I may receive a commission if you purchase through links in this post. I am not a doctor; please consult your practitioner before changing your supplement or healthcare regimen. As an Amazon Associate I earn from qualifying purchases.
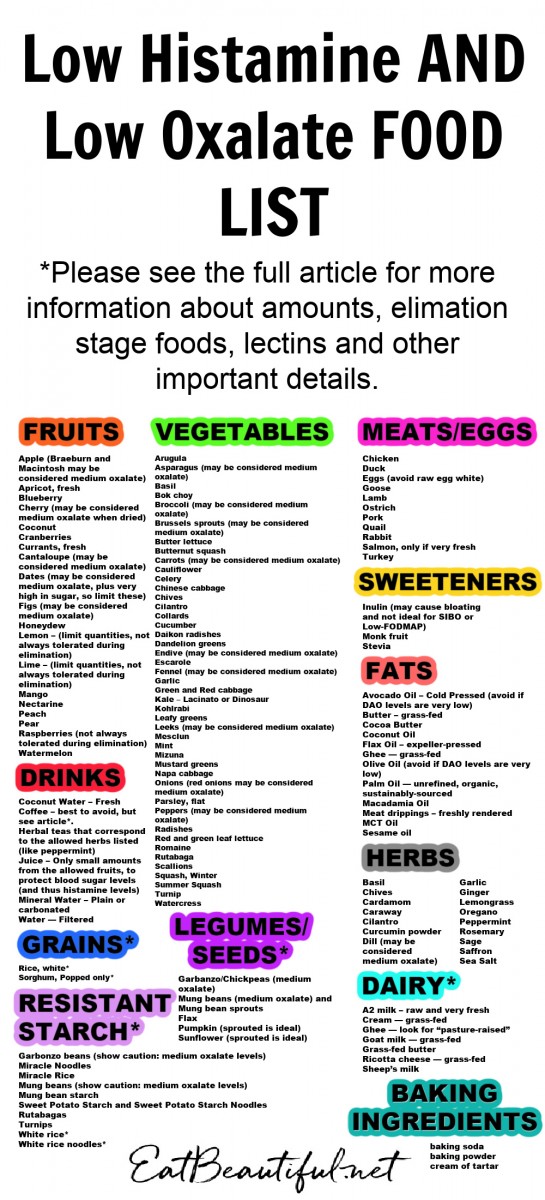
This post provides a combined Low Histamine AND Low Oxalate food list, with a printable — for easy cooking and grocery shopping.
I created this list in part for myself, because it makes recipe creating so much easier — to have low histamine AND low oxalate foods listed in the same place.
Additionally, I have used the (L) sign to indicate which foods may be high in lectins.
Whether you use this list to cook or grocery shop, find the printable for your reference here. Or pin the image below.
You can find a Low-Histamine and Lectin-free Combined Food List and printable here.
The role of Vitamin B1
Certain dietary deficiencies likely cause or contribute to histamine intolerance and oxalate sensitivity. It may be that the Western diet, high in white flour and white rice-based carbohydrates, causes a thiamine (B1) deficiency. (source)
If problems with histamines and oxalates are a warning sign of a nutrient-deficient diet (or impaired digestion of nutrients), it’s helpful in our conversation to include information about:
- foods that further deplete B1
- and foods that are high in B1.
So, below in our food lists, I’ve added notes about B1. Please consider eating foods high in B1, talk to your doctor about supplementing and avoid foods that deplete B1.
Ironically, sulfur-rich foods have also been implicated in depleting B1. So while a nutrient-dense diet usually espouses many sulfuric foods (like cruciferous vegetables), I personally believe these vegetables can impede detox pathways. It may be best to avoid them while trying to heal from oxalate and histamine issues. (source and source)
Many sulfur-rich supplements also deplete the body of B1.
