
Why on this detox is vit c supplements avoided?
Megan says
Hi Michelle, opinions differ on using Vitamin C during the detoxing of vitamin A. Genereux at this time, I believe, feels it may be okay, but doesn’t use it himself or claim to know for sure. (He is very humble as he continues his research.) I believe that Dr. Smith says to avoid C. I used to take it but stopped. Because these two men and many others are still trying to understand all of the pathways and interactions that play in, the details are unknown. I used to take a tapioca-based C, and my kids took an acerola-based C. Most importantly, avoid citric acid.
Lorie says
This is all very interesting, and I appreciate your extensive info on it the diet. I’ll give it a try to see if it eases some of my many symptoms that match, but I also have oxalate overload, and many foods on the limited food list are high in oxalates. Maybe mostly carnivore is the way to go for me. Though your sausage biscuit recipe looks astounding. Thanks again! I’m sure I’ll refer to this page a lot!
Megan says
Hi Lorie, sounds like white rice might be a good staple for you too. I think most of us have to make modifications until we get over food sensitivities. I know for me that this diet helped me to overcome food restrictions, so now I can eat more foods that formerly I could not. Best wishes!
Carrie says
So much to take in, thank you, Megan!! I’m feeling the pull to go in this direction, and believe it could help. Question… in a comment above, you responded, “Most importantly, avoid citric acid.” I’m thinking the citric acid that’s found naturally in citrus fruits (like lemon and lime, which are on the ‘low-or-no-Vit. A’ list (YES list), so a little confused… but are you meaning the manufactured, powdered form? I can see that oranges and grapefruit don’t make the YES list. I’m wondering how this diet is working for you currently (since beginning last spring)? I can see you’ve updated it this year, so assuming you’re still detoxing. I’d read on another reputable/science-based blog about a family who’d learned (after a year on this diet) that they now had quite severe vit. and mineral deficiencies, despite trying to do it correctly. Is this avoidable, and how have you known how to best proceed over this last year? Thank you for your tremendous researching, and for your faith and courage to jump in, and then share!
Megan says
Hi Carrie, that’s right, avoid citric acid in processed foods (used as a preservative) and in supplements. I think I know the blog and family you’re referring to, and I think they added in a lot of foods early (too early) out of fear of nutrient deficiencies and compromised their process as a result. As far as real deficiencies, it’s a great time to be on the diet now because increased understanding has continued to improve the process: usually a B complex, foods rich in certain B vitamins or specific B vitamin supplementation is necessary. There are other advisable supplements as well, such as zinc and food-based nutrition, such as broccoli as it helps phase 2 detox. By following either Grant’s blog Discussion or Dr. Smith’s you’ll be able to see what others are doing, ask questions and know the latest insights. If anyone is particularly concerned about deficiencies, Dr. Smith works one on one with patients. A good friend of mine is working with him and has seen huge strides in her health that she’s sought after for years. She really appreciates him. Personally, I can’t say enough good things about this diet and how it’s helped me. I have added in various modalities along the way, as needed. I use Lifewave energy patches, I take a mineral complex, a B complex, Calcium D-Glucarate (not advised by Dr. Smith but I work with a doctor in town, and she and I like it for me), for K2 we eat more butter than what’s recommended, vitamin D from the sun etc.; I do infrared saunas twice a week as well as other methods that aid detoxification. Lastly, I’ll publish a post this week about using gentian or ACV with activated charcoal which has been key for both my son and me with detoxing and preventing acne. I learn how to proceed through the process itself, research and following the discussions, as mentioned above. You really do learn as you go, and there’s plenty of support available. Thanks for your great questions, and I’m happy to help if I can as you begin and progress!!
Carrie Olson says
So helpful, Megan, THANK YOU!!
I read in your article that Genereaux himself supplements with B vitamins and zinc. I see your link to the B-complex you use (minus Vit. A), thank you. Could you also link which zinc product you now use?
I use Nature-throid for my thyroid… do you know if any of the ingredients it contains would be implicated in Vit. A toxicity? Have you found your thyroid issues to have improved on this Vit. A detox diet?
Again, thank you! 🙂
Megan says
Hi Carrie, I’m so glad it’s helpful! 🙂 Unfortunately zinc supplements are in short supply with the virus right now, because it’s an important nutrient for the immune system and deemed helpful with this virus in particular. Here’s the one I buy: https://amzn.to/3aKf9ik, but it is sold out. However, I actually alternate between taking a mineral complex some days and just selenium and zinc other days, and the good news is that the mineral complex I take, which contains the same amount of zinc IS available: https://amzn.to/2X3fo3L 🙂
Regarding Nature-Throid, that’s the one I used to take, but I am indeed well now, with super low thyroid antibodies and good energy etc. So yes, the diet has helped me with my thyroid as well. It’s very encouraging to progress away from Hashi’s after taking thyroid for years. It is, of course, important to stay on thyroid as long as you need it, because it aids your wellness process until you and your doctor think your actual thyroid is ready to take over the job again.
Blessings!! 🙂
Kristen says
Hi. You say in the paragraph above that food-based nutrition such as broccoli is advisable as it helps phase 2 detox, but isn’t broccoli on the “no” list? Was this question perhaps answered before broccoli was removed from the VAD diet? I’ve been on the diet for just a week so far and have seen a massive improve in my histamine intolerance symptoms. This blog post has been a life-saver! Thanks!
Megan says
Hi Kristen, you guessed correctly that because the diet has evolved, that is no longer known to be true. So, no broccoli on the diet. I am SO happy to hear of your improvement! I love how much this diet helps histamine issues! So glad you found it, and my pleasure to help!
Cindy says
Oh gosh, where to begin…. I just “discovered” you and your web page a couple of months ago. This article of Vit A doxcity is amazing and so timely for me!
I was diagnosed with Lyme Disease last July, symptomatic for over a year before that dx. Before that I was dx with Celiac (or “just about there”) and Hashimoto’s. Both of which are now in question, possibly just effects of the Lyme. Needless to say, I’ve seen several different doc’s, and am now seeing a ND, whom I have a fair amount of confidence in—however! he has me taking a daily high daily supplementation of Vit A, I believe he feels it is supportive of the liver in detoxing!! So you can imagine how mind-blowing this article is for me. I live in a fairly small town so I don’t have an abundance of medical choices, and I like this ND, so think I’ll just stop the Vit A supplements.
I actually started with with a FNP who had me on antibiotics for over 6 months, with zero benefit, so moved over to this ND. I’ve been treating with him for oh maybe close to two months now, and still waiting to see a noticeable improvement. I’m really leaning towards a keto diet to see if that makes a difference. Honestly, I’m growing weary of trying this, then trying that, but I really have no choice, I just have to keep experimenting until I find “something” that makes a difference in my health.
Anyway, I know I’m starting to ramble here, so perhaps this is just to say thank you for ALL the research you do and share with us! It’s nothing short of amazing! I’ll have to re-read (then re-ready again) this article and may be back with specific questions. Thank you, thank you, thank you!!!
Oh, wait, I did have one question…on vitamin B, I thought one needed “intrinsic factor” in the B complex to help absorption? Your thoughts?
Megan says
Hi Cindy, Thank you for your kind words, and I’m so glad this was helpful. I’m also sorry for your health struggles! If you don’t make good progress and see improvement with your current doctor, you might consider Dr. Smith, who might be able to guide you through a Lyme protocol while also helping you to detox vitamin A. It is indeed easy to do a Keto-low vitamin A diet combination, as long as you stay away from all the cheese recipes. But butter and certain animal fats work well, as well as oils like avocado, olive and coconut. But ultimately, Keto may make less of difference than you figuring out how to address one issue after the next in regard to possible toxic load issues — with herbs, binders, detox modalities etc. These are big themes in today’s world, so don’t feel alone as you search for solutions! 🙂
Re B vitamins, the complex is utilized fine, but if your body doesn’t make intrinsic factor, you may be a good candidate for injections of B12 specifically. I give myself a shot weekly. I used to be scared of needles, but now I actually feel empowered 😉 ; it’s not hard and does the trick. Best wishes and much love!!
Susanne Rieth says
Any insight into why pork is excluded from the diet? Is it higher in vitamin a than other meats ?
Carrie says
Hi Megan,
I’d like to purchase/store a larger quantity (maybe 10+ lb. bags) of some organic, well-sourced rice, instead of just ‘piece-mealing’ from store bins, from time-to-time. You always have the best recommendations, due to your researching prowess, thank you! Also, I remember you mentioning you can’t have beans, but wondering if you may know of a good source for purchasing dried beans (above you referenced ‘pinto, black, kidney’), also in large quantities?
You’ve listed peeled potatoes (not yellow) as ‘Low VA,’ and I’m wanting to clarify if you are meaning yellow-fleshed? We often eat ‘red’ potatoes (and sometimes ‘huckleberry’/dark purple-skinned) potatoes, both of which have yellow-flesh, but are those no or low in vitamin A? Also, is detoxing through bathing with epsom salts/baking soda/ACV still a good practice while on VAD?
One more question from another, recent post: with ACV being ‘prebiotic,’ (and I know you mentioned it was recently deemed safe on VAD), can using it daily for the combined activated charcoal detox drink daily be used only so long? The NOW charcoal powder, from coconut husks, w/coconut products being on the ‘no’ list, are the husks okay, or would bamboo or another charcoal also work? (the NOW products says to use for a limited time, but I know you referenced continued use being safe). I fully trust you and your research, thank you again!
Megan says
Hi Carrie! Regarding bulk beans and rice, I source them through Hummingbird Wholesale, here in Eugene, OR, but because of the shortages with the current virus scare, they have had to close their doors to foot traffic. You might check Azure Standard. Currently they are out of stock in all their rice, due to everyone stocking up/hoarding 😉 , but they do still have beans, and hopefully they’ll get rice back in stock: https://www.azurestandard.com/ Personally, I’ve been getting three pounds of organic Basmati rice at Trader Joe’s at a time ever since the shortages started. Re potatoes, only organic peeled Russet potatoes are low in A, so no yellow-fleshed or others.
Re ACV and charcoal, I personally feel safe taking charcoal long term. I may likely scale back to every other day once my detox of A is complete. But I feel safe using activated charcoal (1 capsule daily) for 1 to 2 years … safer than I’d feel without it! because it’s adsorbing all the toxins my body would otherwise be wrestling to usher out. I don’t believe that coconut husk-based charcoal would harm us, since it’s adsorbing A, not releasing it, and it’s not coconut essence. (Even coconut water and coconut sugar are allowed on the diet.) But other sources of activated charcoal are fine too. Taking ACV with charcoal is complimentary to this diet. ACV does not seem to complicate vitamin A detox at all, as other prebiotic foods do. Happy to help! 🙂
J Lee says
Hello?
I accidently stopped by this site and learned so many things…
I think I got overdosed with Vitamin A while taking accutane back in 2013 and ever since then I have had long term side effects such as joint pain, muscle& bone problems, and shortness of breath. I am quite sure that all these symptoms resulted from me taking accutane but doctors have no idea how this could be related….
I am just wondering if these side effects could be cured by following the Vit A detox method… Or do I have to live with these symptoms for the rest of my life… I am desperate to find some answers… Thank you so much. I look forward to hearing from you.
Megan says
Hi J, I can’t speak about cures, but I can say there’s a great online community of others on the diet who also took Accutane. You can plug into Genereux’s Discussion and blog here: https://ggenereux.blog/ You can also reach out to Dr. Smith at NutritionRestored.com. Certainly people are recovering from toxicity through the diet.
Anthony says
Just curious to know if anyone has tried a Liver detox to see if it’s a Liver issue or a Candida cleanse?? I’ve been researching many many hours and days to find out why I am having such a difficult time with Histamine, Lectins, Nightshades, Dairy..etc.. With body temperature issues and skin problems
Kirsten says
Hi Megan- don’t know if you ever check back here anymore, but I was wondering- are coconut aminos allowed? Thanks!
Megan says
Hi Kirsten, yes and hi! I always try to answer all my comments on all posts! 🙂 Yes, coconut aminos are allowed. Blessings!
Kirsten says
Awesome – thank you!
Kirsten says
Hi Megan, I just finished reading Grant’s first book and I was wondering if he still recommends supplementing with taurine? Thanks
Kirsten says
I was also wondering if lemon balm, roasted dandelion root, and rose hip tea are okay?
Megan says
Off the top of my head, I am remembering that dandelion root is okay, and that lemon balm and rose hip tea are not.
Kirsten says
Okay, thanks!
Wavy says
I question whether stearic acid is enhancing the problem, or whether it might in fact be speeding the recovery process. Saturated fats are the healthiest fats for humans – they’ve been wrongly vilified for decades and recent research is finally showing that they are healthy. The fats containing the most stearic acid are the most saturated with the fewest amount of unsaturated fats in them, and it is in fact the unsaturated fats from plant oils, and to a lesser degree from grain-fed chicken and pork fat, that promotes oxidative stress in the body. Thus, the more stearic acid a fat contains, the healthier it is. Plant oils are the most harmful to us.
After reading Smith’s blog entry at the link you provided, I’m left wondering what the mechanisms are for Vitamin A to leave the body. To me, it sounds as though stearic acid is binding with Vitamin A in order to SAVE our organs and tissues from free-floating Vitamin A, and usher it back to the liver which is where the processing of the Vitamin A is SUPPOSED to take place. Isn’t the liver where Vitamin A is conjugated by taurine, and thereby “detoxified”? And where is the most taurine found? In muscle meat of ruminants, as well as other animals.
I do find it hard to argue with mountains of personal experiences that all point in the same direction…if hundreds of people report feeling worse when they consume beef fat, it would seem there is something to that. But maybe are they feeling bad because the Vitamin A is being released from storage in the tissues as part of the “detox” process? As someone who has struggled with oxalate overload in the body, I can tell you that the removal of stored oxalates is more painful than their initial accumulation, and I would think the process of removing stores of Vitamin A could be similar.
From an evolutionary perspective, there’s a lot of evidence to suggest that humans relied on large mammals for food for a very long period of time before the relatively recent advent of agriculture, and our digestive tracts and bodies are in fact designed to thrive on the muscle, fats, and organs of terrestrial mammals. If that is the case, it would make the most sense that by eating the way we evolved to eat, our body is doing what it is designed to do by having stearic acid shuttle a toxic element back to the liver, which our detoxification organ.
cis says
Frankly NO!
I have always assumed that
1) I am vitamin A deficient, if anything
2) natural carotenoids from foods are not an issue for most people,
and certainly for those that have trouble converting them to vitamin A.
How did you come to be vitamin A toxic? Long-term supplementation?
Regards,
cis.
Megan says
Hi Cis, yes, I did supplement with liver pills for years. Thanks for sharing your opinion. This article and diet definitely challenge what so many of us have always assumed about vitamin A.
Frances Arnold says
Your article is informative and eye-opening. Thank you! I think it’s also important to make the distinction between Provitamin A foods, such as those found in plants, and the pre-formed vitamin A foods, such as liver. As well, many people lack the genetic ability to efficiently convert carotenoids into vitamin A. So, for those of us with this condition, I would expect that we are far less likely to develop toxicity unless supplementing with pre-formed vitamin A. Just thought this would be an important distinction to make in your already great article. =)
Alex says
Hello Megan,
Thank you for the information you are posting. This has been a blessing to me and my family in trying to recover from our health issues.
