I may receive a commission if you purchase through links in this post. I am not a doctor; please consult your practitioner before changing your supplement or healthcare regimen.
Why Not Getting Wisdom Teeth Removed is Good looks at multiple scientific studies that directly conflict with what most of us are told when we go to the dentist: “There are no scientifically proven health benefits of pulling wisdom teeth that don’t cause any problems. What’s more, removing wisdom teeth is usually unpleasant and may cause side effects.” (source)
While impacted third molars can require surgery, prophylactic extraction of third molars may cause dangerous long term health conditions.
Of the 5 million extractions done each year in the U.S., tens of thousands of patients end up with lifelong discomfort and disability. Many of these end up with chronic infections that find harbor in their cavitations.
As one source says, “Avoidance of prophylactic extraction of third molars can prevent this public health hazard.” (source)
How many people actually need their wisdom teeth removed?
An NIH conference on “Removal of Third Molars” concluded, “Some type of pathological change can be expected eventually in approximately 12.0% of an impacted 3rd molar population and 1.82% of the general population.” (source)
In this article, we look at:
- necessary reasons to have wisdom teeth removed
- reasons to consider waiting or avoiding this surgery
- less-discussed dangers of the procedure
- alternatives to surgery
Are impacted wisdom teeth always a problem
Many teens receive a prescription note from their dentist referring them to an oral surgeon. On the notes lines, it may say something like, “impacted teeth”.
Wisdom teeth that don’t break through are sometimes called “impacted”. While the term “impacted” sounds bad, the teeth often don’t cause any problems.

Up to 12% of impacted teeth may lead to pain, swelling, tooth decay or inflamed gums.
To the claim, they may also push other teeth out of the way, dentist Dr. Jay W. Friedman says,
It is not possible for lower third molars, which develop in the spongy interior cancellous tissue of bone with no firm support, to push 14 other teeth with roots implanted vertically like the pegs of a picket fence so that the incisors in the middle twist and overlap. Yet that is the reason often given for removal of third molars, even though studies have produced contrary evidence. Third molars do not possess sufficient force to move other teeth. They cannot cause crowding and overlapping of the incisors, and any such association is not causation. (1, 2, 3)
Wisdom teeth that break through the gums may or may not cause problems.
My son’s story
My son’s dentist explained to me: If my son’s third molars weren’t already causing him pain, they soon would be. His wisdom teeth were impacted and would not “have enough room” to come in.
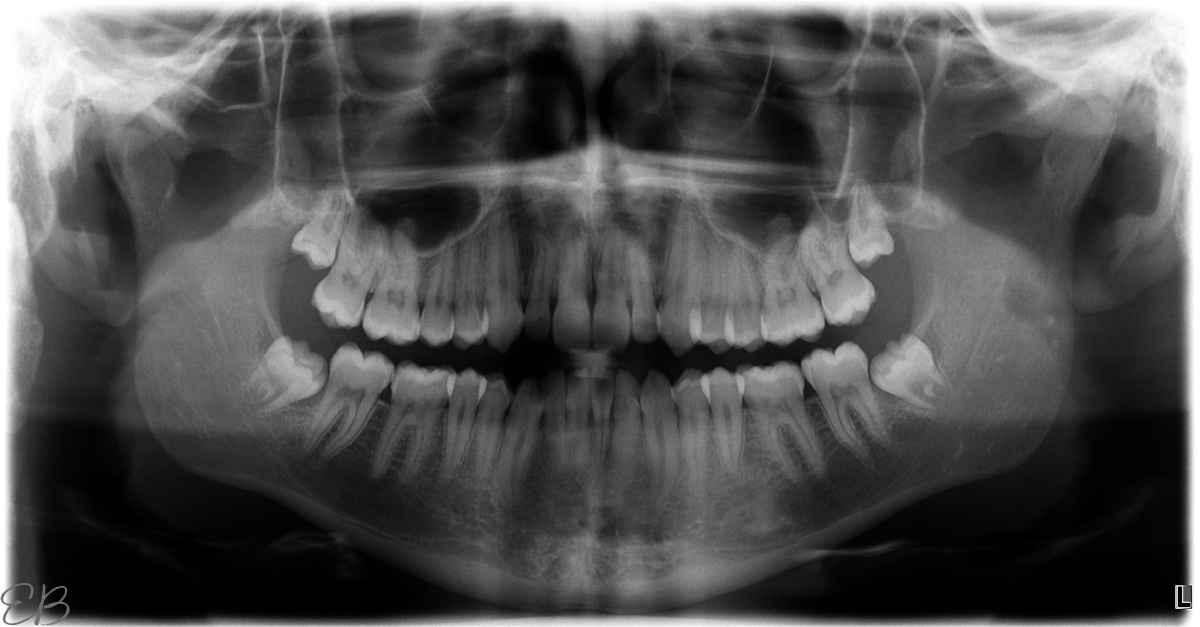
In fact, it was empowering to request to see my son’s x-ray. His wisdom teeth actually look really well placed to not cause him any issues throughout his life. (See x-ray below.) They’re coming in at good angles, and there is room in his jaw for them to stay.