Polyphenols in plants can also deplete dietary B1. You can eat sources of B1 and polyphenols in separate meals to avoid this. (source)
Low Histamine AND Low Oxalate Gluten-free Grains
- Rice, white (L) (Avoid white rice products unless conscientious of thiamine deficiency. I.e. can supplement with B1, eat allowed beans, sunflower seeds in moderation etc.)
- Sorghum, Popped only – (A very small amount may be fine for lower oxalate, about 1/2 cup.)
Low Histamine AND Low Oxalate Vegetables
- Arugula (sulfuric: may deplete B1)
- Asparagus (possibly medium oxalate; B1 source)
- Basil
- Bok choy (sulfuric: may deplete B1)
- Broccoli (possibly medium oxalate, sulfuric: may deplete B1)
- Brussels sprouts (possibly medium oxalate, sulfuric: may deplete B1)
- Butter lettuce
- Butternut squash (L)
- Carrots (possibly medium oxalate; B1 source)
- Cauliflower (sulfuric: may deplete B1)
- Celery
- Chinese cabbage (sulfuric: may deplete B1)
- Chives
- Cilantro
- Collards (sulfuric: may deplete B1)
- Cucumber (L, peel and de-seed to reduce) (B1 source)
- Daikon radishes (sulfuric: may deplete B1)
- Dandelion greens
- Endive (possibly medium oxalate)
- Escarole
- Fennel (possibly medium oxalate)
- Garlic (sulfuric: may deplete B1)
- Green and Red cabbage (sulfuric: may deplete B1)
- Kale – Lacinato or Dinosaur (sulfuric: may deplete B1)
- Kohlrabi (sulfuric: may deplete B1)
- Leafy greens (some are sulfuric: may deplete B1; does not include spinach or Swiss chard which are very high oxalate)
- Leeks (possibly medium oxalate)
- Mesclun
- Mint
- Mizuna
- Mustard greens (sulfuric: may deplete B1)
- Napa cabbage (sulfuric: may deplete B1)
- Onions (red onions possibly medium oxalate; sulfuric: may deplete B1)
- Parsley, flat
- Parsley Root
- Peppers (L) (possibly medium oxalate)
- Radishes (sulfuric: may deplete B1)
- Red and green leaf lettuce
- Romaine
- Rutabaga (sulfuric: may deplete B1)
- Scallions
- Squash, Winter
- Summer Squash (L, peel and de-seed to reduce) (B1 source)
- Turnip (sulfuric: may deplete B1)
- Watercress (sulfuric: may deplete B1)

Low Histamine AND Low Oxalate Fruits
Most fruits contain lectins. So if you’re also avoiding lectins, you may wish to avoid all fruit to start and then gradually increase the fruits below that don’t have the (L) sign. Out of season fruits and high-sugar tropical fruits are also best to avoid.
- Apple (Braeburn and Macintosh possibly medium oxalate.) (Peeled for low-lectin)
- Apricot – fresh (L)
- Blueberry
- Cherry (L) (possibly medium oxalate when dried)
- Coconut
- Cranberries (L)
- Currant, fresh (L)
- Cantaloupe (L) (possibly medium oxalate)
- Dates (possibly medium oxalate, plus very high in sugar, so limit these)
- Figs (possibly medium oxalate)
- Honeydew (L)
- Lemon – (limit quantities, not always tolerated during elimination)
- Lime – (limit quantities, not always tolerated during elimination)
- Mango (L)
- Nectarine (L)
- Peach (L)
- Pear (L)
- Watermelon (L) (sulfuric: may deplete B1)
Low Histamine AND Low Oxalate Meat & Eggs
If you’re also avoiding lectins, be extra sure to choose pasture-raised meats.
- Chicken
- Duck
- Eggs (avoid raw egg white)
- Goose
- Lamb
- Ostrich
- Pork — Pork is low histamine if it is fresh or fresh frozen. Ground pork is riskier, depending on the source, and preserved pork, like bacon or ham, are high histamine. Pork does not need to be aged, so if you connect with a farm, butcher or raise your own, it can be butchered and frozen immediately.