I was wondering if you know if 1. chamomile tea, 2. hibiscus tea and 3. Tulsi Moringa tea (combination of moringa leaf, lemongrass, holy basil and Indian basil) is ok on this diet.
Thank you.
Megan says
Hi and you’re welcome. 🙂 I’m so glad the information is helpful, and best wishes with your health journeys. None of the herbs you named are okay for a low-A diet. We do enjoy rooibos (my youngest son does), so it may be fine. We also drink green and black teas and make jun and kombucha with them. And hot chocolate can be made with carob, if that’s helpful. Also mint tea.
Kristen says
Is Milk Thistle tea ok on VAD? I was thinking it might be helpful with liver detox and whenever I was experiencing histamine symptoms, it always calmed them.
Megan says
Yes, happily, milk thistle is allowed.
Alex says
Hello Megan,
Thank you for answering my tea questions! I am excited to be trying the rooibos tea. 🙂
I have a few more questions, if you don’t mind.
I am (age 51) doing this detox diet with my 19 year old daughter. We both have health issues. I have Hashi, chemical sensitivities, food and pollen allergies, bladder urgency, weight problems, etc. and have used Accutane several decades ago for persistent acne. My daughter has rashes, eczema, keratosis pilaris, food/chemical/pollen allergies, and bladder urgency issues, among others. We have been on the vitamin A-detox diet for about 1 month (doing only animal proteins so far and a little scared to try other foods) and are starting to see results! I am actually losing weight and I have been unable to do so no matter how hard I tried on many previous diets and eating plans. 🙂
My questions are:
1. When is it a good time to start experimenting and add items that I avoided for years on the paleo diet (rice and other foods on the “yes vitamin A-list”) into the diet? Is it when most symptoms are gone? And what symptoms do we watch for to make sure the new items are ok for us to eat – weight gain, headaches, return of old symptoms? How much time between new food introductions?
2. When you eat rice with a little fat, is it ok to add protein such as chicken or beef or is it best to eat carbs separately from proteins?
3. Are you foreseeing that eventually, when hopefully detoxed and symptom free, one could add more vitamin A-List colorful vegetables back or is it a bad idea?
4. Is xylitol allowed at some point?
5. What herbs and spices are allowed?
6. What supplements helped the most with detox?
Many thanks.
Alex
Megan says
Hi Alex, happy to help! 🙂 It’s probably a given, but just to be safe, I’m happy to share what I did and do, but I don’t want to put myself in a position of giving advice because I’m not a doctor. So, I’ll share my experience, and then you guys can decide what’s best for you. Personally, 1) I started white rice as soon as I thought my gut could handle it (after years of being grain-free, similar to you). I also was hesitant and a bit unsure, but it went great. It seems so much healing happened that new introductions went well. I can’t be sure how long I waited, but maybe 2 months? Each of us has symptoms that are unique to us; for me, stomach aches had been a problem; lectin reactions (a rash behind my ear) – so skin and gut symptoms. Rice turned out to be an easy re-introduction for me. Beans and oats took a little longer. With oats, I had to try twice. The first time was too soon, and my lectin-sourced ear rash broke out; then I waited a few months, tried again, and now I eat them daily! Pretty cool. With beans, gas was my issue. I just used Dr. Smith’s advice to go off of the bean chart for blood types, and now I eat beans daily, no problems. 2) I can have blood sugar issues, so I always eat my carbs with protein. I think it’s best anyway, personally. I think of protein as the anchor, and carbs as the side dishes. I think of beans as necessary fiber and a great source of B vitamins. 3) Yes, in fact, I’m starting to do this for my boys: one’s 11 and the other 17. I started by adding back in sources of resistant starch (cassava flour and tiger nut flour). Then I added in occasional pastured pork. Two days ago, we challenged avocado. I don’t plan to buy kale or orange sweet potatoes again, but I do think we’ll eat a broader variety over time. I’ll be doing this diet as-is, though, for many more months before any reintroductions for myself. I don’t plan to eat a lot of super colorful foods in the future, but I won’t advise my boys to stay away from most foods once they’ve detoxed. We’ll just know in the future never again to fortify our diets with those foods or eat lots of them. 4) If you don’t have any GI issues from it, xylitol should be fine at some point. 5) Dill, rosemary, cumin, black and white pepper (if no reaction), ginger (dried and fresh), cloves, peppermint. 6) This could be a longer answer and pretty personal for each person. Dr. Smith and Grant are still analyzing their opinions on this. Certain B vitamins help some people and not others. It’s helpful for many to take something to adsorb vitamin A; for this, I take one activated charcoal daily with gentian root (like this: https://eatbeautiful.net/how-to-daily-detox-activated-charcoal-apple-cider-vinegar/). Zinc is pretty commonly taken. Blessings to you both in your process!
Ariel says
Hello Ms. Megan,
Thank you so much for all of the research you are posting. It has been a lifeline!
My mom and I have had food, chemical, and mold sensitivities for years and have gone through many diets and lifestyles in an effort to heal leaky gut and resolve our health issues once and for all. We have tried paleo (with some but limited success), keto, blood type, and now a carnivore elimination diet combined with low fiber and vitamin A detox. We tried your butter tea today for the first time (with the Traditional Medicinals dandelion root tea) and it is absolutely easy and delicious – such a pleasant treat (very different from dropping some butter into tea, as I tried before)!!
I have several questions (apologies for the scope of them):
1) How did you incorporate the blood type diet into the vitamin A detox? For example, you mentioned that your family members eat different beans depending on their blood type. Prior to beginning the vitamin A detox, my family tried the blood type diet (Mom and I are B’s, Dad is an A). In some ways it was very clear – I thrive on fat, my dad gags on it, and we applied it to beans and grains, but did not notice anything when applying it to fruits and vegetables.2) Through kinesiology, it seems like I have a genetic intolerance/sensitivity to dairy (as does my mom). Do you have any opinions on NAET?
3) Do you have a suggestion for a multivitamin without vitamin A?4) Is cod ok to have on the vitamin A detox? On one hand, cod liver oil is high in vitamin A, but at the same time, cod is a white fish, so I am a little confused.
Again, thank you so, so much!
All the best.
Ariel
Ariel says
Also, one more question: Is prepared blanched almond flour (https://www.costco.com/kirkland-signature-almond-flour%2c-3-lbs.product.100438553.html) acceptable for the vitamin A detox, since the almond skins are removed?
Thank you!
Megan says
Hi Ariel, that blanched almond flour won’t do because it’s conventionally grown (very high in pesticide residue and not grown responsibly). The only almond flour that will work is organic. Here’s the only well-sourced organic almond flour I use or recommend: https://amzn.to/3rWyy8t Best wishes and you’re welcome! 🙂
Megan says
Hi Ariel, great to hear how you’re doing and so glad the tea recipe is lovely for you! 🙂 1) We have only applied the blood type diet to our bean choices. I haven’t found the rest of the information pertinent and don’t apply it to my choice of vegetables. (Although, similar to you, it has given me occasional insights, like that I don’t digest chicken or pumpkin seeds very well.) 2) I have had good experiences with NAET. As long as you like the practitioner, I think it can be helpful. Personally, I would combine it with the concept of food intolerances and stay away from one’s food intolerance in any quantity long term (https://eatbeautiful.net/difference-food-allergy-intolerance-food-sensitivity/). 3) Dr. Smith and Grant Genereux have many good insights on supplements, and one of Smith’s is to take B vitamins separately (or not at all) because not everyone needs all of them and because B6 has been implicated in being neurotoxic. Accordingly, I stopped taking my no-A B complex/multivitamin. I now take all other Bs individually + a multi-mineral which I alternate with taking just selenium and zinc some days. I think perhaps I need to write a post on exactly what I take and eat as an addendum to this article, as others have requested that too, and it’s a bit much to squeeze in here. 😉 4) Cod is not okay. All cold water fish have the risk of being high in A, but the two seafood choices we’ve found to be fine for us, seemingly, are large fresh Atlantic sea scallops and Petrale sole. We have a nice fish market in our town, and we splurge on these once in a while. Happy to help. Blessings!!
Ariel says
Also, one more question: Is prepared blanched almond flour (https://www.costco.com/kirkland-signature-almond-flour%2c-3-lbs.product.100438553.html) acceptable for the vitamin A detox, since the almond skins are removed?
Thank you!
Jesse says
This list is not accurate.
Butter and Ghee are LOADED with vitamin A. Lettuce has a fair amount as beta carotene as well.
Megan says
Hi Jesse, too much butter or ghee are not good on this diet, but the detox mechanisms and processes are complex, and it’s understood that a small amount of butter may aid the detox process in this case. No more than 2 Tablespoons daily is recommended. The additional side benefit is getting food-sourced vitamin K. Lettuce is allowed for a similar reason. Each food that seems out of place has been carefully scrutinized to see how it works in the body to aid or impede the detox of vitamin A.
Alex says
Hello Megan,
Thank you for the detailed answers. I am glad I found your site, as it is full of great research and information. I find myself reading and re-reading your blog posts to reinforce the information. I am planning on trying the gentian and charcoal combo for further detoxing, then taking a break and trying bentonite and maybe DE. Again, thank you so much for answering questions and being so available and clear with your suggestions.
Danielle says
Hi Megan, I have a host of symptoms that have been unable to be diagnosed and a lot of them fall into the histamine intolerance and vitamin A overload categories (horrible GERD on Pepcid for over a year, sensitivity to cold and heat, psoriasis, chemical sensitivity, brain fog, anxiety, fast heart rate etc etc
I don’t want to combine the 2 diets. Which diet do you think is best to start with? Thank you
Megan says
Hi Danielle, I’m sorry for your symptoms and struggles. I can’t give you my opinion on that, because I’m not a practitioner. In your shoes, I would continue reading about both until you feel more clear about what path to take or find a practitioner who can help.
Danielle says
Thank you
Adrien LACROIX says
HI!
What do you think for turnips and well soaked and cooked sorghum (with instant pot)? Do you have good experience with them?
Thanks a loooot!
Best,
Adrien
Megan says
Hi Adrien, Turnips are out. Sorghum is not one of the recommended grains. The grains that are recommended are oats, rice and hulled barley. You’re welcome, and I hope that helps!
Ariel says
I have been on the carnivore diet for 2 months, salivating over the recipes I see on your blog, and am very excited to start introducing new foods (very slowly)! I was surprised how satisfying the meat on its on was, though. Chicken didn’t sit well with anyone in my family, which was unexpected… As I am getting ready to begin the next phase of the diet, I come armed with questions:
1. How much time would you suggest between new food introductions and within food introductions? Is there a certain way to introduce foods more successfully, such as try a bit of rice on Monday, no rice for a few days, a bit more on Thursday, etc.? How much time should I allow for testing of 1 food to know whether it’s a “yes” or “come back soon”?
2. I was discouraged when I started the Vitamin A detox at the thought of not eating so many foods, especially since I went the strict path, but am so pumped up while seeing results and learning that this lifestyle isn’t a life sentence but something amazing for my health! I think I’ll actually be able to eat more foods than before… I have seen some delicious recipes with puffed rice. Do you know if it is ok to start with puffed rice when considering resistant starch (for both raw and baked recipes)? Do you have any suggestions for puffed rice products? Do puffed grains have a lot of resistant starch and is that something for later on in the diet?
3. Is it ok to start adding in rice before reaching an ideal weight or will that slow weight loss further?
4. In your research, have you read anything about the Vitamin A detox helping stroke patients? Already noticed a bit of a difference in my grandma’s cognitive condition by removing chicken and feeding her only beef (better and worse, but some improvement). She had a stroke 4.5 years ago leaving her half paralyzed and severely cognitively debilitated. We’ve tried HBOT, acupuncture, homeopathy, etc. If there is the slightest possibility of her getting better…
5. Would you consider creating a post about what your family eats in a day/week?
6. How do you cook around so many different intolerances?
Megan says
Hi Ariel, I’m sorry for the delay in responding. It’s been a busy week, and I saw this response might take an extra few minutes! 🙂 So, typically the rule for reintroductions of foods in 7 to 10 days. Puffed rice is not considered a health food by ancestral dietitians because it’s a high-pressure process of manufacturing that’s not natural. A small amount may be fine in one’s diet, but I’d focus more on actual rice. Also, as you may know, rice depletes B1, so it’s only advisable to eat it if you offset that with plenty of B1 foods such as beans, beef and macadamia nuts. A lot of emphasis is placed on beans for their B1 and fiber, which helps to excrete toxins. Re weight loss, carbs ideally correspond to activity level (https://eatbeautiful.net/carbohydrate-intake-activity-level-weight-loss-blood-sugar-regulation-guide/); so I like to think of carbs in terms of how many walks I go on in a day, or how often I jump on the trampoline, do squats, yoga etc. If you’re not super active, I’d focus more on nutrient dense oats for your carbs, but mostly on beef and beans. Re stroke recovery, at this time, I haven’t read up on that re vitamin A detox. But certainly beef when pasture raised is a better food than chicken, so that’s a great change you’ve made and noticed. What I have read up on is Lion’s Mane. It’s a wonderful mushroom powder that can be used on this diet. Great for cognitive improvement after stroke or with other neural issues. I love it; I take it. My parents take it too. Watch for noticeable improvement at about 6 weeks. (Here’s the one I buy: https://amzn.to/2O7CCne) Yes, I do need to write a post about what we eat! I’ll plan to do that soon. Re cooking for all the family, I just try to keep my mindset very low stress! Everything comes second to that, just about. So whatever we eat must work with what I can manage with a balanced mindset. Sometimes that means keeping meals really simple: burgers, sliced peeled cucumbers, rice and beans. Other times, it means asking someone to help me, dividing duties so I don’t get overwhelmed or too tired. Blessings!!
Ariel says
Thank you for the feedback.
Just to clarify – when introducing a new food, how often within those 7-10 days do you try the food? Is it just once? Daily?
I will read more about the Lion’s Mane. Rave reviews on the link you sent.
Thank you!
Megan says
Hi Ariel, you’re welcome! There are different schools of thought on how much. Personally, we keep eating that food during the 7 days, daily and not too much at a time. For example, a lot of rice or oats or beans is different for the body to digest than a small amount. So a small amount is a more accurate measure of how the body does with that food. I’m glad about the lion’s mane. 🙂
Adrien says
Thanks Megan
I find difficult to just eat grains like rice or oat :(… Do you have some experie’ce with millet?
Thanks!
Best,
Megan says
Hi Adrien, good question. I have eaten a small amount of millet on the diet, but it doesn’t agree with us as well as may not be as good of a choice for these purposes. However, if you’re very intuitive, you might try it to judge how you do. Buckwheat is another option that may be okay. And hulled barley we have recently added in and really like, although it may not be any gentler than rice and oats. Have you tried white rice (vs. brown) and beans?
Adrien LACROIX says
Thanks for your answer Megan! I tried white rice but I’m feeling sluggish when I eat it 😀 I would to try oat in instant pot and see my reaction …I will give you my feed back
Best,
Adrien
Megan says
I’m glad you’re so in tune with your body. Eating a limited diet sure lets us know what exact foods do in our bodies. I hope oats and even beans work well for you! I really like making soaked oatmeal with bean milk, and how I feel after that combination. But oats and beans didn’t always agree with me.