While wisdom teeth breaking through the gums can be painful, our society allows babies this discomfort because it’s a necessary part of development. Pain alone is not an indicator of a serious problem.
Because health risks increase when most third molars are removed, we believe we’re wiser to avoid surgery as we “wait and see”. If no problems occur, he is part of 98% of the population that should consider the avoidance of wisdom teeth removal.
As this and other studies show, “There is no evidence of a significant increase in third-molar pathology with age“.
Third molar evidence in Europe
In Europe, where routine oral surgeries are not done, 80% of young adults have at least one wisdom tooth that hasn’t broken through.
There is no evidence of widespread wisdom teeth infection in populations where the surgery is not done — nor evidence for the medical necessity of the number of prophylactic surgeries performed in the U.S.
Only 12% of truly impacted teeth are associated with change over time, which could include problems like cysts. (source)
How often does wisdom teeth removal cause complications
Bob Jones, inventor of an ultrasound instrument designed to detect and image cavitations, reported finding cavitations in approximately 94% of several thousand wisdom teeth sites he scanned. (source)
The decayed bone ranged in size and severity but was almost always present.
More recent research by Dr. Boyd Haley showed ALL cavitation tissue samples tested contain toxins.
Wisdom teeth sites are particularly predisposed to cavitation because they contain small terminal vessels, and osteonecrosis is a disease of these vessels. If the local anesthetic used contains a vasoconstrictor (often epinephrine), it shuts down the blood supply to the bone in these areas.
Note: If you plan to have 3rd molar surgery, ask your doctor for non-vasoconstricting anesthetics.
Potential side effects of wisdom teeth removal
As a teenager, I, too, had my wisdom teeth removed. Within a few days, I got a fever and was quite sick. My common infection was called “dry socket”. (Note: Women having this procedure should time it with their menstrual cycle to decrease the likelihood of dry socket. [source])
I was treated with antibiotics and clove-saturated bandages inside the cavitations.
(I am actually grateful for the clove oil that was used, as it likely prevented future infections at the site.)
If post-surgery pain lasts longer than five days and gets worse, or leads to bad breath, swelling or fever, consult your doctor about possible complications.
Here are some complications that can occur:
- The dried blood that closes the wound comes off too soon, leaving the wound unprotected.
- Nerves and blood vessels can be damaged during the procedure.
- Temporary or permanent numbness in the lip, tongue or cheek. (source)
- Various infections in the cavitations left behind after surgery. (These testimonies are quite alarming, and I discuss them more below.)
Symptoms patients may experience include:
- severe facial pain
- neuralgia
- headaches
- very low energy
- phantom toothaches
- various symptoms related to Lyme, mold exposure, heavy metals and other infections
Unfortunately, up to 1% of all wisdom teeth surgeries can cause lasting problems and chronic infections. Many of these infections go undetected.