- Quail
- Rabbit
- Salmon, only if very fresh
- Turkey
Note: Beef and Buffalo are usually high histamine foods because the meat is aged before butchering. If you can access un-aged beef or bison that are slaughtered, butchered and frozen quickly, the meat is low histamine.

Low Histamine AND Low Oxalate Beans/Legumes
Because beans are an excellent source of B1 and fiber, I think it’s ideal to introduce them as soon as they’re tolerated. Beans absorb toxins and may produce detox symptoms when you first introduce them to your diet.
- Garbanzo/Chickpeas (L) (medium oxalate; great source of B1)
- Mung beans (L) (medium oxalate; great source of B1) and Mung bean sprouts
All other beans are high oxalate, but most are low histamine if freshly pressure cooked, with the exception of lentils and peanuts.
This chart helped me to determine which beans I digest best.
Low Histamine AND Low Oxalate Seeds
- Flax
- Pumpkin (L) (sprouted is ideal)
- Sunflower (L) (sprouted is ideal) (B1 source, but can change hormone levels, so observe and don’t overdo)
Note: Most nuts are high oxalate. Macadamias, pecans and pistachios are medium oxalate, (but pistachios usually have major mold issues. I avoid them).
Low Histamine AND Low Oxalate Fats and Oils
- Avocado Oil – Cold Pressed (Avoid if DAO levels are very low.)
- Butter – grass-fed
- Cocoa Butter
- Coconut Oil
- Flax Oil – expeller-pressed
- Ghee — grass-fed
- Olive Oil (Avoid if DAO levels are very low.)
- Palm Oil — unrefined, organic, sustainably-sourced
- Macadamia Oil
- Meat drippings – freshly rendered
- MCT Oil
- Sesame oil

Low Histamine AND Low Oxalate Herbs and Spices
- Basil
- Chives
- Cardamom
- Caraway
- Cilantro
- Curcumin powder (a good substitute for turmeric, which is high oxalate)
- Dill (possibly medium oxalate)
- Garlic
- Ginger
- Lemongrass
- Oregano
- Peppermint
- Rosemary
- Sage
- Saffron
- Sea Salt
Low Histamine AND Low Oxalate Sweeteners
It’s important to reduce sweets when managing histamine issues: any foods that increase blood sugar levels also increase histamine levels.
However, most fruits are safe to eat, so you can sometimes approach treats by either just enjoying fruit or using it as a sweetener.
I think it is best to avoid all of these, but for reference, sweeteners that do not affect blood sugar levels are:
- Inulin (May cause bloating and not ideal for SIBO or Low-FODMAP.)
- Monk fruit
- Stevia
Although not recommended during elimination, very small amounts of Coconut Sugar may also be tolerated.
Low Histamine AND Low Oxalate Baking Ingredients
- baking soda
- baking powder
- cream of tartar
Low Histamine AND Low Oxalate Beverages
- Coconut Water – Fresh
- Coffee – Best to avoid, but see below*. (sulfuric: may deplete B1)
- Herbal teas — That correspond to the allowed herbs listed above (like peppermint)
- Juice – Only small amounts from the allowed fruits, to protect blood sugar levels (and thus histamine levels)
- Mineral Water – Plain or carbonated
- Water — Filtered
*If you feel you need coffee, look for mold-free brands like Clean Coffee.
Low Histamine AND Low Oxalate Dairy
I avoid most dairy that’s not A2A2. The exception is butter from companies like Kerrygold that have part A2 herds and good husbandry principles. While my body is very sensitive to A1 dairy, I do well with Kerrygold. I also do fine with any dairy out of France.
If you’re avoiding lectins, most dairy should be avoided. Fresh, raw A2A2 milk and butter are the exceptions.
- A2 milk — Raw and very fresh (For me, within 3 days of milking, but this will vary person to person.)