Melissa Gonzales says
Im just now starting my first elimination diet. I have been on a limited diet for years. I have fibromyalgia, IC,endometriosis, mcas and chronic fatigue. I can see very much that food is a culprit. However my last naturopath thought more supplements meant better. Oh no did it NOT! I’m severely malnutritioned as my teeth have deteriorated badly. Lots of expenses have been the scope of the last few years. Several life stress for a decade. Anyway I want to start the vad diet but think I need to nourish my spirits alittle and was hoping that you thought that whole rice soaked,cooked and cooled as well as white potatoes wouldn’t be bad for abit. Manly because of my digestive system being so bad that I need to give it a break. I was eating high nutrient foods and high fiber along with RS. Not so good as ive recently learned. I think that I may have to just be gentle for awhile. Give my mind a break and my system before heading out to experiment with alot of things. Supplements I was probably taking 20 difficult a day. For about 4 and a half years. So vit. A toxicity sounds about right. But probably not the culprit because I went to the ND for so many things. What im asking is that if I can eat white rice and potatoes is that alright for a respite for digestion? Beans I don’t know about. But you never know. I haven’t eaten all three of them in years. The potatoes and the rice SEEM to be ok so far. I’d also like to possibly add the white rice flour and tapioca as well. Any advice I’d appreciate 🙏
Megan says
Hi Melissa, in my opinion, yes. Intuition and listening to your body go a long way. Both white rice and potatoes can be gentle for some people. Not everyone digests them well when eaten in the same meal (I am one of these people, so I always eat them separated by 4 hours or so). The other thing to be aware of is that rice depletes the body of B1, so long term you’ll need to supplement or better: eat foods high in B1 to compensate like the oats, mac. nuts or the aforementioned soaked beans. (<—That link shares how to make beans more digestible.) Also, I approached this diet the same way in the beginning. There's nothing wrong with getting your footing and then progressing from there. 🙂 Best wishes and good health to you!!
Alex says
Hello Megan,
I tried the white rice challenge and it did not go well. I ate 3 scant tbls of cooked organic rice along with my usual beef meal and gained 1.8 lbs when I weighed myself the next morning. I also felt sluggish and had mild GI issues for a couple of days after the rice. I stopped the challenge after that first try. One week later, I tried 2 tbls of home cooked stewed apples (white fleshed apple, peeled, nothing added) with my regular beef lunch. This time, I gained 1.2 lbs the next morning, but there were no GI issues at all. That kind of weight gain is not normal for me, as it usually fluctuates up or down by no more than 0.6 lbs, depending on the day. The Carroll test identified three primary intolerances to eggs, honey and fish and combinations of fruit and sugar. So, theoretically, I should be ok with rice and apples.
I was 40 lbs overweight for years and have been on paleo / keto for many years, but lost only a few lbs on animal protein and veggies, so something was not working well. I have been on VAD, eating only beef for 3 months, and I feel great. The weight has been melting off easily and many health issues are slowly resolving. I am also taking charcoal and ACV as per your blog, but wanted to add a little soluble fiber to my diet to bind to the toxic vitamin A and usher it out of the body. I worry about circulating retinol not binding to bile and not exiting the body. Are the daily ACV/charcoal combo enough to remove toxins?
I read your sugar regulation guide and I do walk daily for an hour and am active throughout the day. I am sure I have insulin issues as I am only able to lose weight on straight meat with no added sugars/carbs, not even vegetables. Based on your experience, do you think that as people detox with just doing the carnivore diet for VAD, it is possible to heal enough to introduce more foods?
If you were in my shoes, would you try the apples or rice again or instead challenge beans and oats slowly to speed VAD and hope the weight might fall off eventually, or would you do the straight carnivore and heal further and try adding soluble fiber in several months? Is there anything else you would do to speed the VAD detox?
Thank you.
Alex
Megan says
Hi Alex! I’m so happy for the progress you’re making with low A and carnivore diets! Great news. As you know, the danger of doing the carnivore diet for too long is being low in vitamins B1 and B2, as well as potassium and sometimes copper etc. Not a huge loss not being able to add in white rice, because yes, oats, barley and beans are much better in terms of their nutrition as well as their fiber’s detox role. Depending on your bowel movements and preventing constipation, you could certainly try adding one more activated charcoal tablet at the opposite end of the day (with dinner or before bed). Another option is to add in apple pectin, which is another great binder and should be/hopefully will be gentle for you, working up to 3 capsules, 2x daily (but start with less), at 700 mg. of apple pectin per capsule, like this one (per Dr. Smith’s recommendation). I do think it’s likely that as you continue with your current diet you’ll be able to challenge beans, oats and barley successfully. (Obviously with beans, be sure to see the bean guide and best digestion and soaking tips. I can see from your trial of white rice that you know to do that slowly, with small amounts.) To answer your last question, if I were in your shoes, I’d supplement B1 and B2 (if tolerated) for the time being, add liquid minerals to all water for potassium and begin daily grounding, if you’re not already, to speed healing. If you live anywhere near the coast, I’d get to the beach and walk on the sand, enjoy the sea, as often as you can for the same purpose, especially in the sunshine. These last two tips are incredibly powerful at rebooting the organ systems and accelerating detox and healing. Then I’d challenge beans or soaked oats. This coming week, I’ll publish a bean and oat waffle that may work well for you in the future; it has a sourdough option that makes it extra digestible. So yeah, avoid the rice and apples for now, IMO. Lastly, per Dr. Smith’s forum, he says that some people do better on whole oats and whole barley, instead of rolled oats (oatmeal) or rolled barley, so to trial these to see what’s best for you, when the time comes. One thing I haven’t written about yet, that you may already know, is that to truly properly soak oats, it’s best to add a low-A, gentle grain that contains phytase, the enzyme that oats lack, to break down oats’ phytic acid. This just means, for our purposes, adding 1 to 2 tablespoons buckwheat to your soaking oats with the apple cider vinegar and water, for 12 to 24 hours. Phew! 😉 Well, that covers a lot, but let me know if I left something out.
Alex says
That was a lot of information and I am truly grateful for all the wonderful advice. I will start implementing! Thank you so much!
Nicole says
Great article! I heard about this diet online from Dr Garrett Smith about 5 yrs ago? I’m still in the same mental space of “screw all diets unless it causes immediate severe pain”. I’ve been on diets since food was introduced as a baby. Im done with it all beyond non organic, no dairy or gluten and some random intolerances.
But I do deal with chronic illness, stuck on Ketotifen for MCAD to eat and desperate but I just can’t do another diet – I can’t.
When I was a teen I turned slightly orange from too many sweet potatoes, I still love therm. Later I learned I genetically don’t convert beta carotene to Vit A (or maybe at a very low low efficiency)- is this a good thing or work against me? I also don’t detox Alcohol properly lacking enzymes (severely intolerant to even smell it) and take dehydromyciten to help. Does this work for A detox or against? I’m curious if there are any genetics that could be red flags to know if this is an issue for a certain segment of people.
I guess I’m hoping in time we don’t have to do this extreme restrictive dieting (especially if you struggle with foods in the safe list). I’d love to know if there is anything one can do that doesn’t involve as restrictive dieting, saunas? Detoxing or inhibiting uptake? Just a hopeful thought if this theory is accurate and not related to another variable.
Ashley Zappe says
This is VERY useful information. I wish there was some sort of step-by-step program so I’m not trying to understand everything about vitamin balance all at once. I wanted to let you know, though, that I’m having a very difficult time reading it because the ads are so flashy and always moving; it’s very hard to concentrate. Thanks for writing this!
Megan says
Hi Ashley, thanks for commenting. If you’d like a step-by-step program, I recommend you reach out to Dr. Smith. He does that for his clients! 🙂 I’m sorry about the ads. They are part of what allow me to work full-time on my blog. I try to ignore them and over time that works pretty well for me. Best wishes, and you’re welcome! 🙂
Brent says
Butter and ghee are high in vitamin A I thought?
Megan says
Hi Brent, too much butter or ghee are not good on this diet, but the detox mechanisms and processes are complex, and it’s understood that a small amount of butter may aid the detox process in this case. No more than 2 Tablespoons daily is recommended. The additional side benefit is getting food-sourced vitamin K. Thanks for the question.
Tiffany says
Wow. First, thanks for this info, your recommendations/info on Smith/Genereux and to your readers for supporting this helpful dialogue. I hope my input will help others too – sorry in advance for the long post!
I’ve spent the last 6-7 years researching my failing health full time with no answers. I’ve seen countless doctors, ER visits, tried almost every detox including now low oxalates with Sally Norton and eating more carnivore (guess I have to eliminate egg yolks which sucks), grounding, and have gotten sicker and sicker. I’ve lost my career, friends and most recently my relationship of 12 years. I can’t tell you the depths of despair I feel of health/life.
I tested deficient in Vitamin A and have the MTHFR/COMT mutation, so my doc put me on cod liver oil in 2019 and diagnosed me with mast cell activation. I took until I got skin burning (same with beef liver previously). Unfortunately I’ve since been taking both thinking I was deficient, in addition to a high retinol diet. My long list of distributing symptoms mirror Dr. Smith’s monster list. Here’s the link if it helps others: https://nutritionrestored.com/blog-forum/topic/the-mega-symptom-list-of-poison-vitamin-a-toxicity-and-detox-symptoms/. Many days I’m bed ridden … I was previously athletic and now feel advanced aging and decrepit. All my other blood tests appear “normal,” except for low T3. How’s that possible, I have no idea. Dr. Garrett says a vitamin A deficiency could really be protein/zinc deficiencies. Wow. Guess things aren’t always what they seem.
One of the biggest outward symptoms is hair loss (85% of my hair is gone). Devastating. Odd things make it worse like salt, vinegar, lemon, etc. No idea why. PH issues or detox? Despite genetic mutations that don’t allow me to convert carotenoids into A, juicing carrots and kale caused mass hair dumping and sweet potatoes would give me anxiety. Could be oxalate issues as well vitamin A toxicity?
You mentioned supplements may interfere with detoxing, but that some will help. I am taking Pure Encapsulations methylated B12, B6, folate, biotin, Klaire Labs benfotiamine, Biosil, potassium bicarb for oxalate/PH recovery (bad idea for digestion/taking with lemon/ACV?). I would think to get calcium levels down that taking magnesium would make sense? Like Epsom salt baths, magnesium oil, magnesium malate, and Anderson Sea mineral drops? I have awful night sweats … would be nice to think it was vitamin A detoxing?
Have you heard of Dr. Chris Masterjohn? He says that you need to include all other fat soluble vitamins to balance and detox others. Just thought it was interesting: https://www.youtube.com/watch?v=vTB-yuCJZm4
Some other questions:
–Why are some things high in A allowed like cherries, but arugula isn’t which is a lot lower?
–I saw olive oil isn’t include but is referenced in a comment as being ok? Esp being high in E and helping release A?
—I’ve read ACV can affect bone/mineral health. Is there an upper end to how much to take daily safely?
—I was using tallow soap, including for hair. Bad idea? I’m sensitive to so many scents, additives, etc. in soaps/shampoos.
—Are sardines in water ok?
—Have you heard of the Ion Gut Health? It’s supposed to protect against glyphosate: https://ionbiome.com/products/ion-gut-health In the past it’s caused hair dumping, but wondering if that’s a detox symptom?
—Thoughts on bee pollen?
—Why isn’t pork allowed?
—I tried clicking on your infrared link, but it doesn’t appear active.
I will continue to read through your blog and Smith/Genereux’s. Endless learning to wellness. It seems the more I learn, the more questions I have!
Thanks again for everything.
Tiffany
Megan says
Hi Tiffany, I’m sorry, it would take too long to answer all your questions, but I’ll try to answer most! 🙂 Thank you for sharing where you are, and I’m sorry to hear of your health struggles. I think you’ll find the rest of your answers through careful reading here or in the other two forums (Grant’s or Dr. Smith’s). Cherries are no longer on the Yes list; that changed recently through Dr. Smith continually refining the program/diet. If a food is allowed, like berries, it’s because the body benefits from the food and/or does not store A from it. The food may actually have compounds that assist with detoxification, or the benefits outweigh the VA. Dr. Smith has looked into each food very closely. Occasionally I update this post when new discoveries are made accordingly. Olive oil is okay if it’s not extra-virgin. Small amounts of ACV, but there is still discussion on this. Your soap may be fine if you don’t react to it; watch and see how you do once you’ve begun the protocol. Some people react to stearic acid more than others. No sardines, says Dr. Smith. No on bee pollen. Pork is high in hidden retinoic acid as well as stearic acid. I don’t see the infrared link you are referring to; can you tell me where it’s located in the article? Thank you for letting me know about it. 🙂 Blessings in your process!!
A says
Hi, is it ok to drink Yerba Mate tea (in moderation) per VAD? It has caffeine but seems to have wonderful benefits.
https://www.organicfacts.net/yerba-mate.html
Megan says
Hi there, and I’m sorry I missed your comment until now; it went to another area in my back end than my usual comments. No, yerba mate is not allowed on the diet. Occasionally, it might be fine, but not often. Anything that’s high in polyphenols slows down the process and depletes B1. There’s more, but that’s the short answer as to why not.
Alex says
Hello Megan,
We have been on the VAD diet for almost 11 months now and are going strong! I wanted to ask your opinion about rice protein powder, to add to smoothies, just for variety since we are still pretty limited with food options. It is a brown rice product that is treated with enzymes and I know that we are not supposed to eat brown rice, but wonder if the enzyme treatment takes care of the lactic acid or if I can add oat yogurt to the powder overnight and neautralize the lactic acid and then add it to a smoothie in the morning?
Also, wondering about a product I came across from Designs for Health called WheyCool, which is grass fed whey protein – https://www.amazon.com/Designs-Health-WheyCool-Unflavored-Unsweetened/dp/B00EEEFW1K
Would this product, occassionally and in moderation, in smoothies, be ok at this point in the VAD or at some point in the future? Maybe as a cheat breakfast once per week?
Would appreciate your thoughts on these two questions.
Thank you.
Alex
Megan says
Hi Alex, happy to help. On Dr. Smith’s website, he talks about whey as inhibiting the DH system, or the body’s ability to detox VA. It also may be a carrier of A, so makes it recirculate. Re the rice protein powder, I really don’t know for sure. You could try it mixed half and half with collagen powder. I have actually had the same need for my oldest son who is an athlete and needs to get in a lot of food and protein, and it’s best if one of those meals is convenient. He makes himself berry smoothies with this beef protein-based protein powder, which is the best option I could find: https://amzn.to/3jvewzi It’s very good, but it is a small compromise. I don’t recommend the yogurt option because of aldehydes from yogurt. I was marking some of my fermented recipes VAD-friendly because I overlooked the issue of aldehydes. I don’t think the overnight ferment is ideal. Grant himself has eaten a lot of brown rice. So, I’d choose the best protein powder option based on your instincts, and then see how your body does with no other changes to the diet.
Alex says
Sorry, meant to write phytic acid. Brain not working today….
Alex says
Hello Megan,
Thanks for the response and explanation. Do we also have aldehydes from homemade oat yogurt?
Thanks.