Patients have no idea that their chronic health issues stem back to the removal of their third molars and the ongoing quiet infection that began afterwards.
The link between cavitations and chronic illness
A cavitation is a hole in the bone that cannot be detected through just looking at it.
After third molars are removed, significant cavitations are left behind.
A disease process can begin in which the lack of blood supply to that bone results in a hole or “hollowed out” portion of the jawbone. Sometimes, the holes may spread extensively from their original locations throughout the jawbone and may penetrate the sinuses and beyond.
Recent research shows that all cavitation tissue samples tested contain toxins, and some of these produce significant systemic effects.
The jawbone becomes a holding tank for chemicals and heavy metals that allows more potent toxins to form. (source, source)
If the inside of the bone tissue does not fully heal, it presents:
- the right environment for invasive growth
- a harbor for infection
Chronic health issues from cavitations
Here are some common and serious health issues linked to cavitations:
- mold toxicity
- chronic sore throats
- sinus issues
- low functioning immune system
- Lyme disease (an infection caused by the bacterium Borrelia burgdorferi)
- other bacterial infections
- inhibition of basic body enzymes necessary in the energy production cycle
- inability to detoxify heavy metals, including mercury
- reduced glutathione levels
Regarding bacterial infections, bacteria can actually “hide out” in cavitations due to the absence of blood flow in those areas. Even during rounds of antibiotics, the bacteria have a safe harbor.
Alternatives to wisdom teeth removal
Wisdom teeth removal is a multi-billion dollar industry. Practitioners do not often look for alternatives.
But, there are safer options with fewer complications. These include:
- removal of excess tissue (the hyperculum) around the tooth
- homeopathy (see more specifics on this below)
- good oral hygiene, including tooth brushing
- the use of fulvic minerals, which heighten the benefits of good nutrition (more on this below). Dental health is often a reflection of general health. So, nutrition plays an important part in directing the eruption of teeth.
Nutrition and homeopathy for prevention

Vitamins D and K are important nutrients for dental health. Pregnant women may benefit their unborn children’s dental health by supplementing with these nutrients.
Midday sun is the best source for vitamin D. Good sources for vitamin K are butter and natto (fermented soybean paste).
While some sources also recommend high vitamin A intake for dental health, I have suffered from that advice and, as a result, vitamin A toxicity. A well-balanced diet avoids mega-doses of “super foods” or high doses of vitamins.
Fulvic minerals
Our soils have been compromised by modern farming techniques. Before that time, the earth was rich with minerals — as were the foods grown in them.
Fulvic minerals are trace soil minerals that help the body to assimilate nutrition on a cellular level.
Many years ago, when my health and energy were very low, fulvic minerals were like a gift of energy and wellness to me.
For advanced nutrition, avoid most super foods, embrace grass-finished beef (or wild game), and begin taking fulvic minerals!
You can read more about why to take fulvic acid minerals here.
Homeopathy for prevention
Homeopathy is a promising field for children’s and adults’ dental health.
Homeopathic Master Clinician Joette Calabrese recommends Calc phos 6x and Calc fluor 12x to support tooth and bone health. She says one approach is to place 4 pills in 4 ounces of water and take 1 sip (1 sip = 1 dose), 3 times per day.
Read more of her recommendations here.
Recovery from having wisdom teeth out
Biological dentists who do cavitation surgery
If you have cavitations that are causing chronic health issues, is it possible to resolve them?
Yes. Recommended treatment of cavitations includes surgical scraping of the area to remove all unhealthy bone and all pathology such as abscesses and cysts (removal of the necrotic tissue is key). This uncomfortable process is necessary, as less extreme measures can even worsen the condition. New bone regeneration is the goal after the procedure.
Bone grafts are extremely expensive, and insurance may not pay for the procedure.
Very few dentists are qualified to perform this surgery. No matter how well the surgery is performed, lack of healing and the need for re-treatment is a possibility.
Are wisdom teeth obsolete
Some believe that, like the tailbone, wisdom teeth are something our bodies no longer need.