- Cream — Grass-fed
- Ghee — Look for “pasture-raised”
- Goat milk — Grass-fed (Try to connect with a local farm for the best quality, and ask questions about the extent to which they’re allowed to browse and eat plant life. Not all goat milk is healthy.)
- Grass-fed butter — Preferably Kerrygold, from France or homemade
- Ricotta cheese — Grass-fed
- Sheep’s milk

Low Histamine AND Low Oxalate Resistant Starch Foods
The ingestion of prebiotic foods (resistant starch containing foods that are consumed by our good gut flora) may help protect the body against oxalate damage. Including RS foods in one’s diet may be one step toward achieving balance in the body.
If you have SIBO, undiagnosed bloating or are on a low-FODMAP diet, avoid foods that contain resistant starch.
- Garbanzo beans (Show caution: medium oxalate levels; B1 source.)
- Miracle Noodles
- Miracle Rice
- Mung beans (Show caution: medium oxalate levels; B1 source.)
- Mung bean starch
- Sweet Potato Starch and Sweet Potato Starch Noodles (Sweet potato starch is low oxalate, but avoid sweet potato flour, which is high oxalate.)
- Rutabagas (sulfuric: may deplete B1)
- Turnips (sulfuric: may deplete B1)
- White rice (Avoid white rice products unless conscientious of thiamine deficiency. I.e. can supplement with B1, eat allowed beans etc.)
- White rice noodles (Avoid white rice products unless conscientious of thiamine deficiency. I.e. can supplement with B1, eat allowed beans etc.)
The role of Vitamin A
Personally, I found healing from MCAS and lectin sensitivity by reducing my consumption of vitamin A, which is controversial, but nonetheless, has been life-changing for me. You can read more about my recovery here.
You can PIN the chart below or print it. 🙂


Juniper says
So glad to have found your site! Thank you for the list for both histamine/oxalates. Explains a lot of my weird symptoms Sunburnt skin without sunburn. Do you have any suggestions what to use for face? I’ve tried coconut oil, olive oil, shea butter. Face is skin tight if nothing on. Oils I mentioned will cause itch. Doc cream feels good then whole face starts peeling and cycle again. The recipes look delicious! Thank you so much!
Megan says
Hi Juniper, yes, I use and love castor oil. It’s wonderful. I also recommend you look into the concept of vitamin A toxicity for possible cause and long term solution: https://eatbeautiful.net/vitamin-a-detox-diet-free-printable-food-lists-avoid-eat-toxicity/ Best wishes!
Juniper says
Thank you Megan! I will give castor oil a try. Just placed order for Grassfed gelatin, hydrolyzed collagen and Magnesium. Didn’t know to look for “grassfed” until finding your site. So nice to find a supplement that does not have additives even with the capsule form. Appreciate the discount code and all your knowledge. Abundant blessings and thank you for making healthy food delicious!
Megan says
Thank you, Juniper, so sweet, and you’re welcome. 🙂 Great, I’m glad you’ll try out the castor oil, and I hope it’s a good fit for you. I’m so happy you learned about grass-fed and got the very best options out there. It’s hard to weed through all the hype and competition. Many blessings on you and yours too!! 🙂
JUniper says
Is bacon fat considered high histamine? Even the sulfite-free ones? We love them for cooking or can we use in moderation? Would love to try the apple bacon cookie recipe. Thank you!
Megan says
Hi Juniper, yes, unfortunately. Best to reduce histamines until you overcome the issue, then reintroduce. However, everyone with histamine issues reacts differently to different foods. So you may find that just the bacon fat in the cookies is not enough of a trigger for you and that you can maintain a low histamine diet with that one inclusion.
Jenny says
Hi. Can you tell me if purple sweet potatoes are a “no” for histamine/ oxalate issues? Trying to find some energy foods, as I’m a runner and i need more fuel than protein and veggies all the time. I’ve tried grains and oats but both seem to not sit well with me and my itchy skin issues. Thanks. Any advice would be appreciated. Any creative ways to bake root veggies? Also, which apples are safe to eat?