Alex
Megan says
Hi Alex, sadly, yes. After I finish up the article I’m working on today, I’ll go in and begin updating this post and other recipes I’ve labeled VAD without aldehydes in mind. I hope I haven’t derailed you. I do think it’s slowed us down in small ways or caused small flares. We’ve just pulled back strictly ourselves this week, and I’m looking forward to seeing the gains from that. I find that I’ve been so grounded in WAPF thinking, it’s very hard to rethink fermented foods during the VAD diet. Very hard for me. Let me know if you need help finding additional new foods to add in. We’ve added a few in having to remove a few, and I hope to write a post soon that includes everything we eat (and supplements).
Alex says
Hi Megan,
I was so excited about the oat yogurt recipe and being able to ferment flour (from allowed grains) to finally make bread. 🙁
However, I do value all the information you are putting out for us and I understand that as new facts comes out, you are updating posts and letting us know. It is all very much appreciated! I would love to know more specifics of what you do eat now (new foods, supplements, recipes, etc.)
Thanks for all you do!
Alex
Megan says
Thanks, Alex, for your grace. In general I’m so thorough that I surprised (and disappointed) myself by overlooking this. I’ll be working on that post. Can you tell me in the meantime what your current Yes foods are? I may be able to add a few ideas for you based on what I know you can eat. Curious where you are with beans, nuts and seeds, parsnips and frozen cassava roots right now. Cheers! 🙂
Alex says
Hello Megan,
We would welcome any suggestions! Thank you! We are now eating beef, turkey, white rice, oats and buckwheat and they are wonderful! We could not have grains in years and are very thankful for the delicious soups, stews and porrige we make with these combos. My daughter can also have raisins and stewed, peeled, white fleshed apples. Occasionally, we have parsnips, although it has been challenging to find fresh ones that are not old or moldy in the grocery stores and I have not seen any in the farmer’s markets I visited. We have tried beans and thought we could have them, but that did not turn out well for us long term. We also have had GI issues with soaked and baked crispy almonts, and to a lesser degree with walnuts, so we brave a few crispy walnuts here and there because they are absoluty delicious and sometimes we just want something delicious and different. We never tried cassava because according to the Carroll test, my daughter cannot have any potato.
Thank you.
Alex
Megan says
Hi Alex, I’ve spent the last week updating this post and just republished it. So please feel free to read through it as you have time to grab the foods I’ve added or taken away, as well as other notes. It is difficult to sift through all of the changes that have happened with the diet in the last year, but very rewarding. The most exciting recipe I’ve figured out lately uses parsnips. I wonder if you’d be able to contact a company like UNFI to buy a box directly from them, depending on where you live. Or another similar supplier. I’d try to find organic bulk parsnips. If you’re able to, I have taken my bean and rice waffle recipe and subbed cooked parsnip and zucchini purees in for the rice and beans. The recipe works and is great. If you get your hands on parsnips, let me know, and I’ll share the specifics; otherwise, I plan on publishing the recipe sometime soon. Can you have carob, and have you tried the Carob Muffin on the site?; it has a potato-ingredient, that I’d be happy to help you work around so your daughter can have them too.
Alex says
Hello Megan,
Hope you and your family had a lovely Thanksgiving!
Thank you for updating the above article with new information. I have contacted UNFI to see if I can order a box and am waiting for their reply. Appreciate you letting me know about this option. I would love to try the waffle recipe with zucchini and parsnips if I can get parsnips – fingers crossed. 🙂 Thinking if I cannot get parsnips, maybe I can substitute white rice for the parsnips and cooked zucchini puree for the beans?
Have not tried carob powder yet, but bought some and it will be the next introduction for us! Super excited to add more new foods and try out new recipes!!
Thank you for all you do!
Alex
Megan says
Hi Alex, thanks, and I hope you all had a lovely Thanksgiving, too! My husband reminded me that UNFI supplies sealed grocery items, to it’s actually Organically Grown Company here in Oregon that provides the bulk veggies. Because we owned a restaurant and ordered from both companies, I confused them; sorry to waste your call with UNFI! I can’t remember what state you’re in, but what you want to look for is the bulk supplier of vegetables to markets or co-ops that carry organic. So, if you’re not sure, start with the grocery store, and ask them who their organic veggie supplier is. Try to find a small or medium size supplier who is willing to sell bulk boxes to individual families or small groups (co-ops). Yes, I like your idea of using the rice + zucchini in the existing rice and beans waffle recipe. You may have to play a little to get the inside texture just right, and it tends to get better after it begins to cool, because it’s egg-free, so becomes more bread-like when the gelatin isn’t hot. Yay and hopeful for carob for you! Happy to help! 🙂
A says
Thank you for the updated list!
For the spices, since turmeric has no Vit A and no carotenoids, is it ok for VAD? Between its anti-inflammatory properties and the lovely color it brings, I hope to add it back to my diet.
Megan says
Hi A, no, it isn’t allowed. At first it was, but then later, Dr. Smith found compounds in it that slowed the detox of vA, so pulled it out.
A says
Thank you for the quick response! Does the same go for white and black pepper? I noticed white pepper used to be on the list but is no longer.
Thank you.
Megan says
Happy to help. That’s right. Now, we use a lot of dried, ground ginger in place of pepper, and it works really well!
A. says
Hello,
Do you know if roasted carob power (i.e. https://chatfieldsbrand.com/products/powders/carob-powder/) has phytic acid? From my research, it does not, particularly once cooked and without the seeds, but I’ve reacted to it similarly to my response with soaked almonds (weird, I know) and unsoaked buckwheat (learned to soak pretty quickly after that). Curious if anyone else has has a reaction to carob?
Megan says
Hi A., things that may be relevant to consider about carob: it’s not a seed, but the pod of the seed, which makes it gentler. There are some small amounts of antinutrients in the pod, but these are pretty negligible when the powder is roasted. So roasted carob powder is the best choice. More on carob that makes it gentle: It does not contain tyramine or oxalates, and when carob gum was tested, it was found not to absorb nutrients from food (https://academic.oup.com/ajcn/article-abstract/46/2/307/4694538?redirectedFrom=fulltext). On the downside, re symptoms that may occur with carob, it’s a high-FODMAP and high histamine food. I’m not sure what responses you’ve had with it, but maybe there’s some help in these details.
heraclos says
“It does not contain tyramine or oxalates”
According to “tryinglowoxalates.groups.io” carob contain more oxalate than chocolat or cacao.
Megan says
Hi Heraclos, I’m sorry, but that is misinformation. Please do a search on any other site. Carob does not contain oxalates.
A. says
I realized only several weeks after your response that it was likely not the carob, after all. I had carob with oat milk and I’ve since discovered that oat milk, even from soaked oats, does not work for me – I need my oats cooked. I was sure it couldn’t be the oats! Well, at least the carob was unfairly accused. Looking forward to baking with it. 🙂
Megan says
It can be such a confusing process, figuring out which foods work best in our individual bodies. Thanks for updating, A.
Patrick says
Hi!
Can you tell me what Dr Smith recommends for someone that has constipation?
Megan says
Hi Patrick, I answered you also on the beans post on this topic, but just want to make sure it’s answered here, also in case it’s helpful for other readers. Dr. Smith recommends SunFiber as one great option, and I’ve found it to be wonderful, both for me and for several of my clients. It can be started on a lower dose (1/4 scoop) and then worked up to the full dose of one scoop nightly: https://amzn.to/335eysU I can’t say enough good things about it. I also find that one’s intake of different carbs really affects this as well. Some people do better with varying their carbs! So, for example, only eating oats once a day, or rice twice a day, instead of 3x daily. So I’d play with that a bit, too, to get the perfect balance diet-wise, and then the SunFiber provides the soluble fiber.
Patrick says
I’ve taken sunfiber but I started with 2 scoops/ a day but it was when I didn’t know about vit A. And it didn’t work for me. But I think It was because I didn’t knew about vit A back then and I started with 2 scoops a day right from the beginning, and I’m super constipated. For me it was like taking a placebo. Do you think it was because I started at a high dose of 1 scoop morning and one at night? I was taking sunfiber from nutrify that has partially hydrolyzed Guar gome as its main ingredient. It’s the same right? I wanted to start again at a low dose. In regards to carbs I think that because of my leaky gut every grain seems to feed my bad bacteria, should I eat them nonetheless or give the sunfiber a try again until my gut starts to normalize?
Megan says
Hi Patrick, you are right that that is a really high dose for SunFiber. For myself and the clients I know who are using it, 1 scoop at night seems to be the right amount. Of course, that could vary for you, but others who tried to do more also got constipated. I think that SunFiber is one very helpful piece of the puzzle, and then we also need to look at diet as far as resolving constipation: which grains and how many, which veggies, fruits or beans may also help. I don’t do well with rice 3x a day, for example. And yes, perfect to start slow. I started with less than 1/4 scoop and took over a week to get to one full scoop. Re carbs, depending on how long you’ve been on the diet, have you tried any cassava flour? I find that instead of doing all grains for myself, I split the carbs in the day: so cassava at breakfast and rice at dinner, with either or neither at lunch. Sometimes I do just protein at lunch. It’s good to gently experiment with how each choice affects your bowels. If you do rice, be sure it’s Basmati, too, as others ferment in the gut and can feed bacteria. If cassava causes bloating or new problems for you, then it’s too soon. I added it into the low vA diet after 2 years because of concerns about its resistant starch, and now it actually is helpful.
Patrick says
Is medium ripe banana low in vit A, and can i eat it freely in this diet?
Megan says
Great question, not freely. I allow my boys to have one medium ripe banana a week.
Niki says
Excellent post and information! I’m curious if you’ve evolved your thoughts/experiences/conclusions with the VAD approach since this post? I find it overwhelming and afraid of getting sucked into another orthorexia situation and hyper focus in attempt to heal chronic illness when it may not apply. I’m not sure Dr G Smith would be helpful in avoiding me going down that rabbit whole of mentality… he’s pretty intense, I’d connect with you but I have no funds to allocate to this.
Megan says
Hi Niki, thanks for explaining your thoughts and reaching out. Occasionally I have clients with the same concerns. Personally, I have never struggled with orthorexia, I think because my pursuit of being 98% well is always more intense than my relationship with food. My wellness drives me (without me trying emotionally), and food and my research on diet is just a tool to be well. I have also always LOVED food, which makes it easier, I think, for me to adjust what I’m eating, because I can always find ways to love new restricted foods themselves. Instead of feeling the weight of the restriction, I fall in love with the new foods I can have and really enjoy them. So that’s my recommendation if you decide this is a good and likely truthful avenue to pursue, is the mindset of truly loving your new foods as you pursue truth and wellness. Anytime you feel restricted or miss an old food, find a new favorite to FULLY enjoy… It is not about doing it right; that’s an academic and intuitive choice beforehand that’s already been made; it’s about enjoying each day what you can have. A good example in my current diet is dandelion root tea. I recently went low oxalate and low salicylate as well as low A, and I was missing my other hot cups; I finally figured out I could still have pure dandelion root tea, and now it’s my favorite. I love it so much each morning, and focus on that instead of the other hot cups I had to give up or perfectionism. So, re your other questions: Personally, I no longer believe this diet is a theory. I believe scientifically that it’s respectful to call it a theory still, but I fully believe it’s true based on 100s of us who have done the diet now for 2-3 years and the new rodent studies that Genereux has done. It’s amazing to me how entrenched our mindset is against this concept that it’s so slowly considered, whereas diets like Whole30, AIP and GAPS were immediately considered factual without any long term data about the health effects of eating the rainbow that intensely. Re Dr. Smith, I think most people who find him very intense get used to his bedside manner over time because his research is so remarkably insightful. It is giving grace for quirky personalities, knowing many brilliant humans before him have similarly been very intense socially as well. It can become endearing as you appreciate the content of what he’s sharing. I hope those thoughts are helpful. At the end of the day, your intellect and intuition are important factors in deciding if this diet is right for your body. Blessings in your process!
Patrick says
There’s any specific best time to take Charcoal? Is it before a meal, during it or after?; or on an empty stomach in the morning? If I don’t tolerate a whole capsule of 500mg charcoal, can i open it and put the powder in the water and drink it? I heard that psyllium can help the charcoal go through the intestines and out. So blend both together before taking it?
Megan says
Hi Patrick, I take activated charcoal each morning with my other supplements and right before breakfast. When you say you don’t tolerate a whole capsule of charcoal, what happens? Does it make you constipated? Do you already take psyllium and find it helps you with constipation? Yes, you could stir them together and take them as you describe.
Patrick says
Are chickpeas aka Garbanzo beans allowed in this diet? I might have a problem with oxalate and for my research most beans are high in oxalates with the exception of a few and chickpeas included.
Megan says
Hi Patrick, they are indeed allowed on the diet. I personally do the low oxalate version of the diet. I enjoy chickpeas, black eyed peas and yellow split peas as the best bean options that fit both diets, as well as lentils. Black eyed peas and yellow split are the lowest oxalate, but chickpeas are great for medium oxalate, which is best when you first begin reducing oxalates (to avoid oxalate dumping).
Juan says
Hello, in one of the dr Smith’s livestreams he mentioned an article that is inside the love your liver program where he specifically tells about types of dysbiosis and what are the different probiotics that someone could try in specific occasions. Can you tell me which ones are mentioned, and their different applications in relation to different types of dysbiosis? I really wanna try on probiotics, because i have dysbiosis and pratically anything that I eat just goes slowly in the digestive tract and don’t seem to get well digested. And i’m already 2 months in the low vit A diet, feeling like this is the right path to go.
Megan says
Hi Juan, I’m so happy the diet is working well for you! I can’t share that detailed of information because Dr. Smith has put it in a paid venue partially for that purpose, that to have access, people to need to pay him for his work. I’ve provided the dietary basics so people can get started. I do think his price is affordable, and the forum is worth the price, if at some point you want to consider that. Personally, I did not find the probiotics to be helpful, but you may. Another option for you to consider is Serrapeptase. It needs to be taken 1 hour before food on an empty stomach with a full glass of water. I started at the 40K dosage. Some people end up taking a higher dose. It’s wonderful for aiding digestion and promoting healing. You can read more about it. It is allowed on the diet. Here’s the one I use: https://amzn.to/3IM6D2i If you try it, I hope you find it to be very helpful. Best wishes in this process!!
ShirlGirl says
Hi Megan,
Who is your ND and do they do tele-med? I’m trying to find an ND that understands all this to work with me.
Shirley
Megan says
Hi there, have you reached out to Dr. Smith? He’s the one I’d recommend who works with this diet and has a vast wealth of information for those of us doing the diet. He can do tele-med, and he does lab work.
ShirlGirl says
Thanks Megan! I did find the link to him and have saved the site.
Megan says
Great. 🙂
ShirlGirl says
Also, if you could answer another question, did you do low histamine diet while doing Vit. A detox? The list for Vit. A seems to have a lot of histamine foods listed.
Thanks in advance,
Shirley
Megan says
Happy to help, Shirley. Yes, I did. I started with egg white omelettes cooked in butter with sauteed mushrooms for breakfast. I had to wait to introduce beef, so I ate chicken. Etc. I just made do with the few foods I could have, and after 2 weeks I was able to begin reintroducing foods. By 6 weeks, I had no further issues with histamines and was eating all the low A foods with lots of beef. I supplemented with B1, since egg whites alone can deplete it.
ShirlGirl says
Thanks again Megan!