A similar theory circulated about the appendix 20 years ago. We now know that the appendix has an important role in the body’s detoxification process and in digestion.
I suspect even the tailbone has a purpose, and of course, many scientists agree.
On a related topic, I was told to have my tonsils out when they became infected in my early 20s. I now wish I had known better.
What’s your experience been with wisdom teeth removal?
You can pin this article here:


Suzanne says
I wish I had known about Weston A Price and George E. Meinig when I was young and before my wisdom teeth were removed. At least I know about not getting a root canal.
Megan says
Hi Suzanne, yes, agreed. Thanks for mentioning the work of George E. Meinig! If any readers are interested, his book is here: https://amzn.to/2Wj16h0 My only caution about Dr. Price’s work is the dietary advice that evolved from it, to load up on vitamin A, which as I mentioned in the post, I believe is quite dangerous (and not natural to native diets even). But so glad you also mentioned the root canal issue. More reading and insight for interested readers, and so many of us are affected.
Alex says
Hello Megan,
Thank you for this post! I, too, had my wisdom teeth removed when I was 18 because the dentist determined they would lead to overcrowding and crooked teeth. I wish I hadn’t. So much medical advice these days does not look at root causes and gentle solutions to health concerns and as a result, we spend years in agony from various mounting health maladies, searching for solutions.
Megan says
Hi Alex, thanks for your comments, all so well said. Years of searching for solutions because a gentle alternative wasn’t considered. The functional medical reminder about looking for the root cause really feels overlooked with tonsils. Amazing how many are removed, and we don’t look at what’s causing the infection. Re wisdom teeth, it would be interesting for both of us (and millions of others) to get to go back and look at our xrays, the way I got to look at my sons’. We’re conditioned to take our practioners’ advice without seeing the determining factor first. I couldn’t believe how good my son’s looked after being told they needed to be removed. One benefit to our “years of agony” is how much we’re learning in the process (to leave us on a positive note).
Meaghan says
Hi, thank you for this article. After I had my wisdom teeth removed, because the dentist said there wasn’t much room and it might make my teeth crooked, I got constant infections. I went to the dentist several times and it was so expensive. And then I discovered salt water. And it worked way better than the antibiotics and was exponentially cheaper. I wish I had never had them removed. I never really trusted our dentist growing up, he would always push for expensive, unnecessary procedures for my parents but I never imagine wisdom teeth removal would be the same thing.
Megan says
Thanks for sharing, Meaghan, and I’m sorry for the misguidance you received and the difficulties since! It is so hard to discern what’s actually necessary and what falls into that category of interventions that can cause harm, especially when the procedure is presented as necessary.
Jennifer Dages says
Thank you. We are trying to make decisions about my 20 year old daughter right now. So this article is super helpful. I need to see an xray. I just look at my 17 year old’s xray and it looked exactly like the one you shared here, which leads me to believe that daughter is fine.
Megan says
Hi Jennifer, I’m glad it’s helpful, and best as you decide what’s right for her. 🙂 Thanks for sharing!
Shelby says
I have half erupted wisdom teeth (one is horizontal not great I know) but I have postural orthostatic tachycardia which to dentists isn’t a problem but even just local affects my heart terribly. Not that they care they still push it on me when I have a condition that can lead to cardiac arrest if I go under anesthesia. But no one talks about when the risks of removing the teeth outweigh the benefits. I have seen no one talk about what to do when you physically or medically cannot remove them. I am keeping them very clean flossing and brushing in between doing salt water rinses the whole nine yards. but they keep scaring me with what can happen if they aren’t removed. Never about what can happen to me if I remove them. I refuse to do it do to the risks with my condition but I keep getting the same fear mongering.
Megan says
Hi Shelby, I’m sorry. Maybe you can find a doctor who is educated in both the benefits and the risks, somewhere else in the States. I believe there may be a few. Most doctors just aren’t educated in the risks of your situation, only in the benefits of the surgery. And yes, the fear part is very disheartening. I pray you find that wise voice/source of knowledge.