Megan says
Hi Jenny, how do you do with garbanzo beans and white rice? Any foods on the list are okay, so apples, but not sweet potatoes. Also, the seeds and fruits listed could work for energy.
Connie Harwood says
Hi Juniper, This sight is so helpful. Thank you ! My question is about mushrooms. Are they allowed on a low histamine diet? Not one of the sights I’ve searched has included mushrooms in their list. Thanks again for your help.
Megan says
Hi Connie, if it’s not on the list, then it’s not okay, so mushrooms are out.
James says
Mushrooms are high in histamine, guaranteed.
Miriam Moss says
Why are leafy greens on this list? They are considered high oxalate, especially spinach.
Megan says
Hi Miriam, thanks for the question. Leafy greens means an assortment of diverse greens, like lettuces, turnip greens, mustard greens, cabbage, collards, kohlrabi greens, boy choy, watercress and arugula. It does not mean spinach, which is usually referred to in food lists by itself, as it’s so well known and distinctive. Thanks for letting me know that my wording was confusing; I’ll clarify my intent above. 🙂 Swiss chard is also high oxalate, so I’ll clarify that as well.
Vanessa says
Hello thank you for this list.
A few questions
I don’t see zucchini on the list I thought they were low histamine and oxalate?
What about yellow squash ?
I am dealing with interstitial cystitis symptoms
Do you think that’s a histamine issue ?
Megan says
Hi Vanessa, you’re welcome. They are both included as summer squash: “Summer Squash (L, peel and de-seed to reduce) (B1 source)”. 🙂 Re IC, have you read this post: https://eatbeautiful.net/how-i-healed-my-interstitial-cystitis/ And also this one: https://eatbeautiful.net/vitamin-a-detox-diet-free-printable-food-lists-avoid-eat-toxicity/
Vanessa says
Also what are your thoughts on connect milk, coconut flour , coconut sugar and coconut yogurt?
Thank you 🙏🏻
Megan says
Hi Vanessa, coconut is indeed listed under the Low Histamine AND Low Oxalate FOOD LIST.
Vanessa says
Thank you so very much! I am going to contact the dr you listed. I think I have MCAS possibly from the va((ine. 😔 I just did some testing.
Megan says
I’m so sorry! Best wishes for full wellness!
Diane McKenzie says
My son as well has stomach issues I think from the same thing.
George says
Hello am glad l found ur site.. just wanted to ask you about arugula and watercress l heard they are both have lectins? Or all cruciferous vegetables have lectins? I thought arugula is rich in surfur aswel? Thanks
Megan says
Hi George, both arugula and watercress are low in lectins. No, not all cruciferous veggies are high in lectins. Yes, arugula is high in sulfur. 🙂
George says
Thanks for the reply Megan.. so does it means even arugula will deplete vitamin b1 just like broccoli since is high in sulfur too? I like arugula but just wanted to get my facts correct before l eat these vegetables blindly without knowing side it’s side effects.
Megan says
Hi George, happy to help! And great questions you’re asking. I’m going to update arugula above to show it’s high in sulfur, so thanks for helping me to see that I missed that. Yes, in my opinion, it’s best to eat foods like arugula in moderation or only occasionally/not at all. I think it’s wise of you to want to understand before re-building your diet.