I am really struggling with this since I am also healing from Hodgkin’s Lymphoma naturally and can’t eat very much meat (heme iron feeds cancer) and I have been pretty much vegan for the past 2 years. Trying to implement with beans and rice, but finding it so difficult to figure out which ones I can have without reaction. My gut is shot since I had breast explant surgery on March 21, 2022 to see if I could get to the root of all the histamine and Mast Cell reactions. Then after they pulled drains I became so sick with an infection that it put me in the hospital for 5 days and on 5 different antibiotics. The worst is that I am now down to 101 lbs and am 5’4″, underweight for sure. I’m assuming I might have Vit A toxin since I have been eating tons of Vit A in the large amount of greens everyday through juicing, smoothies and large salads. But I was on low oil, did eat nuts (until now-histamine issues with them). Not sure how to gain weight while cutting out so many foods.
Megan says
If you can, I’d schedule an appointment with Dr. Smith, or me, if that would be helpful. If you buy Dr. Smith’s lactoferrin from him, this gives you an almost free 15 minute consult with him, during which time you could ask him your most important questions. You can read this page; I can’t remember exactly how it works, so you may need to email Julie, but you want to choose the option that includes the consult. https://nutritiondetective.com/store/p/lactoferrin SO sorry for your struggles!
ShirlGirl says
Thanks Megan! Appreciate your thoughts. I will look into that.
Megan says
Happy to help, great!
Deanna says
Hi Megan, here’s my story.
I have many “autoimmune” diseases including non-alcoholic fatty liver, prediabetes, endometriosis / adenomyosis, and many more. I had finally ordered a copy of Sally Fallon’s “Nourishing Traditions” and became convinced that ancestral eating is the way for me. However, there have been some bumps in the road.
First, was when I became extremely ill, almost instantly, after eating a handful of raw radish sprouts. I have pretty severe IBS and this episode was horribly painful. Then, yesterday, I tried my first dose of cod liver oil. I applied it to my skin and noticed a slight red bumpiness. Well, maybe it’s the lemon extract, I thought. Down the hatch went 1mL of the fishy oil, and I *immediately* got a headache. I wasn’t sure if this was some kind of bizarre detox reaction, or if the oil itself was making me sick. Then I got sick to my stomach, which wasn’t a surprise to me.
Then by the grace of God, last night, I discovered Grant’s first book, and am already a third of the way through it! I am very excited to have found this information about vitamin A toxicity. I can relate to almost all of the symptoms and diagnoses.
I am overwhelmed about where to start. I see a naturopath, but this isn’t on her radar at all. I seem to be intolerant of all cruciferous vegetables, all grains and legumes, beef, pork, dairy, and more. I am really lost about what I can eat safely, since beef, rice, and beans seem to be staples for people.
I also have a question about cashews. I understand that you have a parenthetical statement that they are a fruit. For those of us who do well with fruit, would cashews be ok?
Thank you so much!
Megan says
Hi Deanna, I’m so glad you found Grant’s book! Wonderful timing, before you got worse. But, I’m sorry for your suffering and pain so far. What’s great about starting a low A diet is you can modify it a bit in the beginning to accommodate food sensitivities that you’ll overcome. I can chat with you here to some extent, or if you need more support, you can email me at [email protected] for consulting, OR reach out to Dr. Smith if you know you want and need a doctor. He can do full blood work and a mineral analysis. Because of your broader health issues, it would be great to seek his help at some point. In the meantime, cashews are out. But you do need to land on some proteins to start: can you do clean white fish and chicken? Egg whites? (See notes about supplementing with B1 when eating egg whites.) These would be temporary until you can add in grass-finished beef or buffalo (or wild red meat game). Great to avoid all cruciferous veggies. Can you do: peeled zucchini, peeled cucumber, butter or romaine lettuce, peeled apples, blueberries? How do you do with organic tapioca pearls? Macadamia nuts, sprouted pumpkin seeds? These are some places to start, and then you could build from whatever your “safe” foods are over time. I’ll help you figure out some starting foods, and you’ll have enough to be on a low A diet with a little variety while creating some stability.
anne says
Hi- I have MACAS and can only eat 3 things right now. Millet, chicken breast and kale. Is it better to eat NO vegetables than to eat the kale? Thanks.
Megan says
Hi Anne, I can only tell you what I would do in your shoes, but not what is right for you. For me, I would indeed not eat kale. Many native peoples have just eaten meat and grains. There are sometimes supplements we need, like zinc, selenium or B1. Best wishes for recovery and wellness and reintroducing other foods soon. I, too, had just 3 foods I could eat at one point. xo
Sam says
Hi. When you look at the stearic acid contnet of both butter and coconut oil, isn’t butter much higher. From what I read, the stearic acid content in butter is 10g per 100g and in Coconut oil it is only 2,8g per 100g. If it really is stearic acid that makes is the problem, shouldn’t butter be also on the avoid list? And if I remember correctly the stearic acid is a problem only if the coconut oil is extra-virgin but I think refined oils are even more problematic in overall health (atleast that is what studies suggest). Also, do you know if it is possible to get a Hypervitaminosis A from accutane?
Thank you for your good work!
Sam
Megan says
Hi Sam, butter has some beneficial properties that when eaten in small amounts compensate for any seemingly problematic components. If you’re in the Dr. Smith forum, there are more details you can access, which include the mechanisms at work on a scientific level as well as how the diet plays out with hundreds of patients. This does hold true: EV coconut oil is problematic and 2 T or less of butter daily is not. I can tell you from 3 years following Dr. Smith’s insights and Genereux’s original insights, that they are right, amazingly so. Re Accutane, a big YES. I did write about that in this article, but I know it’s a long one and easy to miss one section. But a large number of the people on the diet used Accutane. Happy to help. 🙂
Joe says
I see a lot of mention of peeled apples but no explanation as to why the peel needs to be removed. In my limited research I could find no reason why you would want to remove the peel for the purposes of Vitamin A detoxification. Apples in general have very little Vitamin A in them (<2% of daily recommended depending on apple variety). I understand that removing the peel may reduce that a bit, but it's already such a low value compared to some other foods that were approved for eating on this diet like lettuce or arugula, that I'm not sure it would really make a meaningful difference. The peel is where most of the fiber content of the apple is as that can help feed healthy gut bacteria. It seems like the benefits of the peel far outweigh the risks. Am I missing something?
Megan says
Hi Joe, just to first clarify, arugula is not allowed on the diet. I’m not sure where you saw that? The peel on apples, like the peel on most fruits and veggies, is where the carotenoids are concentrated. It is the source of most of the vitamin A, so we avoid that, as it’s a source of the toxins we’re reducing on a low A diet. We still get fiber from the apple itself, and because this is a short term detox diet with a specific purpose, we add fiber to our diet in other ways that are safer to ensure the toxins are being ushered out: beans, oats or even an effective fiber supplement like SunFiber. If you are on the diet, or decide to, I recommend tapping into Grant or Dr. Smith’s forums, because there you can see a lot of these kinds of discussions. A lot of what “seems” to be the case from the outside has been studied by these two men for the last few years, including clinical work with all of Dr. Smith’s patients, to help them streamline the process. All of the suggestions and guidelines are remarkably accurate and not accidental or items overlooked. Also, remember that daily recommendations do not take into account that vitamin A is a toxin. Any vitamin A in is not vitamin A out.
Sherrie says
Hi Megan, let me tell you something about myself I am a type one diabetic was diagnosed at 10 months old, I lost my eyesight completely at the age of 21, now I see a kidney doctor but they say my kidneys are doing good but they are a little damage due to protein, and I’ve got arthritis, and I just want to know if this diet would do anything for me, because a lot of the veggies that you say not to eat I eat I love them, I don’t eat a lot of bad stuff I’m very healthy but I’m trying to lose weight which I was on keto and did not work for me very well, I lost some weight then I gain nine back so I’m still trying so I’m wondering if this would help me please let me know thank you so much
Megan says
Hi Sherrie, I’m sorry to get your message so late; it went into a different file. I would suggest you reach out to Dr. Smith. You are someone who should work directly with a doctor. Best wishes! (I give his contact info in the post.)
Bonnie says
Curious as to why Bibb / Butter lettuce is on this OK list of foods to eat when it is high in Vitamin A and Carotene? https://www.urmc.rochester.edu/encyclopedia/content.aspx?contenttypeid=76&contentid=11250-4
Megan says
Hi Bonnie, there are several foods like butter lettuce that have been included on the diet because they broaden it without causing problems. Not everyone on the diet need include it, or Romaine lettuce for example, but it is pretty benign eaten in moderation. It is actually relatively low in vitamin A precursors. Also, it’s ideal to compost the darker outer leaves and enjoy the heart more, which is what we do with Bibb and Romaine.
Patrick says
Yam is low vit A? It is allowed on the diet?
Megan says
No, definitely not.
Trista says
Hi,
My 5 year old seems to have gotten toxicity with her formula when she was around 3 months.
It contained almost twice her daily recommended amount..add in the pumpkin or carrot or sweet potato baby food.
She slowly started turning orange. At around 18 months we seen her paediatrician who said it was fine but the immunologist told us about vitamin A being stored in the liver and that it was now going to her skin. Simply told us to cut out orange foods until her skin returns to normal.
Which is what we did. But she was still getting formula due to eating issues. So still getting too much vitamin A.
She reacted to dairy severely. Constipation, loss of eye contact… regression.
We had assumed milk protein allergy.
After 6 months we started slowly reintroducing orange foods which seemed to cause eye issues and neurological issues. But never connected vitamin A toxicity the cause. Being we didn’t realise how serious this vitamin A issue was.
Papaya for instance would cause my daughter to look out the corner of her eye. But at the same time it seemed to help her eczema. Once we cut out papaya the eye thing went away.. until it came back some time later and we couldn’t figure it out.
I wanted to ask if you know much about vitamin a causing hypercalcemia?
My daughter not only reacts to all dairy but we have now realised it’s anything high in calcium.
She also reacts to high vitamin A foods. And until now we hadn’t seen the connections. Thinking it was histamine and high salicylates causing issues. Which it still could be due to the havoc vitamin A toxicity causes.
Unfortunately we have been giving her dairy free spread which contains added Vitamin A. She was getting almost her daily recommended from it.. she started throwing up after carrot and cantaloupe and I couldn’t figure it out until now.
I keep a diary and looked back and her throwing up episodes is always after something high in vitamin A.
We have cut out the spread and all high vitamin A foods and she is bouncing back better than expected..
What is interesting about butter is that when we had tried it last year, she started to be able to have some foods without reaction. Even dairy. We used organic grass fed.
The only thing is that she would get really hyper after it. Which dairy does in general. So I assumed she was intolerant all the same. But can’t help but think that the butter was helping her. Her eczema also cleared up around that time.
Since stopping the vitamin A spread and cutting out vitamin A, her eczema is almost gone touch wood. And some other issues also seem to be going away.
Interested to know if you have any information with hypercalcemia. Many studies show the connection to vitamin A toxicity.
Also about salmon. We have read that salmon can treat hypercalcemia. Do you have any information about its role in vitamin A toxicity? As it seems to be on the low end for Vitamin A content.
Thank you in advance. I hope to spread awareness of vitamin A toxicity also.
Megan says
Hi Trista, thanks for sharing so much, and I’m so glad you figured out vitamin A toxicity and are well on the road to recovery with your daughter. Yes, absolutely vA toxicity can lead to hypercalcemia (and also iron overload). Gentle supplementation of minerals like zinc and magnesium, and vitamin D from the sun, may be helpful for your daughter. I’d steer clear of salmon and most brightly colored foods. I can tell you from Genereux and Smiths’ work and my own experience that salmon is a No food. I would not look at any isolated claims about certain foods being good for any condition. Instead, I’d stay closely with the low A diet, consider hair mineral and blood testing, so you can supplement wisely and also consider other factors like: copper toxicity, aldehydes etc as her wellness progresses. Dr. Smith can help you with the exact diet and supplements for her, or I’m happy to answer any other questions if I know the answers. 🙂
Alex says
Hello Megan,
I hope you are doing well.
My brother has been using Garcinia HCA (this brand: https://www.amazon.com/Life-Extension-Garcinia-HCA-Count/dp/B00MQSMIP4) for years for kidney stones. Do you know if Garcinia Cambogia is detrimental to the liver due to vitamin A?
Megan says
Hi Alex, I hope you are well, too. 🙂 Based on Dr. Smith’s information on the topic, all citric acid or chemicals similar to it, which is this supplement you’re referring to, mess up copper metabolism. I’ve written a bit about this that you may have read, but copper toxicity has ended up being a key piece of the low vA diet and wellness process. So it looks like this supplement is a big No to me. I hope that helps. I also see that problems with this supplement for the larger community do happen to the liver.
Alex says
Thanks so much, Megan. I will let my brother know.
I am so thankful I found you and your site.
All the best,
Alex
Megan says
So glad you’re here, and I’m so glad it was helpful! 🙂
Jr says
Not sure if anyone mentioned but sunflower seeds contain vitamin E. Sunflower butter is usually my go to if I ever feel I need vitamin E.
Great post!
Megan says
Hi Jr, thank you! While a small amount of sunflower butter is allowed on the diet, sources of vitamin E are actually discouraged. It is problematic in the detoxing of vitamin A, and over time I’m sure Dr. Smith will publish more of his opinions about vitamin E in general, and why it can be problematic. Sorry about that.
Barbara says
This diet has a lot of overlap witn the well-known low oxalate diet I follow to avoid joimt pain and other issues. I encourage you to learn more about this as your detox diet also imcludes a dew foods dangerously high in oxalates. Also has some overlap with a gout diet.
Megan says
Hi Barbara, thanks! I have actually done a low oxalate version of the VAD diet and written about it. I found it helpful and now maintain a medium oxalate diet. I also have several low oxalate recipes on the blog. Here’s one of the articles that combines low oxalate and VAD: https://eatbeautiful.net/lox-oxalate-and-low-salicylate-food-list-with-printable/
Alfreda says
Hi Megan! Me again!
2 more questions
1. I realize that cucumbers might have to be my go to right now because of the other food issues I’m dealing with. It looks like cucumbers are a go to for your family as well. How did you make cucumbers work although it is a lectin? Up until now I have been peeling, deseeding and limiting to an amount each time I eat it.
2. I’m going to try wild caught scallops and Petrale Sole from Vital Choice. I hope these are currently ok to eat.
Do you know of any other low fat wild caught white fish that is safe now that cod is out?
Referring to Vital Farms list of wild caught white fish, I see that they sell Pacific Lingcod and Black Cod (probably out), Atlantic Haddock, Alaskan Halibut, Chilean Sea Bass,
Megan says
Hi Alfreda, yes, what you said is the right approach to cucumbers, until you can handle more, and then I began leaving the seeds in. 2. I personally found these seafood options helpful at one long stage of my low A diet, so I personally think it’s fine. Long term, maybe not, but we all have to make compromises with our limitations to get the next stage. We personally ate lingcod, black cod and Chilean sea bass. Again, I can’t officially say they’re perfect, as black cod is a bottom dweller, for example, but we were eating these only once a week or less, and it helped us through a time. If you don’t need them, then exclude, but if you need the variety for now, then I believe they’re fine for short term. Copper and mercury are two issues to consider with seafood, copper being a shellfish issue. So depending on how copper toxic you are, and how/how much you’re supplementing with zinc and molybdenum, you may or may not want to include.
Alfreda says
Thanks so much!
Megan says
My pleasure!
Alfreda says
I did it again. Please remove my last name.