George says
Yes wanted to know how these so called healthy vegetables like cruciferous vegetables can do to you despite being labelled as superfoods by most doctors out here but with little facts on how they can literally make you sick by suppressing ur thyroid not to mention depleting ur B1 as you mentioned on ur article. Thanks once l again l have book marked ur article as is very important and is speaking a lot of facts that most people won’t as lectins are one the demons that are making us sick silently out here. And l noticed you didn’t include mushrooms as low in oxalates? Is all mushrooms that are high in oxalates? Maybe l got so much trust with sally k Norton as she listed them as low in oxalates on her vegetables recommended list? What’s ur final say on mushrooms when it comes to lectins/oxalates? Or is just them common mushrooms like white button but maybe oyster mushrooms and other are low? And final question is about nettle leaves l make tea with them as they seem to be so beneficial but l see you haven’t included on ur list? Do you think they are high in lectins/oxalates? Thanks
Megan says
Hi George, agreed. The tests done on these foods’ compounds are so often poorly understood, as their interactions in the body are quite complex and impossible to recreate in labs. People without a sensitivity can handle some of these compounds in moderation, especially when food sourced. The real problem comes when we’re told they’re super foods that we should load up on + we may have a sensitivity, or when we supplement. Most doctors and nutritionists are not educated about the dangers of different compounds in vegetables or foods in general. Re mushrooms, white button mushrooms and shiitake mushrooms are both very high in oxalates, BUT the vast majority of those oxalates are insoluble. So, they won’t affect us and are therefore considered low oxalate. Oyster mushrooms are moderately high in oxalates and are mostly soluble, so should be avoided. Re nettles, they may indeed be beneficial. I have a unique standpoint on most “superfoods”, especially if they’re high in vitamin A. As we’ve implied, we so often rush headlong into the regular consumption of these foods without understanding all the complexities if eaten often. In this article on recovering from lectin and histamine issues, I talk about vitamin A’s possible relationship to these chronic sensitivities, and also share how I got well from these issues: https://eatbeautiful.net/mcas-histamine-lectin-intolerance-tips/ You may find it helpful.
Bee says
Wow, great article and food lists! The connection with b1 is very intriguing… Do you have a brand of b1 supplement (or b complex) you recommend thst is yeast free and well tolerated? I don’t have a colon and thus am more likely to be deficient in b vitamins, and the symptoms line up.
Thanks so much! I just discovered your website and am avidly soaking up the info you gave posted!
Megan says
Hi Bee, I’m so glad the article and website are helpful! 🙂 This is the B1 I take: https://amzn.to/3c1kqUM It does not say yeast-free specifically, but it does say it’s free of just about everything else, including gluten, so it may or may not work for you? I no longer do a B complex but add in B2 and B3 as needed. B complexes often contain one or more undesirable ingredient, too much of a shotgun approach. I hope that’s helpful?
mary stephen says
This is an excellent consolidated article : detailing the nutritional pros and cons, as well as the interactions with superfoods. I really thank the author for taking the trouble to provide us such valuable information that is of practical importance.
I hope you are able to keep up and carry on this good work
Megan says
Thank you, Mary, I’m so glad the article is helpful.❤
George says
Hello Megan, l hope ur keeping well, l just wanted to ask you more about lectins since l know they are second poison next to oxalates, with oxalates am able to understand them and know their damage than lectins as many people are saying if you buy organic vegetables like tomatoes or any produce that contain lectins it will be lectins free if it’s grown organically? What’s ur say on that statement? Do you think bring organic makes these vegetables lectins free compared to non organic? And what ur main lectin vegetables or fry that you must avoid to heal like is their others that have less lectins proteins than others? Thanks
Megan says
Hi George, unfortunately organic veggies do still have lectins. They are part of the plants’ defense systems, for organic or non-organic. Some veggies with lectins that you can reduce and still eat are cucumbers and zucchini. Both are good peeled and de-seeded.
George says
Hey Megan, thanks for clarifying that..what bout celeriac root is it low or medium oxalate like celery itself? Thanks
Megan says
Celeriac, or celery root, is moderate.
George says
But another thing since an trying to get more facts about oxalate or lectins, if someone is using cocoa butter lotion like palmers would it mean the lotion will have oxalates or lectins in it that it will affect the skin or absorbed via the skin? Because l saw ur post saying that u were eating cocoa butter and you felt not good then you stopped it you felt better, was that due to the fats or oxalates? And does that applies to using cocoa butter lotions on skin too? Thanks
Megan says
That was due to the stearic acid in cocoa butter. I think it’s best to stay with castor oil topically, or a few other ingredients or products that are thoughtfully chosen for topical use. Castor oil is really gentle and safe for most people.
Keith says
From what I’ve looked up, pork seems to be considered the main high histamine meat to stay away from. Is there a reason for this discrepancy? Thanks
Megan says
Hi Keith, you bring up a good point that I will clarify in the post. Pork is low histamine if it is fresh or fresh frozen. Ground pork is riskier, depending on the source, and preserved pork, like bacon or ham, are high histamine. Pork does not need to be aged, so if you connect with a farm or raise your own, it can be butchered and frozen immediately. I will add to the post! 🙂
April says
Is oatmeal ok?
Megan says
Hi April, good question. The oxalates in oats are controversial. They are low histamine. The most obvious issue with oats is lectins, which can exacerbate histamine issues indirectly. So, it’s possible on this diet to trial oats, and see how you do, but with caution.
Amanda says
April, I seem to handle steel cut oats nicely. I usually cook a big batch in my pressure cooker and then freeze them by individual meals. They’re great for a quick breakfast.
Patres says
Hi,
may I ask why are raspberries in the list under both low oxalate and low histamine foods? They contain 48 mg of oxalates per cup and they are high in histamines also, see:
Histamine:
https://www.mastzellaktivierung.info/downloads/foodlist/21_FoodList_EN_alphabetic_withCateg.pdf
Oxalate:
https://www.webmd.com/diet/foods-high-in-oxalates#:~:text=Many%20fruits%20contain%20some%20oxalates,with%2048%20milligrams%20per%20cup.
Megan says
Hi, and you are right. They are there by mistake and will be removed right now. Thanks for letting me know! They are high in oxalates, and somehow I missed that. Re histamines, different lists say different things, and that’s because “…raspberries are considered high histamine but have quercetin in them, which is an antihistamine. This accounts for some of the confusion, as a person googling antihistamine foods might come across raspberries because of the quercetin content, while a person googling high histamine foods would also find raspberries on the list.” -from healinghistamine.com
Lee says
Thanks for such great info. I sometimes sprinkle a 5 medicinal mushroom blend tincture on my food. Would this be high histamine?
Megan says
Hi Lee, the blend probably isn’t high in histamines, but there are other amines that can trigger a histamine reaction. In mushrooms, they’ve found putrescine and spermidine. Especially putrescine can tie up needed DAO. I would eliminate the blend to start with, and then challenge a little at some point to see how you do.
George says
Hey Megan l hope you been keeping well, l just wanted to clarify with ginger as herbs/spices since l saw many sites even that trying low oxalate group saying is high oxalate and cardamom too? And also l saw you didn’t include blackberry on ur oxalate/lectin article, do you think blackberry are low lectins as well as low oxalate? And ask what about tangerines and sour sop are these low oxalates? Thanks
George says
Hey and also just want to verify with winter squash like kombucha/delicata a do acorn squash are low lectins and low oxalates? Or it all winter squash are low lectins and oxalate? Thanks
carly stewart says
Hi there,
If i take glutathione will that help me process sulphur foods in my body better and me to eat more?
I definetly think i have oxlates issues and maybe salicyates im not sure.I am confused by my long list of fruit and vegetables i cannot have and why.I suspect maybe latex issues and have a diagnosis of mcas -mast cell activation and recent tests have shown infections,bacteria,mold illness in me.Im more reactive round mt time of the month and mainly 7/10 days before leading upto it.The only fruit and vedge i can eat with no swollen tongue,puffy cheeks,raction is orgainic brown onione,Orgainic garlic,Blueberries.I am so hungry.