Megan says
done 🙂
Angela Watson Robertson says
Hello! Where can I find a list of yes/no foods for Lectin Free + Low HIstamine + VItamin A detox? I see that many foods on the vitamin A detox list conflict with lectin free and low histamine. I’ve been battling SIBO/parasites/MCAS/HIST for over a year and still at my wits end what I could be eating that is bothering me but now looking at lectins, but it’s so hard to stay on this restrictive of a diet for so long and now this Vitamin A thing! wow. Thanks for your help.
Megan says
I understand. Sometimes when you start the low A diet, or others, too, you do have to be on a pretty limited diet. It can be very helpful to work with Dr. Smith when deciding on what one’s diet should be in the beginning. In your case, if you wish to do the DIY version, which I did, too, you’ll need to cross reference and combine all the lists to see what you can have. Ideally you’ll be left with some source of protein and some source of carbs, at the very least. It doesn’t have to be perfect, but ideally you find a place where you’re stable, and that’s where you start from, ideally no triggers, and you begin to see improvement. For me, I started with egg white omelettes, sauteed mushrooms and peeled white potatoes. I have a client who started with really fresh low histamine fish, blueberries and one other food we found for her. Within weeks, in both cases (as examples), new foods were added in successfully. Keep in mind the option of supplementing with vitamin B1, too, as I do think that was helpful, as well as the other ideas I share in this post: https://eatbeautiful.net/mcas-histamine-lectin-intolerance-tips/ Let me know if you have any specific questions after you try to create a Yes food list for yourself. (I assume you already have this list to compare with the low A list: https://eatbeautiful.net/low-histamine-lectin-free-food-list-printable/) Best!! There is always an answer/cause to symptoms, so keep on keeping on!
Angela Watson Robertson says
Who is Dr Smith?
Megan says
Hi is the main doctor that works with patients on the diet, and he’s also behind a substantial amount of the research on liver detox, copper toxicity and related issues. You can find him here: https://nutritiondetective.com/, and he also has various forums for teaching and community support.
Alfreda says
Hi Megan!
What is the latest on artichoke hearts on LYL?
I bought them when I started Vit A and am now ready to try them but it doesn’t sound like it is on Dr. Smith list of “yes” foods.
Megan says
I believe they are still officially a Yes food. I just checked again, and people as recently as 8 months ago were talking about them. I don’t see anywhere that they were removed. I do see your unanswered question in there. 😉 I also see that Romy put a “?” next to artichokes below the inulin discussion. When I looked for studies, I did find one that says artichokes are high in inulin, (as well as an article): https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6778948/ I just posted the question in LYL to the broader group, so maybe more people will read it there than in the smaller inulin thread. We’ll see what people say!
Alfreda says
Aww! So thoughtful of you! Thank you! I guess we will wait to see!????
Megan says
Sadly, no word there. I’d avoid until we know more. I will try to remember and ask Dr. Smith at my next appointment with him. 🙂
Alfreda says
Sounds like a great idea!
Ethan M says
Hi Megan,
I recently started a low Vit A diet using your website as a guide. It’s been extremely helpful so far. I have a couple questions:
1. How did you introduce carbs as you progressed through the diet? What carbohydrate sources and when as you reintroduced them? I’m transitioning from 2 months of keto, and have been having some discomfort, bloating, and constipation. I know you touched on it above, but I would really appreciate more clarification.
2. Is Dr. Smith a reputable Naturopath? My parents are skeptical of giving him money online, and would appreciate your honest word that he’s trustworthy. I’ve found his Youtube and website extremely helpful, but they’re still hesitant.
3. Have you helped consult people that have had supposed Accutane damage? I believe I have Accutane damage, taking it twice when I was 13 and 14 y/o (I’m currently 21). If so, have people recovered well?
4. How should I implement charcoal?
4. What would be the best piece of advice you’d give someone starting a low Vit A diet?
Megan says
Hi Ethan, happy to help. From being in the Love Your Liver forum, I can say that so many of us have similarities in our processes, but we each also sometimes feel like we have to figure something out for our unique body, because each one’s history and current state really is unique. So, I can happily weigh in, but it may not work for you, as I know you know. 1. I actually started with peeled russet potatoes, because I was grain-free at the time and also had other restrictions. From there, I eventually added in oats successfully, which became a staple food for me. I do not do great with rice, but do pretty well with Eden’s brown rice pastas. If rice causes you constipation and bloating you might try their pasta or my next mention: My best carb is actually white masa. I know a couple of people who can’t do it, so it’s not a sure thing. But for me, it’s gentle and doesn’t have inflammatory compounds like high oxalates. 2. I understand that concern. Yes. I have now known him for years and many clients who’ve worked with him personally. Plus, I have had 5 people from my immediate family as his patient. It is a lot of money to pay online, but I’ve found the process very secure, and his receptionist Julie is helpful if needed. 3. Many people in the Love Your Liver forum are recovering from Accutane damage. Dr. Smith feels it can take a bit longer to recover after using this Rx, but frankly, I think it’s taking all of us a long time to fully recover. And it’s just necessary, no matter how long it takes. There’s no other way than forward. I am personally not seeing new clients right now because we just adopted internationally, but yes, I have had clients who took Accutane and are currently on the diet. 4. I can tell you what I do for charcoal, because I’m not a doc, so I can’t say what you should do. I take 2 doses at night (the equivalent of 2 capsules, but I stir a bulk product into water so I have less pills), with added Magnesium Citrate (this one: https://amzn.to/3XE4iQf, a little less than 1/2 a scoop in water, to prevent constipation from taking double/extra charcoal). You could always start with just one capsule of charcoal, which is how I started, and just make sure you’re regular before you increase, or you can add in more Mg until you’re regular. (The only activated charcoal brand I’ve found that isn’t good and to avoid is Solaray’s.) If it’s good, it should turn your poop black and anything it touches black; it should basically stain. 4. Hmmm… 😉 that’s a tough one. Find the few foods your body likes and that have you on track for detoxing smoothly, without any big symptoms, and camp out there happily for a long time, just making small tweaks as necessary. Don’t cheat. Also, make your appt. with Dr. Smith ASAP because having that lab work back and being on the right supplements really helps a lot. Best! I’m excited and happy for you!
wanda S says
Perhaps more rapid vitamin A detoxification would result from water fasting.
Megan says
Hi Wanda, good question, and it’s been answered more thoroughly in the Love Your Liver forum, but in short, no. The body needs fiber to detox vitamin A. Water alone will only detox a small amount. The body also benefits from protein (meat) in the process, and certain minerals also benefit the process: zinc, for example.
Wanda S says
I wonder if vitamin a toxicity might be the cause of non-healing veinous leg ulcers, which by the way are extremely painful.
Megan says
Dr. Smith does address this. He pretty much addresses everything lol. He’s quite amazing how he works with each patient and every single symptom they have to overcome them and attain wellness. He understand the complex body systems and explains things beautifully as he aids in the process of getting well.
Wanda Schneider says
Elsewhere you said that CBD oil causes fatty liver disease. So, I was wondering if vitamin a toxicity is also known to cause fatty liver disease?
Megan says
Hi Wanda, rather, a fatty liver can not store excess vitamin A as well, so toxic vitamin A is left to re-circulate in the body more, or be stored in other tissues, because it can’t be stored as well in the liver. A fatty liver will cause more vitamin A symptoms, as a result.
Teresa says
Hi there,
Where can I test my vitamin A levels and my copper levels? Is there a do it yourself at home option that you know of?
I have IBS forever and am open to trying anything at this point. Thanks for all of your articles!!!!
T
Megan says
Hi Teresa, I’m sorry for your IBS, and happy to help. 🙂 Definitely those of us with chronic or stubborn issues tend to be the most open-minded about this concept, and then find amazing relief and encouragement. I would definitely encourage you to save up (if necessary) to actually see Dr. Smith, or his PA, which is less. They will order the tests from a lab and send you what you need for the hair test, which is necessary for an accurate copper level. Dr. Smith uses both blood and hair tests to get the most accurate reading. You can go through a lab on your own, but you will need one of these two to read your results, as they have their own ranges, which are relevant, and then their dosing recommendations will be accurate, and they’ll keep working with you for 6 months, follow-up times to make sure you’re getting better. I wish it wasn’t a financial investment, but you get probably more than you pay for. Dr. Smith is very thorough, and you get the forum, too, included, of helpful people on the same journey. I hope that helps!
Guillermo says
Dear Megan,
Thank you in advance for your info in regards of VAD.
Would you mind explaining why the following foods:
– Coconut meat/kernel;
– Refined & decolored palm oil; and
– Cocoa powder/solids 100% (0% cocoa butter)
are not suitable for VAD? Wonder if palm kernel oil is out, too…
Cheers!
Megan says
Hi Guillermo, sure, they all contain fat components, most notably stearic acid, which exacerbate the detox of vitamin A, and in really noticeable ways. This kind of fat makes toxins more aggravating instead of helping the toxins exit the body, so one will feel or see frustrating symptoms when these are included. The only fats that don’t do this are modest amounts of refined oils like olive oil, avocado oil and refined coconut oil. Even butter does not allow the diet to go as smoothly. I have personally experienced this, and find ongoingly the wisdom of the protocols, as they always turn out to be true when challenged, and it’s a waste of time and ends up being discouraging to do the alternative. Cheers, too!
Guillermo says
Hi Megan,
In regards of previous comment. What size of VA does Nutritional Yeast have?
Best regards!
Megan says
Hi! Nutritional yeast is not allowed on the diet. It increases the absorption rate of vitamin A, encouraging its storage in the liver instead of the opposite.
Guillermo says
Hi there!
Almost forgetting. What about toasted and grounded barley flour (aka Machica; with this name is known at Andean regions of Ecuador, Peru and Bolivia)?
Kind regards!
Megan says
Hi Guillermo, hulled barley flour is great, but not hulled isn’t ideal for this diet. Best!
Guillermo says
Hi there! Hope you’re doing well!
In fact, after first grounding, barley is sifted and grounded over and over again, several times, until we get the finest flour; it’s (indirectly) hulled after all.
If you wonder why barley is toasted, it’s to enhance its nutrients.
Best to you, too!
Megan says
Thanks for that clarification! Best to you as well! 🙂
Alex says
Hello Megan,
I hope you are doing well.
I wanted to ask what your thoughts are about dried Smyrna figs vs. black figs for VAD. There is conflicting and confusing information online… Are any black figs better than the tan colored figs due to lower carotanoids? Does it make a difference if figs are fresh or dried? For black figs on VAD, is the reference to any black colored figs or is that a variety of specific figs that are lower in carotanoids and A? And lastly, are fresh figs best for VAD due to them being less sweet? I have never had fresh figs, but had the dried tan ones and love them. I had not had them in years and was wondering which ones are safest to consume and not sabotage our VAD efforts.
Thanks.
Megan says
Hi Alex, happy to help, and I hope you all are well, too. Black figs are lower in carotenoids, and fresh are better than dried. That being said, in small amounts, it would be okay to eat any or all, but mold is a big issue with dried figs, so watch for that closely, as you can often even see it on dried figs. The other issues with figs is how high they are in sugar, so if you eat dried, you might choose to eat only as many as you would if they were fresh (about 3, for example). They are my favorite fruit, so I can relate to your questions. Our tree is still pumping them out right now, all before our first frost. We are eating them daily (I eat 1 to 3 a day), and I had to freeze many, too, so they wouldn’t be wasted. Enjoy!!
Guillermo says
Hi Megan, hope you’re doing well!
Regarding your last response. Why do you prefer figs over medium-ripe bananas (not cooking bananas – aka plantains – they have about 20 times more carotenoids than dessert bananas), if it has smaller amount of carotenoids than the former?
And another one. What are your thoughts about tasteless gelatin? Or collagen, in the same regard?
Kind regards!
Megan says
Hi Guillermo, you, too, thank you! (Sorry for the late response!) I’m not sure I exactly understand your question, so please feel free to clarify if I’m misunderstanding. I do not prefer figs to bananas. 🙂 I think bananas are a great food on this diet! 🙂 Wonderful potassium, and if the sugars don’t bother the eater, great to eat more than one a day. Both gelatin and collagen are fine, but not quite the super foods they’re touted to be, IMO. They can serve a few functions, though. Gelatin can be helpful in certain recipes, and is certainly a fine food to consume. It can be gentle and helpful for some, but I don’t believe it will create great health strides for most people. Collagen can be useful in recipes as well, and it can be used conveniently alongside meat proteins in a day, if someone is having a hard time getting enough protein for a variety of reasons.
Guillermo says
Hey there, Megan!
Thank you so much for your response! And, putting aside the fact either figs or (dessert) bananas could get wasted, eating them frozen are so tasty!
Sure thing, gelatin is used for consistency; in the same regard, is gel (mucilage) from flax safe, even though seeds being high in lutein + zeaxanthin?
Best to you!
Megan says
No, flax is out, definitely discouraged. Best to you, too! 🙂
Bob says
This concept is truly fascinating (and really weird!). I’m sticking my toe in the water, I’m dealing wit a rash on my back that “suddenly” emerged. Do you think it makes sense to start by eliminating all A supplements (in my multivitamin, etc.) and seeing if that does me some good, and then proceeding with the full diet? Or do you recommend jumping in feet first right from the start. (I’m guessing the latter!) Thanks, and best regards. (By the way, any thoughts on chia seeds, good or bad?) — Bob
Megan says
Hi Bob, yes, many of us have come to the diet like you are. I know I felt that way. Yes, all in. Because you can always decide it isn’t working. But to see if you’re a “believer” lol, I would eliminate both supplements and offending foods. Chia seeds are out, sadly. But I do a lot with pecan butter and macadamia nuts, if you find that helpful. Good luck! I think this diet is for almost everyone. I hope you see a significant improvement.
Bob Frost says
Thanks Megan! OK, all in! 🙂
Megan says
Great to hear! Let us hear how it goes, if you’d like to. 🙂
Bob Frost says
One more quick question if I may — goat milk, yes or nor? Thanks in advance and happy holidays.
Megan says
No problem. It’s a No. Happy Holidays! Let me know if you need non-dairy milk options.
Claudine says
Hi Megan, where do you purchase A2A2 products that you mentioned? Thank you!
Megan says
Hi Claudine! In my case, originally it was a local farmer. But I have now also found Alexandre brand cream that’s grass fed and A2A2 at some local markets, including Market of Choice. It is low and slow heat pasteurized, but it does agree with my body, and I always know my body can tell what’s the good stuff and what isn’t. I use it rarely now, or in very small amounts for special occasions. We don’t use enough to buy from the local farmer anymore. Here’s their product: https://alexandrefamilyfarm.com/products/a2-a2-organic-heavy-whipping-cream I am so happy this company exists.
Janet says
Do you have a shopping list for foods that are ‘okay’ to eat if I need to go on the Vitamin A detox, low histamine, and low oxalate diets all at the same time?
Thank you,
Janet
Megan says
Hi Janet, the best thing to do is to print out the PDFs from both articles, and then highlight the foods that are all in common. I did this personally when I was low histamine, and it worked well. Here’s the Low Histamine and Low Ox list: https://eatbeautiful.net/low-histamine-low-oxalate-food-list-printable/ Best to you in your process!
John says
Hello, I was wondering if anybody could help me with any of the issues I’ve been having. 27 year-old male, been having neurological issues for going on 2 years now and I’m almost at the end of my funds entirely trying a million different approaches to even get the tiniest bit better. I will list my symptoms here to see if it is of any use. It has been complete hell trying to live like this.
Started with body-wide muscle twitching (fasciculations) in May – June 2022, this symptoms has been 1 of 2 that is here every single day and has not let up. Some days I may twitch 40 times, other days I may twitch upwards of 600-800 times. Sometimes they are fast almost like a rapid-fire gun, sometimes they are very small and hardly noticeable. Every muscle in my body can be affected. Eyelids, calves, arms, legs, chest, stomach, outer and inner ears, head, back, I do not think there is a single spot I haven’t had them.
- The second symptom to appear is 2/2 of symptoms that have been here since the beginning and has been ongoing since the very beginning. There has not been a single day this symptom hasn’t been here, all of the other symptoms from here range in severity/frequency. This symptoms is tinnitus. It started roughly 1 month after the twitching and it is in both ears (had my hearing checked they said it’s perfect with no inflammation or swelling and no hearing loss) It is a high-pitched ringing. Sometimes it will flare in 1 ear at a time, similar to when you put an ear under water. It will feel as if that ear is full and have a lot of pressure and the ringing will become louder. It can happen in either my left or right ear but as of now it only ever happens in 1 ear at a time. It typically lasts for 30 seconds – 5 minutes when it flares. Sometimes it happens multiple instances per day, sometimes it doesn’t happen for a few days.
– Internal vibrations. This symptom just feels like my nerves are shaking or vibrating, I also call them internal tremors. I believe it is different from the muscle twitching. It does not happen commonly at all, but when it does happen it seems to go on for a couple of days before ceasing.
- Double vision. I have had a few instances of double vision since this began, it feels like when you cross your eyes to look at your nose, that feeling of pressure on the muscles/nerves behind your eyes when you do it, but it will happen all on its own. This is a very uncommon symptom. I have had my eyes checked and they said my vision was 20/20 perfect, I also had an MRI to check for MS etc… And they said my brain looked great. I will also mention in this section that sometimes when I feel the pressure in my head and I move my eyes around I can feel a tightness in my head/brain and it makes the head pressure worse.
- Brain fog. This symptom lasted for a few months but does not appear to be a thing anymore, for now (hopefully). For the few months that it happened it felt like when a television is on a static station. It is a difficult symptom to describe for me. It was harder to think and process information, it felt as if somebody had poured a bottle of honey inside of my head.
- Heart palpitations. When this symptom began it was very intense, the palpitations were so strong that I would get very dizzy from them and nearly pass out, they would also happen sometimes 30-40 times in a day. Now they seem to be very rare, they are no longer very strong. When they happen now they do not make me dizzy, they just take my breath away a tiny bit, but they happen a couple times sometimes in a week, sometimes per 3-4 months. So this specific symptom has calmed down a lot.
- Head pressure. This is currently my most debilitating symptom. It feels like somebody is squeezing my brain and it is the most uncomfortable feeling I have ever experienced in my entire life. It does not hurt any, and I am very familiar with various types of headaches and migraines (have had them my entire life) it just simply feels like my brain is in a vice, and sometimes when it flares up or gets worse throughout the day I can feel other neurological symptoms come on as a result of it. For example: Sometimes I will feel my jaw forcibly clenching due to the immense pressure, or I will feel my eyes forcibly blinking rapidly because of it.
- Insomnia. During the beginning I just had trouble sleeping due to the anxiety and depression. Now I physically struggle to sleep, I can’t seem to sleep for my regular 8 hours anymore and have not been able to in 8-9+ months. And whenever I awake from sleeping my brain issues always feel much worse, very intense head-pressure, groggy zombie-like feeling, as if I’ve been heavily drugged. I’ve also noticed that if I nap throughout the day the intensity of my neurological symptoms upon waking up are always much more intense and exaggerated than if I were to wake up from a normal sleep one would take through the night.
- Brain surges/zaps. This symptom is an extremely difficult one to describe but I will try my best. It is different from SSRI/SNRI/anti-depressant withdrawal brain zaps that people discuss, where you can actually feel electrical jolts surging through your brain. It is more like my brain itself is jumping and I can feel it affect my train-of-thought. It’s as if my brain is a human-being and it is abruptly hit by a freight train (I apologize, I know this sounds crazy but I would have never believed this could happen to a human, it is very difficult to describe and equally difficult to live with). This symptom appears to have calmed down a tad but in the first few months it was extremely intense. Another way I could describe it is it feels like I am having 1/1000th of a stroke or 1/1000th of a seizure. Maybe not the best way to describe it but I am at a loss for how to portray it to other people so I am using the best words I have at my disposal.
- Tingling. Sometimes I have tingling but it only appears to be in my head-region. It feels like when you get goosebumps but only in my head.
- Sometimes I can feel and hear my heartbeat in other parts of my body I would not typically be able to.
- Vertigo/dizziness. Very self-explanatory symptom, I occasionally get dizzy from whatever is going on, it does not appear to be very common, though.
- I can occasionally feel blood rushing to my head, and with this sometimes I can hear waves rushing through my head that sound like whoosh whoosh, it does not typically make me dizzy but it does sometimes feel like I will just faint altogether.
- I experience random nosebleeds now and I never have before in my entire life. They are very rarely bad, typically they will only last a minute or so.
- Light and sound sensitivity. I wear sunglasses a lot of the time now, even if it is cloudy outside, it is very hard for me to have any light around me (doesn’t cause pain just discomfort). And with the sound sensitivity sometimes certain sharp sounds (doesn’t necessarily need to be loud, could be a door opening/closing in a certain way) will cause me to get jolts sent through my brain. These jolts (which also took me until last week to find a good way to describe them) feel exactly like when you grab an electric fence and it sends that shock right through your muscles that makes your arm jump for example, except these are in my brain.
There is more that I have dealt with but these are the main issues and I didn’t want to overload the page/website with a billion things. Thank you to anybody willing to read/reply (I will also note I was bit by a tick before this happened but was never able to receive any treatment for it if that is any help).
Megan says
Hi John, I hope you’re considering this diet. The symptoms matter less if they disappear! Consider two weeks on the diet outlined here to see what happens … Best wishes. Also, don’t forget about Dr. Smith and his forum, both well worth anyone’s attention who’s dealing with symptoms they don’t understand.
Sierra says
Hi Meagan,
Wow I am so impressed with your blog. So many relevant posts to me and so well written and researched. I have a background in hospital pharmacy and appreciate all the references you give for further reading.
I have been dealing with immune dysfunction for a decade (recurrent and multiple sinus/skin infections, Epstein Barr Virus, Dysautonomia/POTS, SIBO, Candida overgrowth, adrenal fatigue, chronic Lyme, Mast cell activation and Multiple Chemical Sensitivity, heavy metal toxicity). I had been working with holistic and alternative practitioners and they would help me resolve whatever the syndrome of the year was, but the next year I would develop something else. Now I’m working with traditional Western doctors to get some definitive root cause answers and waiting on my Whole Genome Sequencing with Sequencing.com to see what rare disease I may have. I would say all of my syndromes are in remission except that I had an episode 7 months ago with temporary vision loss combined with bloody nose and pulsatile tinnitus (I could hear my heartbeat in my head). So now I am working with a neurologist to discover the cause. So far they found 2 bilateral brain aneurysms so I am being evaluated for vascular connective tissue disorder. I read this week that Fluoroquinolone antibiotics have been found to cause aneurysms in people with these disorders. I definitely had my share of those drugs when dealing with all my infections over the years. So maybe I’m considered “floxxed”.
Do you feel like these conditions can all be explained by Hypervitaminosis A? I was supplementing with high dose Beta Carotene when my health began its descent. I was also 7 years into working in a stressful workplace that also had black mold infestation, 7 years into monthly indoor pesticide application at home, 4 years into Mirena birth control IUD, had mercury exposure (CFL bulb burst in the room), got a stomach flu virus and was in a toxic marriage. My running theory was an epigenetic trigger of multiple stressors (virus, toxins and emotional distress) combined with a genetic mutation that caused immune dysfunction (either inherited or somatic mutation, likely from Epstein Barr virus, which put me through the ringer 7 years prior to my subsequent health descent). I recently got my Immunoglobulin levels checked and they are as follows: IgG = Normal, IgM = High, IgA = Low, IgE = Low. I have yet to see my immunologist for follow-up.
I recently started doing the liver flushes with malic acid, Epsom salt and olive oil based on Dr Hulda Clarke / Dr Andreas Moritz. I have been getting lots of “greenies” out with every BM for months now, even without taking any supplements for it. I take a boatload of supplements every day (adding to the stearic acid burden). I have also tried doing parasite flushes but so far have been unproductive; though it seems one must experiment with many different herbs/drugs sometimes. I am also looking into NeuroTherapy / NeuroFeedback to regulate my nervous system and brain, as well as Quantum Biofeedback (for anyone unfamiliar with this, it uses a machine that recognizes the unique vibration of hundreds of different chemicals in the body and finds any that are out of whack and actually helps the body to regulate them, which is helpful for a variety of hidden toxicities and imbalances).
Thanks so much for your advocacy and inspiration! I look forward to reading all your posts and trying your recipes!
Megan says
Hi Sierra, thank you for your kind words and for sharing. Yes, we’re a sort of family it seems, those of us who’ve had these long toxic histories and all the symptoms to show for it. It sounds like you’ve hunted down some accurate causes. While your beta carotene stint can certainly account for many symptoms, as can heavy metal and mold exposure, one of the best things about the diet and working with Dr. Smith, or doing the DIY version of his work, is that it includes all this and more. Many folks in the forum have had Lyme, MCAS etc, and so there are many variations to meet each individual’s situation. I would also recommend DNRS brain re-training. It’s excellent for all those little side symptoms and causes that you could spend a fortune hunting down; it retrains the brain, and can make it all go away. You can check out the website. Best wishes on this very very hopeful journey! So glad I can help a little.
Sierra says
Thanks for your thoughtful reply, Megan. I actually did the Gupta Brain Retraining program and found a lot of benefit from it. I will continue looking into VAD in the meantime.
Megan says
Good to hear, Sierra! Okay, sounds good. Also consider DNRS, possibly, as it seems even more beneficial. That’s just based on my own process of choosing between the two, as well as two friends who’ve done the Gupta and told me about it and their experiences. It seems to take “patients” only halfway to healing, whereas DNRS seems to take people the whole way or 95% there. Glad you’re interested in VAD. 🙂
Krysta MacGray says
Hi Megan,
Thank you for this informative and thorough article! It’s very intriguing. It is a lot to take in, so forgive me if I am getting something wrong in my questions. It seems that there are “phases” to the VAD diet, is that true? For example, it sounds as if you reintroduced sourdough bread and white rice after months of not having it in initial detox, is that accurate? If so, are the foods lists you’ve provided what is allowed during the initial detox and how do we know what we are allowed to add in later phases? Is there a how to guide of some sort?
Also, I’m just trying to wrap my head around different information after reading the opposite for years, but is the VAD diet gut healing and will it help to resolve food sensitivities? On both AIP and GAPS I have only ever been able to reintroduce one food group–dairy (cultured, grass fed butter, 24hr yogurt, 24hr sour cream, kefir) and I never had much of a reaction to those anyway, so I’m not even sure I “healed” enough to be able to finally tolerate them on those diets or if I was not sensitive all along. I still react to every other food that is reintroduced. Aside from symptoms, my biggest driver in getting well is being able to expand my diet and being on such restrictive diets for long periods of time is difficult. Can VAD help with this? I just have such a hard time believing sourdough bread and gut healing are compatible, but then again, I have been indoctrinated big time by autoimmune diets 🙂 I just want to know the truth.
Megan says
Hi Krysta, your first question sure reminds me of my first months and time with the GAPS diet lol ;). No, there is no official intro time or phases on the VAD diet, but it can be tailored for each person’s individual health situation, which encouragingly usually changes as you begin. For me, progress was fast. So I started with a low histamine version of the diet that I figured out for myself and then added grains and other foods as soon as I could. Each person should choose what foods they can tolerate to start with from the full list and start there. If you can tolerate all the foods, then that’s great, too. Yes, the diet is gut healing. As the diet cleans out the bile ducts of the liver, the bile itself stops getting into the bloodstream and causing damage. Plus, we eliminate other damaging compounds, such as sulfuric foods, which break down the GI lining. So even though the diet can be called VAD or Low Vitamin A, it really is so much more that FULLY leads to and is integral in healing the gut. This is why I couldn’t get gut healing from any other diet (such as GAPS): not just because those diets include foods high in vA, but also because they push foods high in sulfur, copper, aldehydes etc. Yes, food sensitivities will go away, but each person’s time frame is different. Yes, VAD will help you be able to add lots of foods back in (for example, I now enjoy croissants from a lovely French bakery once a month with no symptoms, and we go out for ice cream for special treats …), but it is not a fast diet either. It does take time. While I can eat real croissants and good ice cream now, it will still be a while before I eat “everything” again. I won’t eat foods with vA or copper until my body has fully detoxed them, and then I can occasionally if I choose. Certainly, same for sulfuric foods, all dairy etc. It will take time. The liver does not detox quickly. But I personally know that this approach is the right one, so I find contentment with my little treats and all the foods I can have. For example, I now eat oats, beans and rice daily, and I just love these staples. Prior to the low A diet, I had not eaten grains for 10 years. I am definitely happy, although, sure, I miss a few foods. Right, re sourdough, no anti-nutrients, ancestral flour from Italy, no high sulfur from whole grain wheat etc, low copper, low A … and the souring process has mellowed the gluten. It’s gentle. 🙂 But, I like your questions, and I hope you get to see for yourself. Your skepticisms are similar to how I felt, too! In some cases, it took me years on the diet to finally agree with a point, and then I just experienced it to a level that it was finally fully evident. Like you said, after years of believing the other messages, it’s very hard to switch the mindset. Yes, keep seeking the truth, and I’m so glad you’re here and learning all you can about this approach.
Guillermo Valarezo says
Hi Megan!
It’s been a long, long time from the last time I wrote… hope you’re doing well!
I have the following questions:
Which is the proper time and dosage to take activated charcoal? And, how often it has to be done?
In advance, thank you so much!
Megan says
Hi Guillermo! Nice to hear from you, and yes, doing well here. I hope you’re well, too. Based off of Dr. Smith’s work, I think it’s best to take activated charcoal before bed. I stir mine (the bulk AC) into my potassium water, and take my Mg and zinc pills with it. The reason is that many/most people have a bile dump during the night, so this way, the AC is there to adsorb any toxins from that bile. For some people this even helps with sleep, as that 3 am bile dump causes insomnia for some. I take the equivalent of 2 capsules, which is one scoop of this bulk brand (it’s the best because it’s hardwood sourced). I do just once daily. Dr. Smith does advise people to take more IF it doesn’t cause any constipation; so that’s the challenge, is increasing can cause constipation. But more is better otherwise, because more toxins are sopped up. So you can just make sure you’re taking enough Mg, potassium and fiber to have regular bowel movements. Best!
Jody says
Hi Megan,
Is white carrots low vitamin A? Since it has no pigment. Is there any beta carotene? Like white corn is compared to yellow corn? White is on low vitamin A list of food. Where do white carrots fall?“
Thank you,
Jody B.