Thank you for taking the time to read my post,
Best wishes Carly 🙂
Megan says
Hi Carly, personally I do not think glutathione plus including sulphuric foods is helpful. I would check out the posts on vitamin A toxicity and seek out the help of Dr. Smith, who is discussed in these posts: https://eatbeautiful.net/vitamin-a-detox-diet-free-printable-food-lists-avoid-eat-toxicity/ and https://eatbeautiful.net/my-exact-diet-supplements-for-vitamin-a-detox-my-progress/
Kim says
hi, am glad to find your colorful list, (although I do not have a color printer). What I really want to do is to print it BIGGER because its so small. is there anyway to do this? Please? Thank you so much! 🙂 bless you! and thank you for your blog post!! 🙂 Ps. Does it reflect that raspberries are not on there now?
Megan says
Hi Kim, you should be able to print it black and white and on a full size 8.5×11 sheet of paper. I personally did this. Is there someone you can ask to help you with your computer and printer? I’m glad the list is helpful! 🙂 Raspberries are considered high in oxalates.
Lara says
FINALLY! A list of things we CAN enjoy!!! Talk about depressing & discouraging when you are looking for what you CAN have, & all you ever find are websites telling you what you CAN’T have! Thank you, thank you, thank you!
Megan says
YAY, Lara!! That makes me so happy, too! So glad it’s helpful!
Lee Jenkins says
Thank you for your helpful information. I have Coeliac Disease and I am intolerant to salicylates, amines, glutamates, sulfites and sulfates. I was recently diagnosed with hay fever. I am trying to manage a low histamine diet whilst taking my other food intolerance into account. I wondered if you, or do you know of anybody, I could contact for help. I’m in New Zealand so it would probably need to be an online consultation.
Many thanks, Lee
Megan says
Hi Lee, yes, I highly recommend Dr. Smith. He’s the doctor that heads of the low vitamin A diet, which is what helped me (and others) completely overcome histamine intolerance (and many other things). It looks deeper at that actual cause of our issues, whereas most practitioners don’t know how to fully recover from the sensitivities you mention. Here’s his website where you’ll find contact information and introductory information, too: https://nutritiondetective.com/ He meets with clients remotely, including international clients. Best!
Lee Jenkins says
Thank you so much for replying, replying so promptly and with helpful advice.
Many thanks Megan, Lee
Megan says
My pleasure, and I’m glad it was helpful! 🙂
Lora Plavcan says
Hi Megan,
Thank you for taking the time to share this important information! I think I may have tyramine intolerance, may be sensitive to histamine and oxalates as well. I’ve been searching for info about tyramine foods, what to avoid, what’s safe, ect. and have found a few helpful websites; It seems to be easier to find info on histamine though. I have learned that some foods are high in both histamine and tyramine. Do you recommend any resources/consultations regarding tyramine? I’m hoping and praying to be able to get tested soon. It’s very challenging to do trail and error and end up with blood pressure spikes from certain foods.
Also, regarding dandelion greens, I’ve read that they are high in oxalates; please clarify. I have them growing wild, but have not eaten them because of this. Thanks again for all you do!
Megan says
Hi Lora, I’m sorry for your struggles. I’m glad you’ve isolated some of your triggers; that’s a good start, even though it’s a lot of work and hardship still. Dandelion greens are high in oxalates, from my reading. More than anything else, I recommend an appointment with Dr. Smith, who’s the leading expert on overcoming pretty much all health challenges through detoxing the liver properly of vitamin A and other toxins, as well as the body of copper. It’s amazing how many other conditions clear up when these issues are addressed, arguably THE root cause. You can find him here, and consider the group consult for less money if the financial side is a challenge. His price includes all lab work. https://nutritiondetective.com/ You can read more here about the low A diet: https://eatbeautiful.net/vitamin-a-detox-diet-free-printable-food-lists-avoid-eat-toxicity/ Best wishes!
Riva Francis says
I just want to say goats are not “pasture-raised” animals. They are browsers, not grazers, which means they do not eat grass they eat plants… Tree leaves and brush… bushes and such, naturally. That being said, you are never going to find “grass-fed pasture raised” goat milk products.