Megan says
Hi Jody, happily, white carrots are allowed! I eat them regularly. 🙂
Anna says
We just celebrated a year of A. We celebrate because it saved our lives, literally, to take out the poison. I won’t say that it has been easy, but the hard part is not the diet itself. It’s super simple and easy. The hard part is the experience of eliminating so much poison. When you understand the relationship of retinol to ethanol (similar), you really that the mental and emotional effects are not too dissimilar either.
I didn’t notice a discussion of copper, but I think it needs to be mentioned. It’s the VA analog of the minerals. Very toxic, wicked stuff to eliminate, and very damaging.
We also use an array of supplements that become more critical during this detox.
Minerals get used up quickly in the elimination and the rebuild.
Molybdenum and selenium are critical for ALDH to function, and potassium and zinc are essential for copper to leave the body. Potassium is very tricky to maintain; we have needed to supplement close to the RDA.
We use coenzymated B-1 and niacin to aid the detoxification, and a lot of charcoal in topical and oral forms.
Lactoferrin is useful, maybe essential.
So much to learn from GG and GS!
Megan says
Yes, love the mention of GG and GS. Involvement in Dr. Smith’s forum is almost essential for getting one’s supplements right, but Grant did it so simply and amazingly, too. I’m so happy for your celebration and progress, Anna! Thanks so much for sharing.
Guillermo says
Hi there, Megan! Hope you’re doing well!
It’s been quite a long time since my last comment, though… anyways, thank you beforehand for your kind attention!
Would you mind giving your comments in regards of alfalfa? Is it VAD safe?
Cheers!
Megan says
Hi Guillermo, indeed! Alfalfa is not allowed. Off the top of my head, too many undesirable minerals, including copper. Cheers!
Sara says
Hi Megan!
I’m just exploring some of this to see if it can help my family, and I have a few questions for you:
1) Do you know if castor oil is beneficial to use for liver support? I know some oils are high in vitamin a, but I can’t find any information on this and am curious if you know if it’s helpful or harmful in this case.
2) What do you use for a moisturizer? I have used coconut oil and homemade tallow balm for years, as well as tallow soap. Just wondering what you use, if you are avoiding some of these.
3) My 18 month old daughter cannot have any dairy. It seems like butter/ghee are the main sources of cooking fat? What would you use if dairy is out for cooking family meals right now?
4) Were you done nursing/having children when you started this journey? I’m currently still nursing my daughter and would like to continue to grow our family. My health and her health are not in a great place, and I’m hoping to improve them before having another, but I also don’t want to spend five years on a detox diet and put off having another child. Do you know any families that have continued to grow as they go through the process of healing their liver from excess vitamin A? I’m just curious if there is any hope for us to heal, while also having more children.
Megan says
Hi Sara, happy to help. Starting with your last question, Dr. Smith advises going slowly if you haven’t started the diet yet and you’re nursing or very slowly if pregnant – so it’s okay to reduce copper and vitamin A, but you don’t want a major detox while doing either. If you can begin fully right when you wean and before you conceive again, then there’s no problem getting pregnant or nursing after you get through an initial detox to continue, as long as you’re taking activated charcoal, and gently correctly supplementing with things like zinc and molyb, to grab the copper etc. Re cooking fats: refined olive oil or avocado oils are best; avoiding all dairy is best. For moisturizing: Castor oil + jojoba oil are a great combo for most skin needs. Shea butter can be good for lips or DIY mixes. Re castor oil for liver, activated charcoal poultices are better, more effective and recommended.
Sara says
Okay, thank you, Megan!
Megan says
You’re welcome! 🙂
Rita says
I see that organic almonds are ok. Does that mean we can use almond flour?
Megan says
Yes, Rita, organic blanched almond flour, in moderation. Everyone is different, so just be aware of how your body responds to nuts. None of us wants too many omega 6 fatty acids. Here’s the best sustainable one that I buy repeatedly: https://amzn.to/4aKjrpF
Rita says
Thank you so much! I really appreciate you getting back to me so quickly!
Megan says
My pleasure!
Anne says
Hi Megan! I’m so glad I found your blog! I have a few questions about the allowed foods:
1. Is white flour, non-enriched of course, allowed? I see you mention sourdough bread, but what about normal bread made with white flour and no eggs?
2. Is it okay to have non-dairy yogurt like coconut yogurt? What about non-dairy cheeses?
3. What about edamame?
Thank you!
Megan says
Hi Anne, so glad you’re here, and I’m sorry for the delay in responding; I got behind!
1. You could do a small amount of clean white flour that’s not soured, like King Arthur brand, organic, or an organic brand from Italy, made into bread that isn’t soured, but there are some benefits of sourdough, and one of the main ones is that it affects blood sugar levels less than yeasted unsoured breads. Re glycemic index and glycemic load, sourdough bread has a GL measurement of 8 and a GI measurement of 54, whereas regular white bread has a GL of 9 and an GI of 71. (Overall, any white bread will deplete thiamine [Vitamin B1], so it’s not recommended to make it a staple, or be sure to supplement B1 in food or pill, depending on your body.)
2. Unfortunately, all yogurts (and other ferments) contain aldehydes, a compound that slows liver detox significantly. It depends on the recipe for non-dairy cheese, but all that I’m familiar with would have either an ingredient or a compound that would stand in the way of a smooth detox process.
3. Edamame are soy, so they are a big No: estrogenic, hormone altering, and the green indicates vitamin A.
Happy to help, but sorry, too. Thankfully, the other Yes foods get pretty great over time as you find your stride and new eating patterns.
Anne says
Hi Megan!
Also, for someone who is trying to decrease VA, could Siggi’s Skyr be a good alternative to traditional yogurt? It’s fat-free yogurt from grass-fed cows and lists 0% of VA.
Thanks!
Megan says
The absence of fat is surely a good thing, but the aldehydes are still there, and all dairy is a source of vA even if it’s a precursor; it then turns in to vA in the body. Better to miss it for a while, and then overcome the craving. You’re not alone. Many of us have been so so sad to stop eating yogurt and dairy, me included!! But it’s worth it.
Hihi says
Hi, this is so interesting to consider!
I had a question about the liver and ferments. I had a friend who’s son was on pain pills in the hospital for a major injury. When he drank the popular brand of kombucha in the bottles, the effectiveness of his pain pills would decrease to the point that she decided not to give him any more kombucha until after his intense pains were gone.
Can you explain this? We assumed the kombucha was allowing a detox, I would assume the metabolism of pain pills is in the liver? I understand there are a lot of things involved in detoxing, metabolic pathways and alleles and specific genetic factors. But since you are a va nerd and have said ferments hamper detox (or only va toxicity?) I am interested.
Please don’t worry about giving too much or too detailed of an answer, and thank you for your time and research into all this va stuff!
Megan says
Hello Hihi, and I’m sorry for the delay in responding. I just now saw your comment. In the case of kombucha, I suspect it has more to do with the aldehydes in it. Aldehydes interfere with medications, (and they also impede detox). Thank you and best!
Sarah says
This is SO incredibly helpful. Thank you Megan!!
Megan says
I’m so glad, Sarah! You’re welcome! 🙂
Stacy says
Hi Megan,
One more question…I don’t know if I have high oxalates or histamine, and it seems many of the recommended foods on the detox vitamin A diet are counter to the other diets. Which diet to do first?!
Thank you!!!
Megan says
Sure, try to combine or overlap the diets so you have your own unique diet that works for your body, with no symptoms, just for short term progress, to start. For example, I started the Low vA diet also low histamine. I ate egg whites, sauteed mushrooms and peeled russet potatoes. That low inflammation approach worked so fast that I was able to add in beef in less than a month. While I wouldn’t recommend someone on a low A diet eat egg whites or lots of potatoes in general, both those foods were fine as far as vA goes; it’s just that one is sulfuric, one is high-ish in copper, and the other is a nightshade. BUT, it doesn’t have to be perfect. We’re just looking for what it takes to be low vA and low histamine/low oxalate for long enough that the body can recover and get its footing to make progress. I hope that helps! Send me back your specific foods if you need more help. Which Low vA foods leave you with no symptoms?
Stacy says
Hi Megan,
I greatly appreciate your responses. On the low vA diet, I can eat chicken, barley, lettuce and peeled cucumbers. I’m also able to handle oats and eggs and cottage cheese. I get severely constipated without fiber from vegetables, so I’m hoping to work that out as well.
Thank you!!
Stacy
Megan says
Hi Stacy, very happy to help. This is great, actually, the number of foods you can eat. You can make a chicken and barley soup as a staple. Do you have an instant pot? Or eat them separately if you prefer, or both. You can also roast chicken, for variation, or make ground chicken patties, which are good for breakfast (if the ground chicken is very fresh, so low in histamines). For the low histamine version of all those, you’d need to make something, and then freeze and defrost all the leftovers to keep them from aging. I think you are familiar with this process? And hulled barley is recommended on the diet, plus lower in oxalates. It is likely you can make a tweaked version of these oat waffles: https://eatbeautiful.net/easy-oat-flour-waffles-gluten-free-vegan/ You can sub barley flour for the almond flour: https://amzn.to/47Hib7e What fiber foods might you tolerate for keeping regular, two good options: apples, low histamine beans (most are); can you eat either? The lettuce, cucumbers, occasional egg whites are all good. I’d avoid egg yolks and the cottage cheese entirely, as it’s not low A, and all dairy ends up complicating the process. However, if you’re brand new to the diet and just starting and it seemingly agrees with you, you could keep it in for now, in moderation. If the waffle recipe works for you, that will also be good for digestion, as would a daily bowl of oatmeal, depending on if your body does fine with two servings of oats a day, or prefers just one. Thoughts?
Stacy Fleischman says
Hi Megan,
I would very much like to set up a time to speak with you, so I can begin my journey of recovery and healing with more formal support. I greatly appreciate all the advice and online information so far! Please let me know if this will work for you.
Thank you so much!
Stacy
Megan says
Hi Stacy, yes, I’d be happy to. You can email me at [email protected], and we can find an appointment time. 🙂
John says
Hi Megan,
I was wondering what your thoughts are on bouillon, specifically this ‘Better than Bouillon’ product. It’s sitting in my refrigerator and appears to be low vitamin A/copper. I’m aware it’s probably not the healthiest product in the world, but I’m thinking it may be okay to use once in a while.
I didn’t see anything on this document mentioning bouillon, so I thought I would inquire.
Thank you for your feedback,
John
Megan says
Hi John, it does contain turmeric (and soy), so even though it isn’t thrifty, I’d move it along. If you want something for the same purposes, you could try Bone Broth Powder HERE. It has just one ingredient if I remember correctly. It is expensive, but I have a bag in my pantry for the situation you described, which is very occasionally when I need it. If you decide to get it, at checkout, use code MEGAN15 for 15% off your order. 🙂
John says
Hi Megan,
I’m so glad I found your site. There’s such a wealth of information here. Thanks for keeping it up to date and making it easy to find things like your recipes.
I’ve been on the low vitamin A diet for about a month now. I’m already noticing some clearing up of my dry, cracked, peeling feet, especially on my soles. I’ve pretty much elimanted most sources of vitamin A the best I can, considering I ate massive amounts of carrots, eggs, tomatos, salmon, avocados, broccoli and more over the last couple of decades, but not anymore.
The only known sources of vitamin I’m consuming now is from green beans, celery and romain lettuce. These foods are on your good foods list, but are still sources of vitamin A. Considering all the foods I’ve eliminated, I think it’s enough to shift the balance in my favor while still consuming these 3 foods in modest amounts. Also, I see Iceberg lettuce might be a better option for consuming lettuce.
Thank you in advance for your thoughts on this.
John
Megan says
Hi John, that’s correct! Great job!! I’m so glad you found the website and low vitamin A diet, too! (I apologize for the long delay in responding. My mom passed away unexpectedly, and it’s taken its toll on my body and ability to work.) Great that you’ve seen improvements in your cracking feet. This symptom is actually a common one with vitamin A toxicity. So where you are now, with the foods you’re eating, is a great place to stay. Or, if you ever choose to eliminate the green beans and romaine and any darker celery, that’s good, too. Let your unique body, temperament and intuition be the guide. You will keep making progress with your current diet. I got to the point after 6 years that I stopped with all green foods just because now I’m working on deep vitamin A, and even small amounts affect me more now. I’ll be here if you have questions over the coming months or years. It’s a great journey!! I hope you’re doing hardwood activated charcoal, too?
John says
Hi Megan, Thanks for the reply. I’m sorry to hear about your loss. Thanks for pointing out that cracking feet are common with vitamin A toxicity. I also noticed some chest acne disappear, probably because of all the eggs and cheese I was consuming.
Now after listening to many of Dr Smith’s livestreams, I’m starting to think I’m copper toxic as well. I noticed even 10mg of zinc will give me a reaction I don’t tolerate well. I’ve since moved down to 5mg which seems to be fine.
Thanks for all the other fine points, and good luck in your journey in 2026 and beyond. And no, I haven’t started the activated charcoal yet, but will think about it now.
John
Megan says
Hi John, thank you. Yes, copper ends up being a big part of most people’s detox journeys, even though most of us could not have anticipated another villain as bad as vA. Good for you, fine-tuning your zinc dose, sounds perfect. When you’re ready, molybdenum (usually 150mcg) is another antagonist to copper. Best!
John Damone says
Hi Megan,
I am considering the activated charcoal as you indicated in one of your earlier replies. I’ve been looking for something to help me with my 3:00AM bile dumps, which have a tendency to wake me with some discomfort on occasion. And I may have some IBS to go along with this.
Since I’m very wary and hesitant to push things with additional supplemets (zinc, magnusium, molyb, etc), plus I’m hyper sensitive, my thinking is why not start with the charcoal before introducing anything else?
Thank you for your thoughts on this, John
Megan says
You’re welcome, John. I hope it helps. You may need to play around with dosage and very gradually increase your nighttime dose before bed, over time, making sure you stay regular (with dietary fiber, magnesium and potassium). I started with 1/2 teaspoon charcoal. It’s good it’s an affordable supplement and that it adsorbs vitamin A and other toxins; like you said: why not start with it, when it gets rid of toxins? It agrees with most people, but not everyone; so you can be aware.
Matt says
I live in the Uk and am on a low vitamin diet. i seem to be doing well with semi skimmed milk. Here it is not fortified with vitamin A. Do you think this is ok in conjunction with a low vitamin a diet
Megan says
Hi Matt, great to hear about you doing a low vA diet! Sadly, no, on the milk. It can work at first, if you’ve removed so many other sources of vA that your body is thrilled for the decreased burden. I kept eating cheese for probably 6 months, in small amounts, and still made progress. But, eventually, all dairy has casein, or it’s a carrier for vitamin A, or there’s some vA compound in it that sabotages. I’d find or make the best clean Oat Milk. We love it now, although it was hard at first. Best!
Annamaria says
Hello, you wrote an excellent article and I subscribed to the newsletter. However, it seems to me that you missed the fact that Grant also wrote a third e-book, “Breast Cancer”. Perhaps you could add it to the article, as many women might be interested.
Greetings from Italy
Megan says
Thank you, Annamaria, indeed! I didn’t include that one because it’s a very specific topic instead of an intro and overview of vA toxicity in general. So glad to have you here, and thank you again. How lovely that you’re in Italy!